NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
US Department of Health and Human Services. The Surgeon General's Call to Action to Prevent Skin Cancer. Washington (DC): Office of the Surgeon General (US); 2014.
Why We Must Act Now
Skin cancer is the most commonly diagnosed cancer in the United States, and most cases are preventable.1-3 Skin cancer greatly affects quality of life, and it can be disfiguring or even deadly.1,4-6 Medical treatment for skin cancer creates substantial health care costs for individuals, families, and the nation. The number of Americans who have had skin cancer at some point in the last three decades is estimated to be higher than the number for all other cancers combined,1,7,8 and skin cancer incidence rates have continued to increase in recent years.1,9
Each year in the United States, nearly 5 million people are treated for all skin cancers combined, with an annual cost estimated at $8.1 billion.10 Melanoma is responsible for the most deaths of all skin cancers, with nearly 9,000 people dying from it each year.11 It is also one of the most common types of cancer among U.S. adolescents and young adults.12 Annually, about $3.3 billion of skin cancer treatment costs are attributable to melanoma.10
Despite efforts to address skin cancer risk factors, such as inadequate sun protection and intentional tanning behaviors, skin cancer rates, including rates of melanoma, have continued to increase in the United States and worldwide.1,13-17 With adequate support and a unified approach, comprehensive, communitywide efforts to prevent skin cancer can work. Although such success will require a sustained commitment and coordination across diverse partners and sectors, significant reductions in illness, deaths, and health care costs related to skin cancer can be achieved.
This document is a Call to Action to partners in prevention from various sectors across the nation to address skin cancer as a major public health problem. Many partners are essential to this effort, including federal, state, tribal, local, and territorial governments; members of the business, health care, and education sectors; community, nonprofit, and faith-based organizations; and individuals and families. The goal of this document is to increase awareness of skin cancer and to call for actions to reduce its risk.
The first section describes the problem of skin cancer and its major risk factors. It also discusses the relationship between exposure to ultraviolet (UV) radiation and health. The second section describes the current evidence on preventing skin cancer, including current initiatives in the United States and in other countries. The third section describes the gaps in research related to skin cancer prevention, highlighting areas of research where more work is needed. The fourth section identifies specific opportunities to prevent skin cancer by reducing UV exposure in the U.S. population and calls for nationwide action.
This document also includes six appendices, which provide further detail about specific topics. For more information about the scope of this document and definitions of commonly used terms, see Appendix 1. Appendix 2 describes symptoms of skin cancer. Appendix 3 provides a brief discussion of skin cancer screening. Success stories in skin cancer prevention are discussed in Appendix 4, and current federal efforts on skin cancer prevention are summarized in Appendix 5. Abbreviations and acronyms are listed in Appendix 6.
Why a Focus on UV Radiation?
Although genetic factors, such as being fair-skinned or having a family history of skin cancer, contribute to a person's risk,18-24 the most common types of skin cancer (see Appendix 1) are also strongly associated with exposure to UV radiation.3,25-30 UV exposure is also the most preventable cause of skin cancer. This Call to Action focuses on reducing UV exposure, with an emphasis on addressing excessive, avoidable, or unnecessary UV exposures (such as prolonged sun exposure without adequate sun protection) and intentional exposure for the purpose of skin tanning (whether indoors using an artificial UV device or outdoors while sunbathing).
This document focuses on primary prevention of skin cancer through reducing overexposure to UV, not on early detection or screening. The evidence on skin cancer screening is growing, and ongoing examinations of the evidence are important. Melanomas diagnosed at earlier stages are much more treatable than those diagnosed at later stages.6,31 It is important for the public to understand that anyone can get skin cancer and to know the signs, which can be found in Appendix 2 and at http://www.cdc.gov/cancer/skin/basic_info/symptoms.htm. Information on screening is available in Appendix 3.
Factors other than UV exposure can increase the risk of skin cancer in certain populations. Certain uncommon genetic mutations, such as those linked to familial melanoma and xeroderma pigmentosum, can strongly increase a person's risk of melanoma.32 Occupational exposures to ionizing radiation, high doses of UV radiation, or exposure to certain chemicals during manufacturing processes may increase skin cancer risk beyond that of the general public.32 However, this document focuses on reducing the risk of skin cancer in the general U.S. population.
Sources of UV Radiation Addressed in This Document
UV radiation is a type of electromagnetic radiation emitted by the sun and from some man-made lights, with wavelengths longer than X-rays but shorter than visible light.33,34 For most people in the United States, the sun is the most common source of exposure to UV radiation. UV radiation from indoor tanning devices is a less common but more easily avoidable source of UV radiation exposure than from the sun. More information about UV radiation, including the different types, is provided in the “Exposure to UV Radiation” section (see page 11). This Call to Action discusses important steps that can be taken to reduce exposure to the most common sources of UV radiation at the population level.
UV Exposure and Overexposure
UV exposure stimulates melanocytes to produce melanin, often resulting in a tan or sunburn, both of which indicate overexposure1 and damage to the skin, skin cells, and DNA within those skin cells.35,36 The underlying biology of skin cancer risk is directly related to damage to the skin and its genetic material.37 Although all UV exposures can affect skin cancer risk, entirely avoiding UV rays from the sun is neither realistic nor advisable for most Americans. Spending time outdoors is associated with positive health benefits, such as increased levels of physical activity and improved mental health.38-40
Skin Cancer Incidence and Mortality
This document focuses on the three most common types of skin cancers: basal cell carcinoma (BCC), squamous cell carcinoma (SCC), and melanoma, which together account for more than 99% of skin cancers (Figure 1).41,42 These three types of cancer are described in greater detail in Appendix 1. BCC and SCC are the most common types of nonmelanoma skin cancers (NMSCs).

Figure 1
Types of Skin Cancer.
Nonmelanoma Skin Cancers
In the United States, information on BCC and SCC of the skin is not routinely collected in population-based central cancer registries, so information on these cancers comes from medical claims data, survey data, and special studies.2,10,43 Of the 5 million U.S. adults treated for skin cancer on average each year, an estimated 4.3 million (1.9% of the adult population) are treated for NMSCs (BCC, SCC, and other rare skin cancers), according to an analysis of the Agency for Healthcare Research and Quality's Medical Expenditure Panel Survey.10 Among those aged 65 years or older, an estimated 6.9% (9.3% of men and 5.0% of women) are treated for NMSCs on average each year.10 Medicare data for 2002–2006 showed that the number of procedures used to treat NMSCs in the Medicare population increased by 16.0% during that period.2 A special study that examined deaths from SCC and BCC in Rhode Island during 1988–2000 showed death rates of 0.29 and 0.08 per 100,000 per year for nongenital SCC and BCC; the rate for melanoma during the same period was 2.6 per 100,000.5,44
Basal Cell Carcinomas
BCCs are thought to be more common than any other type of cancer and are generally treatable.1,7 Although national rates are not available, studies have estimated BCC incidence rates in some states. For example, incidence rates for BCC during 1993–1994 in New Hampshire were 309.9 per 100,000 among men and 165.5 per 100,000 among women.45 Arizona had an estimated rate of more than 900 per 100,000 among men and nearly 500 per 100,000 among women in 1996.46 The incidence of BCC appears to be increasing at a rate of about 2% per year in the United States.1,13,47 About 70%–80% of NMSCs among males and 80%–90% of NMSCs among females are BCCs.43
Melanoma
Melanoma is the third most common type of skin cancer and is responsible for most skin cancer deaths.9,14,32 In the United States, according to federal data for 2007–2011, more than 63,000 people are diagnosed with melanoma, and nearly 9,000 people die from this disease each year (Tables 1 and 2).11,49 Although melanoma rates overall are highest among older adults, it is the third most common cancer in adolescents and young adults (aged 15–39 years).12 Recent analyses have found increases in incidence across all tumor thicknesses and stages.9 If current trends in cancer death rates continue, melanoma will be the only cancer objective included in Healthy People 2020 that will not meet the targets for reductions in cancer deaths (http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicId=5).50,51
Table 1
Invasive Melanoma Incidence, by Sex and Race/Ethnicity, United States, 2007–2011,.
Table 2
Melanoma Death Rates, by Sex and Race/Ethnicity, United States, 2006–2010,.
Variation by Sex
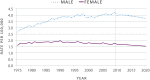
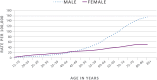
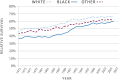
In 2011, melanoma of the skin was the fifth most common cancer for men, with an incidence rate of 25.4 cases per 100,000 (31.0 for white men, the group with the highest rates) and the seventh most common cancer for women, with an incidence rate of 15.7 per 100,000 (20.1 for white women).52 During 2002–2011, melanoma incidence increased at an average annual rate of 1.6% for men and 1.5% for women.52 This increase is the largest increase of the 10 most common cancers among men, and it is surpassed only by increases in thyroid cancer among women (Figure 2).51,52 Although incidence rates for melanoma are increasing among both males and females (Figure 3), melanoma death rates are only increasing among males (Figure 4).9,14,51
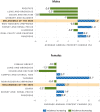
Figure 2
Average Annual Percent Change in the 10 Most Common Cancers, 2002–2011. Abbreviation: NOS, Not Otherwise Specified.
Melanoma incidence and death rates are highest among males, especially non-Hispanic white males (Tables 1 and 2 and Figures 3, 4, and 5).50 Increased risk of melanoma in white males may be related to a variety of factors, including skin type and historical differences in sun exposure and sun protection behaviors. White men aged 65 years or older have the highest incidence (130.1 cases per 100,000) and death rates (23.7 per 100,000) for melanoma.9,12
Variation by Anatomic Site
Melanoma is found more often on parts of the skin that get more intermittent, intense UV exposure, such as the torso and legs, although patterns vary by age.32,53 In addition, the anatomic distribution of melanoma varies by sex, most often occurring on the legs for females and on the torso for males.32 Recent research suggests that melanomas among young women may be particularly increasing on the torso.54 However, these patterns are complex and vary among populations.55 Because acral melanoma (which occurs on palms of hands and soles of feet) arises in typically unexposed areas of the body, the role of UV exposure in this cancer is thought to be limited, and acral melanoma may have different risk factors than other types of cutaneous melanoma.56,57
Variation by State
State incidence rates for melanoma among all races vary widely, from 11.9 per 100,000 in Alaska to 31.9 per 100,000 in Utah during 2007–2011.49 Reasons for state variations include differences in populations by race, age, and genetic background; by socioeconomic status (SES) and health care access; and by patterns of UV radiation and exposure, as well as differences in collection of data on melanomas by state central cancer registries.53 Much of the variation in state rates is because of differences in state populations. Among non-Hispanic whites, the population at highest risk, higher UV levels are associated with higher melanoma incidence rates; for this population group, Alaska has the lowest melanoma rate of all states (14.8 per 100,000), and Hawaii has the highest melanoma rate of all states (66.7 per 100,000).49,58 States in southern latitudes have the highest death rates for melanoma among non-Hispanic white populations.52,59
Survival
The prognosis for patients with metastatic melanoma remains poor, but has been improving because of recent advances in treatment.60-62 Survival is poorest among black populations, possibly because of later diagnoses and lower perceived risk, and because these populations are disproportionately diagnosed with certain types of melanoma with poorer survival rates (acral lentiginous melanoma) (Figure 6).6,63,64
Economic Burden of Skin Cancer
In addition to causing illness and death, skin cancer is costly to the nation. Skin cancer treatment is estimated to cost about $8.1 billion in the United States each year, $4.8 billion of which is for NMSC and $3.3 billion of which is for melanoma.10 Several new medications are available for skin cancer, which increases treatment options but could also lead to higher costs.65-67
Skin cancer also results in significant costs beyond those related to treatment. Annual costs associated with lost workdays and restricted-activity days are estimated at $76.8 million for NMSC and $29.4 million for melanoma.68,69 An individual in the United States dying from melanoma loses an average of 20.4 years of potential life, compared with an average of 16.6 years for all malignant cancers.70 Annual productivity losses associated with these lost years is estimated to cost an additional $4.5 billion ($3.5 billion attributed to melanoma deaths and $1.0 billion attributed to NMSC deaths).69,70
Risk Factors for Skin Cancer
Genetic Factors
People with certain genetic risk factors are more likely than others to develop skin cancer. Genetic risk factors for skin cancer include having a lighter natural skin color; blue or green eyes; blond or red hair; dysplastic nevi (a type of unusual mole) or a large number of common moles; and skin that burns, freckles, or reddens easily or becomes painful after excessive time spent in the sun.18,24 People with red hair may be at particularly increased risk of melanoma.24 In addition, those with a family history or personal history of skin cancer, especially melanoma, are at increased risk.18-23
Skin Type
Skin cancer risk varies by skin type, which is classified by how likely a person is to tan or burn. The six skin types of the Fitzpatrick skin type classification system are shown in Table 3.71 Sunburn often is used as a proxy outcome measure in skin cancer prevention studies because it takes into account the person's skin type, as well as the intensity and duration of UV exposure. Although anyone's skin can be damaged by UV exposure, people with skin types I and II are at the highest risk of burns, damage from UV radiation, and skin cancer.
Table 3
Fitzpatrick Skin Type.
Originally, the Fitzpatrick system was constructed for white populations and had only four categories (Skin Types I–IV). Types V and VI were added to the system later in recognition of the wide variety of races and skin types.71 Because the Fitzpatrick system was developed to measure the skin types of whites, the terminology used may make it difficult for blacks or other races to classify their skin type.72 Although the Fitzpatrick system is often considered the gold standard for categorizing skin type, it may not always accurately reflect an indvidual's risk of skin cancer, and other systems have been proposed.73,74
Race and Ethnicity
Race and ethnicity play an important role in skin cancer risk because characteristics associated with race and ethnicity (such as skin, hair, and eye color) are indicators of melanoma risk. Blacks and Asians/Pacific Islanders have the lowest melanoma incidence and death rates, followed by American Indians/Alaska Natives and Hispanics (Tables 1 and 2). People of European descent and non-Hispanic whites have the highest melanoma incidence and death rates because they generally have lighter natural skin color.32,53
However, race and skin type do not always align neatly, and wide genetic variation exists within races.75,76 People who identify as being other than non-Hispanic white may still be at higher risk of skin cancer because of their skin type and may underestimate their risk.63,64,77-79 Some black Americans report being sensitive to the sun.80 Recent data showed low reported use of sun protection behaviors among Hispanics, and melanoma may be increasing among some Hispanic groups.77,81
Exposure to UV Radiation
Although genetic risk factors contribute to a person's skin cancer risk, most skin cancers are believed to be caused by a combination of genetic factors and exposure to UV radiation, from the sun and from artificial sources such as indoor tanning. By reducing intentional UV exposure and increasing sun protection, many skin cancer cases can be prevented.
Types of UV Radiation
Sunlight is made up of different types of electromagnetic radiation, mostly infrared, visible, and UV. Exposure to sunlight has both positive and negative effects. Although sun exposure can have positive effects on mood and stimulates production of vitamin D, exposure to UV radiation also damages DNA and cell functions, and that damage can lead to cancer. UV radiation is categorized into three types: UVA (UV radiation with a wavelength of 315 nm to 400 nm), UVB (280 nm to 315 nm), and UVC2 (100 nm to 280 nm).33,34
UVB radiation has intermediate levels of energy and can cause sunburn and direct DNA damage (Figure 7). Ozone and other components of the atmosphere absorb more than 90% of UVB from the sun, but the amount absorbed varies widely depending on time, location, season, and weather. Certain chemical and carbon emissions also have caused depletions in stratospheric ozone since the 1970s, and evidence suggests that this decrease has led to an increase in ground-level UVB levels.82,83 Further study is needed to determine whether ozone depletion is contributing to the increasing incidence of skin cancers worldwide.82-85 UVA radiation has less energy than UVB radiation, but it can also cause skin cancer and other skin damage. Unlike UVB radiation, nearly all UVA radiation passes through the atmosphere, and it penetrates to deeper layers of the skin than UVB radiation.
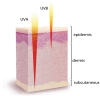
Figure 7
Types of Ultraviolet (UV) Radiation and Skin Penetration. Note: UVC radiation (not shown) is almost completely absorbed by the earth's atmosphere and does not generally affect human skin.
U.S. Environmental Protection Agency's UV Index
The UV Index developed by the U.S. Environmental Protection Agency (EPA) provides daily and hourly forecasts of the expected risk of overexposure to UV radiation from the sun. The UV Index scale describes how to use the UV Index to help avoid harmful exposure to UV radiation, with a lower UV Index indicating a lower risk on a scale of 0–11 (Table 4). In winter, the average UV Index is 2 or below, although it can be higher on some days. During November–January, the daily average for the UV Index is usually 2 or below nearly everywhere in the United States except Florida and Hawaii (http://www2.epa.gov/sunwise/monthly-average-uv-index). However, reflective surfaces, such as snow, water, and sand, and high altitudes can increase risk of overexposure to UV radiation and sunburn. EPA recommends that people use more sun protection strategies as UV levels get higher. For specific recommendations for sun protection at different UV levels, visit http://www2.epa.gov/sunwise/uv-index-scale.
Table 4
Ultraviolet (UV) Index Levels.
UV Exposure and Skin Cancer
Many skin cancers can be avoided by reducing exposure to UV radiation.3,25-30 As many as 90% of melanomas are estimated to be caused by UV exposure.25,86 Some evidence suggests that certain rare skin cancers, such as Merkel cell carcinoma, a rare but frequently fatal cancer arising from neuroendocrine cells, may also be related to UV exposure.41,42 The degree to which UV exposure increases a person's risk of skin cancer depends on many factors, such as individual skin type, the amount and types of sun protection used, whether exposure is chronic or intermittent, and the age at which the exposure occurs.15,86-92
Ecologic studies have shown that light-skinned people who live in areas with higher UV exposure, particularly when they are younger, have higher rates of skin cancer, especially SCC.85,88,93 Similarly, melanoma is thought to be caused by sun exposure throughout life, possibly with stronger effects in early life, although adult exposures clearly increase risk as well.87 Some studies suggest that UV exposures in childhood that do not result in a burn may be associated with lower rates of future melanomas.94,95 Melanoma incidence is also associated with higher SES, which is a combination of education, income, and wealth. This association is likely due to the relationship between SES and other risk factors, such as skin type and patterns of UV exposure.32,78 When people with lower SES are diagnosed with melanoma, they tend to have poorer outcomes, probably because of later detection and poor access to treatment.6,32,96,97 See Table 5 for a comparison of avoidable risk factors for skin cancer.
Table 5
Excess Health Risks Associated with Ultraviolet (UV) Exposure, by Type of Skin Cancer and Type of UV Exposure.
Chronic Versus Intermittent UV Exposure
The effects of some risk factors are different for different types of skin cancers. Chronic exposure is defined in different ways in the literature, but usually refers to frequent, extended outdoor exposures to UV radiation from the sun above a certain number of times a week or a certain number of days a year.43,87,90,95,98-103 Studies of chronic exposure usually do not include short frequent exposures, such as those experienced by the average person in his or her commute to work or school. Extended or intense exposures experienced only a few times a year, such as the sun exposure received on a trip to the beach, are typically classified as intermittent exposures. Continuous, chronic UV exposure, such as that observed among outdoor workers, is more strongly associated with SCC, while intermittent or recreational exposure is more strongly associated with melanoma and BCC.43,87,95,99-103
Sunburn is a clear sign of overexposure to UV, and it typically occurs after intermittent exposure; sunburn at any age increases a person's risk of skin cancer.9,43,87,99,100 Indoor workers may receive a substantial proportion of their total UV radiation from intermittent exposure.104-106 Cumulative exposure to UVA through glass windows, which block most UVB, can also cause skin damage over time.107,108
Outdoor Workers
Although research clearly indicates that outdoor workers are at increased risk of BCC and SCC, some studies suggest that outdoor workers might not have an increased risk of melanoma, or that they may even have a lower risk than indoor workers.43,109-111 When stratified by UV level, outdoor workers in UV-intense areas do appear to be at increased risk of melanoma.55,103 Studies of melanoma risk and outdoor work may be limited by lack of information on other related factors, which then limit the ability to attribute effects to the relationship between outdoor work and melanoma.15,91 Regardless of these potential study limitations, outdoor workers often experience excessive UV exposure on the job, and efforts are needed to ensure that outdoor workers are protected from the sun.
Indoor Tanning
Indoor tanning devices, such as tanning beds, tanning booths, and sun lamps, expose users to intense UV radiation as a way to tan the skin for cosmetic reasons. Although reducing UV overexposure from the sun can be challenging for some people, UV exposure from indoor tanning is completely avoidable. In 2009, the World Health Organization (WHO) classified indoor tanning devices as Class I human carcinogens on the basis of strong evidence linking indoor tanning to increased risk of skin cancer.27,112 Meta-analyses have consistently shown that indoor tanning increases the risk of developing SCC, BCC, and melanoma (Table 5).27,113-121 The risk increases the more an individual uses indoor tanning, with younger and more frequent users having more steeply increased risk.113-121
Findings consistently document a strong association between increased risk of melanoma and indoor tanning use, although the magnitude of the association varies from study to study, reflecting different populations and settings. A recent international meta-analysis that included 31 studies collectively reviewing 14,956 melanoma cases and 233,106 controls (individuals without melanoma) reported that individuals who reported ever indoor tanning had a 16% increased risk of melanoma over those who never indoor tanned.121 The association between indoor tanning and melanoma increased when analysis was restricted to more recent studies conducted in 2000 or later (22%) or when restricted to individuals who had used indoor tanning devices 10 or more times in their lives (34%).121 When analysis was restricted to the 11 studies from North America, including 4,395 melanoma cases and 79,358 controls, the increased risk of melanoma with ever using indoor tanning was 23%.121 In one U.S. study included in the meta-analysis, researchers reported a 74% increased risk of melanoma among individuals who reported ever using indoor tanning compared with those who did not tan.116 Findings from this study also reported a strong dose-response relationship, with greater risk for more sessions, hours, or years spent tanning.116
Indoor tanning also increases the risk of BCC and SCC.122,123 For NMSCs, indoor tanning was found to increase risk of BCC by 29% and of SCC by 67%.120 A 2014 meta-analysis estimated that more than 400,000 cases of skin cancer may be related to indoor tanning in the United States each year: 245,000 BCCs, 168,000 SCCs, and 6,000 melanomas.124
Initiating indoor tanning at younger ages appears to be more strongly related to lifetime skin cancer risk, possibly because of the accumulation of exposure over time from more years of tanning.114,116,118,119 The magnitude of increased risk with younger age at initiation varies because of differences in collection and reporting of data, but studies consistently show an increase in risk. A frequently cited meta-analysis estimated that tanning before age 35 increased risk by 59%.118,119 This risk estimate is based on a compilation of data from U.S. and international studies from different settings.118,119 One 2010 U.S. study found that ever using indoor tanning before age 18 increased risk of melanoma by 85% compared with never indoor tanning; risk for those aged 18–24 years increased by 91%.116 Years of use of tanning devices appeared to be the strongest predictor of increased risk in this study, with increased risk of 47% with 1 year of indoor tanning, 64% with 2–5 years of indoor tanning, 85% with 6–9 years of indoor tanning, and 145% with 10 or more years of indoor tanning.116 Harms of indoor tanning may be accelerated for adolescents and young adults, leading to early-onset skin cancers.115,125,126
Although earlier studies describing the association between indoor tanning and skin cancer had been criticized for not accounting for skin type and outdoor UV exposure or sunburns,127 more recent studies have controlled for these factors, and these studies have also found that indoor tanning increases the risk of melanoma.116,125,128-131 For example, a 2014 study showed that individuals who tanned indoors without burning had an increased risk of skin cancer, regardless of lifetime sunburns experienced.128
According to 2013 Youth Risk Behavior Survey (YRBS) data from the Centers for Disease Control and Prevention (CDC), about 13% of high school students, 20% of high school girls, and 27% of girls in the 12th grade had used an indoor tanning device, such as a sunlamp, sunbed, or tanning booth (not including a spray-on tan), one or more times during the previous 12 months.132 Results from CDC's 2010 National Health Interview Survey (NHIS) show that some groups of young adults had high rates of indoor tanning, specifically non-Hispanic, white women aged 18–21 years (32%) and 22–25 years (30%). Among non-Hispanic, white indoor tanners, 58% of women and 40% of men did so 10 or more times during the 12 months before the survey.133 A study that combined data from the YRBS and NHIS reported that about one-third of non-Hispanic white women aged 16–25 tanned indoors each year.134
No evidence exists to suggest that indoor tanning is safer than tanning outdoors or confers any substantial protection from future sun exposure. Studies have found that indoor tanning exposes users to excessive levels of UV radiation, especially UVA.135-138 The average intensity of artificial UV radiation was found to correspond to a UV Index of 13 or 14 (extreme), with some devices measuring even higher.135,136 Some studies have found that tanning devices may expose users to 4–13 times the amount of UVA as exposure from summer noontime sun in the District of Columbia, depending on the type of device used.136,138 In studies examining the relationship between UV exposure and skin cancer risk, indoor tanning is typically classified as intermittent UV exposure (similar to outdoor recreational exposure) rather than chronic exposure because of the acute intensity of the exposure.90,98 An estimated 3,200 people a year in the United States seek care in emergency rooms with injuries attributed to indoor tanning.139 In addition to increasing skin cancer risk, indoor tanning can cause burns to the skin, acute and chronic eye diseases if eye protection is not used, and, if tanning devices are not properly sanitized, skin infections.139-141
Other Harms Caused by Excessive UV Exposure
In addition to increasing the risk of skin cancer, UV exposure can have adverse effects on the skin, eyes, and immune system. Excessive UV exposure can damage the immune system; cause premature skin aging, including wrinkling, mottled pigmentation, and loss of elasticity; and increase the risk of actinic keratoses, which can progress to SCC.86,113,142,143 Excessive UV exposure may reduce the effectiveness of folic acid supplements, which has potential health consequences for pregnant women and women of childbearing age.144
Excessive UV exposure can also damage the eye, affecting surface tissues and internal structures, such as the cornea and lens. Unprotected exposure to excessive UV radiation can cause photokeratitis (sunburn of the eye).145 Chronic exposure to UV radiation can lead to skin cancer around the eyelids (BCC, SCC, and melanoma), as well as cataracts, conjunctival cancers, pterygium (abnormal, noncancerous growth in the corner of the eye that can extend to the cornea and partially block vision), age-related macular degeneration, and possibly ocular melanoma (melanoma of the eye).145 Wearing sunglasses that fit properly and have 100% UVA and UVB protection is the best way to protect eyes from UV damage.146,147
Complex Relationship Between Outdoor UV Exposure, Vitamin D, and Human Health
As well as being a carcinogen, UV radiation can affect other aspects of human health.148,149 UV exposure can stimulate production of vitamin D in the skin, a vitamin important for bone health and associated with other health outcomes.150-152 Complete avoidance of sun exposure may put bone health at risk, although too much exposure increases risk of skin cancers and eye disease (Figure 8).82,86,142 UV radiation is sometimes used as a medical treatment for certain skin or bone ailments.153 Many people engage in regular physical activity outdoors, which can lead to UV radiation overexposure if appropriate sun protection is not used (see the “Reducing the Risk of Skin Cancer” section on page 23 for a discussion of sun protection methods). Some have also suggested that UV exposure may have benefits for heart health by reducing blood pressure, but the evidence is still evolving.154,155 The following sections summarize the current evidence on UV exposure, vitamin D, and other health benefits.
Vitamin D
The health benefits of sun exposure are often framed within the context of vitamin D production. Vitamin D is essential for human health and is synthesized by the skin after exposure to sunlight.150,151,156 Although the scientific literature has established vitamin D as an important component of bone health,151,152,157 substantial research has also been devoted to the role of vitamin D in the prevention of numerous chronic diseases, including autoimmune conditions, obesity, diabetes, high blood pressure, heart disease, preterm birth, certain types of cancer, and all-cause mortality.155,158-165 The results of this research are primarily based on ecologic studies and are conflicting.151,160,166-170 Some have speculated that low vitamin D concentrations may be a result of ill health, rather than a cause.166,171,172
In 2010, the Institute of Medicine (IOM) published a report examining dietary reference intakes and optimal serum 25-hydroxyvitamin D (25OHD) concentrations.3,151 During 2001–2006, roughly one-quarter of the U.S. population had serum 25OHD values that put them at risk of inadequacy, 8% were at risk of deficiency, and 1% had a high serum 25OHD value that may possibly be harmful.172 Optimal concentrations of serum 25OHD may vary among individuals.173 Blacks have the lowest 25OHD concentrations compared with other racial and ethnic groups.156,172 Lower concentrations of vitamin D-binding proteins among blacks may provide more bioavailable vitamin D, potentially explaining the paradox of frequently diagnosed deficiency among U.S. black populations, who also tend to have better bone health than whites.156,174,175
Although maternal concentrations of vitamin D and incidental sunlight exposure are sufficient for most breastfed infants, some can be at risk of vitamin D deficiency if adequate vitamin D is not obtained from another source, such as a supplement. The American Academy of Pediatrics recommends a supplement of 400 IU/day for infants and children not consuming enough vitamin D-fortified formula or milk to provide the recommended daily amount of vitamin D.176,177

The amount of outdoor sun exposure needed for meaningful vitamin D production depends on many factors, including time of day, time of year, latitude, altitude, weather conditions, a person's skin type, amount of skin exposed to the sun, other individual circumstances, and reflective surfaces, such as snow, water, and sand. According to WHO, 5 to 15 minutes of casual sun exposure on face, arms, and hands 2 to 3 days a week in the summer can sustain adequate concentrations of vitamin D in most people.142 However, those with dark skin may require 3 to 6 times the amount of sun exposure as those with light or fair skin.142,178,179 Because the skin of a person with fair complexion is less able to produce a tanning response,180 the amount of sun exposure needed for a fair-skinned person to get a tan either indoors or outdoors, even before sunburn, exceeds levels of exposure needed to synthesize vitamin D.135-137,181 In the winter months in northern latitudes, exposure to sunlight does not result in meaningful cutaneous vitamin D synthesis.151
Because the U.S. population contains wide variations in skin tone, and because our nation covers a wide array of latitudes and geographic conditions, populationwide recommendations for obtaining vitamin D from sunlight would likely result in too little vitamin D in some groups and too much sun exposure in other groups because no known threshold of UV exposure exists that does not also increase skin cancer risk.182 Exceeding limited levels of exposure is not advisable because the skin can only produce a finite level of vitamin D, and increases in UV exposure are not proportional to increases in serum vitamin D concentrations.183-185
For individuals and populations who avoid all sun exposure, a dietary source of vitamin D is necessary to maintain vitamin D status.186 Although complete sun avoidance can result in vitamin D deficiency, evidence to date does not suggest that sunscreen use causes vitamin D deficiencies. In 2001, the U.S. Food and Drug Administration (FDA) reviewed seven clinical studies that examined the effect of sunscreen use on vitamin D concentrations and determined that the studies failed to show that sunscreen use caused vitamin D deficiencies.187 Adequate vitamin D can be obtained safely through food and dietary supplements without the risks associated with overexposure to UV radiation.150,151 Research suggests that most people get the majority of the total vitamin D they need from food rather than from the sun.188
DIETARY SOURCES OF VITAMIN D
The best natural sources of vitamin D in the diet include fatty fish (such as salmon, tuna, mackerel, sardines, and catfish) and fish liver oils.173 Small amounts of vitamin D are also found in egg yolks, beef liver, some mushrooms, ricotta cheese, and some cuts of pork. Vitamin D-fortified foods and beverages provide most of the vitamin D in the U.S. diet. Almost all of the milk in the United States is fortified with vitamin D, and many of the ready-to-eat breakfast cereals provide a small amount of added vitamin D. In addition, specific brands of soy beverages, orange juice, yogurt, margarine, and other foods are also fortified with vitamin D.189
Medical Uses of UV Exposure
Dermatologists and other doctors sometimes use UV light to treat health conditions, such as psoriasis, rickets, and eczema. These providers are advised to carefully weigh the risks and benefits of UV treatment for individual patients and carefully monitor doses.153,190-196
Benefits of Being Outdoors
Beyond the benefits directly attributable to UV exposure, spending time in outdoor environments may also have positive effects on physical and mental health, including higher levels of physical activity and positive effects on overall health and sense of well-being.38-40 These benefits can be achieved while using adequate sun protection, including shade, protective clothing, and broad spectrum sunscreen with a sun protection factor (SPF) of 15 or higher to reduce skin cancer risk.38-40,197-199 Features like shade trees can make spaces more attractive and provide protection from the sun and heat. In turn, perceived availability and “greenness” of spaces are associated with increased physical activity and better mental and physical health.200-202 The presence of shade in play spaces for children increases the use of the play space and children's activity levels.203,204 Thus, changes to outdoor environments can increase both physical activity and sun protection, aligning important public health goals.
Risks of Indoor Tanning Outweigh Any Potential Benefits
The benefits to limited UV exposure when outdoors do not extend to indoor tanning.205 UV exposure from indoor tanning is particularly intense, the type and intensity of UV emitted varies between devices, and exposures often exceed limits recommended by FDA or by states.135-138 Some tanning lamps emit primarily UVA, which tans the skin but does not induce vitamin D production or provide even the minimal photoprotection that a UVB-induced tan provides.150,206,207 Some tanning lamps do emit UVB, but studies suggest that vitamin D production is limited and plateaus after brief exposures, so that the amount of UV radiation needed to tan generally exceeds levels needed for adequate vitamin D production.183,208 Indoor tanning does not appear to be protective against cancer or all-cause mortality. A recent study found that indoor tanning was not associated with reduced risks of internal cancer.209 In addition, a large Swedish cohort study found that, although outdoor UV exposure was associated with reductions in all-cause mortality, exposure to artificial UV radiation from indoor tanning was associated with increased mortality.210
Some people associate tanned skin with attractiveness and health. Some also believe that a tan provides protection from future UV exposure and sunburn (often referred to as a “base tan”).211,212 Tanning is the skin's acute response to damage from UV rays.213-215 A UVB-induced tan provides minimal sun protection, equivalent to an SPF of about 3, and thus does not provide adequate protection against future UV exposure.216,217 Belief in the protection of a “base tan” may lead to a false sense of security and inadequate use of sun protection while outdoors in the sun.212 Some studies have found that indoor tanning does not protect against sunburn.212,218 People who engage in indoor tanning before going on vacation may be more likely to stay out longer in the sun, putting themselves at greater risk of sunburn.212

Low levels of sunlight in the winter months may contribute to seasonal affective disorder (SAD),219 and as a result, some indoor tanners may attempt to self-treat SAD with UV exposure through indoor tanning.220,221 Medical treatment of SAD frequently incorporates light treatment, but UV wavelengths are not generally recommended (although some lights used in treatment of SAD may contain small amounts of UVA and UVB).153,219,222 In addition, light is thought to affect SAD through the retina, not the skin.219
Current Trends in Sun Protection, Sunburn, and Indoor Tanning
Data on behaviors related to skin cancer risk among the U.S. population are collected by CDC through the national YRBS and NHIS. The national YRBS is a cross-sectional, school-based, biennial survey that monitors the prevalence of health risk behaviors among high school students. It is a nationally representative survey of students in grades 9–12 attending public and private schools.223 This survey includes questions about using sunscreen with an SPF of 15 or higher and indoor tanning. The NHIS is an annual, cross-sectional, nationally representative survey of the civilian, noninstitutionalized U.S. population.224 Interviews are conducted, mainly in person, with adults aged 18 years or older in each household, with follow-up interviews by telephone when necessary.
A periodic cancer control supplement to the NHIS includes questions about outdoor sun-protective behaviors (staying in the shade, wearing a wide-brimmed hat, wearing a long-sleeved shirt, wearing long clothing to the ankles, and using sunscreen with an SPF of 15 or higher), indoor tanning, sunburn, and sun sensitivity. This supplement is sponsored by CDC's Division of Cancer Prevention and Control and the National Cancer Institute (NCI) in the National Institutes of Health (NIH).
According to YRBS data, sunscreen use is low among U.S. high school students, with only 10.1% using sunscreen with an SPF of 15 or higher always or most of the time when outside for more than 1 hour on a sunny day. Sunscreen use is higher among high school girls (13.2%) than boys (6.9%) and higher among non-Hispanic whites (11.5%) compared with non-Hispanic blacks (4.7%) and Hispanics (7.9%). During 1999–2011, a significant linear decrease occurred in the prevalence of routine sunscreen use (from 13.3% to 10.8%). However, prevalence of sunscreen use remained stable from 2011 (10.8%) to 2013 (10.1%).132,225
NHIS data from 2010 indicate that use of sun protection was also low among U.S. adults and that about 37% of adults had been sunburned in the past year.226 Sunburn4 rates were even higher among adults aged 18–29 years and sun-sensitive groups (defined as those who burn repeatedly and freckle). Half of all Americans in this age group (about 65% of non-Hispanic whites, 10% of non-Hispanic blacks, and 35% of Hispanics) reported having had a sunburn in the past year.227 Although NHIS data indicate that some sun protection behaviors have increased among young adults over the past decade (including use of shade, use of sunscreen with an SPF of 15 or higher, and wearing of long clothing to the ankles), a corresponding decrease in sunburn has not been reported.227
Indoor Tanning
According to 2013 YRBS data, 13% of high school students had used an indoor tanning device, such as a sunlamp, sunbed, or tanning booth (not including a spray-on tan) one or more times during the previous 12 months.132 The prevalence of indoor tanning was higher among female, older, and non-Hispanic white students, with the highest prevalence among 12th-grade females (27.2%), and among non-Hispanic white females (30.7%). During 2009–2013, a significant linear decrease occurred overall in the prevalence of indoor tanning device use (from 15.6% to 12.8%). The prevalence of indoor tanning device use did not change significantly from 2011 (13.3%) to 2013 (12.8%). Data from the 2013 YRBS indicate that among students who engaged in indoor tanning, frequent sessions were common, with more than half reporting frequent use (10 or more times during the previous 12 months).132
Results from the 2010 NHIS show that 6% of adults aged 18 years or older had engaged in indoor tanning in the past year.133 The prevalence of indoor tanning was higher among females (9%) than males (2%) and among younger adults than older adults, with the highest use among adults aged 18–21 years (12%), 22–25 years (12%), and 26–29 years (9%). Similar to the data for U.S. high school students, rates were higher among non-Hispanic whites (8%) than among non-Hispanic blacks (<1%) and Hispanics (2%). Certain demographic groups had high rates of indoor tanning, including non-Hispanic white women aged 18–21 years (32%) and 22–25 years (30%). Among non-Hispanic white indoor tanners, 58% of women and 40% of men did so 10 or more times during the 12 months before the survey.133
Footnotes
- 1
See Appendix 1 for a definition and discussion of overexposure and for definitions of different types of UV exposure.
- 2
Although UVC radiation has the highest energy of the three, it is almost completely absorbed by the earth's atmosphere and is not responsible for cancer in the general population.
- 3
The IOM report states that people with serum 25OHD levels of below 30 nmol/L (12 ng/mL) are at risk of deficiency relative to bone health and that serum 25OHD levels of 50 nmol/L (20ng/mL) or higher are sufficient. It expresses concern for values above 125 nmol/L (50 ng/mL).
- 4
The NHIS defines sunburn as even a small part of the skin turning red or hurting for 12 hours or longer. This definition is only given to respondents who request more information about what is meant by sunburn.
- Skin Cancer as a Major Public Health Problem - The Surgeon General's Call to Act...Skin Cancer as a Major Public Health Problem - The Surgeon General's Call to Action to Prevent Skin Cancer
- Electrolytes - Diet and HealthElectrolytes - Diet and Health
- LINC03026 long intergenic non-protein coding RNA 3026 [Homo sapiens]LINC03026 long intergenic non-protein coding RNA 3026 [Homo sapiens]Gene ID:102724156Gene
- Madame Curie Bioscience DatabaseMadame Curie Bioscience Database
- Homocystinuria Caused by Cystathionine Beta-Synthase Deficiency - GeneReviews®Homocystinuria Caused by Cystathionine Beta-Synthase Deficiency - GeneReviews®
Your browsing activity is empty.
Activity recording is turned off.
See more...