Details of Typical Clinical Findings in NF2
Vestibular schwannoma. Initial symptoms include tinnitus, hearing loss, and balance dysfunction. Onset of disability is usually insidious, although occasionally hearing loss may occur suddenly, presumably as a result of vascular compromise by the tumor. Affected individuals often report difficulty in using the telephone in one ear or unsteadiness when walking at night or on uneven ground.
With time, vestibular tumors extend medially into the cerebellar pontine angle and, if left untreated, cause compression of the brain stem and hydrocephalus. Significant facial palsy is rare even in individuals with large vestibular schwannomas.
Schwannomas may also develop on other cranial and peripheral nerves, with sensory nerves more frequently affected than motor nerves.
Children and young adults with an apparently isolated vestibular or other cranial nerve schwannoma should be considered at risk for de novo and often mosaic NF2 [Pathmanaban et al 2017].
Spinal tumors. At least two thirds of individuals with NF2 develop spinal tumors, which are often the most devastating and difficult tumors to manage [Dow et al 2005]. The most common spinal tumors are schwannomas, which usually originate within the intravertebral canal on the dorsal root and extend both medially and laterally, taking the shape of a "dumbbell." Intramedullary tumors of the spinal cord, such as astrocytoma and ependymoma, occur in 5% to 33% of individuals with NF2. Most persons with spinal cord involvement have multiple tumors. Although multiple tumors are often present on imaging studies, they remain asymptomatic in many individuals.
Meningioma. Approximately half of individuals with NF2 have meningiomas in cross-sectional studies [Goutagny & Kalamarides 2010]; however, lifetime risk may approach 80% [Smith et al 2011]. Most are intracranial, although spinal meningiomas occur. NF2 meningiomas tend to occur less frequently in the skull base than supratentorially and are usually of the fibroblastic variety [Evans et al 2000, Kros et al 2001]. Meningiomas in the orbit may compress the optic nerve and result in visual loss. Those at the skull base may cause cranial neuropathy, brain stem compression, and hydrocephalus.
See Genotype-Phenotype Correlations.
Ocular involvement. One third of individuals with NF2 have decreased visual acuity in one or both eyes. Posterior subcapsular lens opacity – rarely progressing to a visually significant cataract – is the most common ocular finding. Lens opacities may appear prior to the onset of symptoms of vestibular schwannoma and can be seen in children.
Retinal hamartoma and epiretinal membrane are seen in up to one third of individuals. Rarely, other ocular manifestations may occur; persistent hyperplastic primary vitreous has been reported in a father and son [Nguyen et al 2005]. In adulthood, particular issues with the cornea can occur, especially after surgery, resulting in the loss of facial, trigeminal, and intermedius nerve function.
Intracranial and intraorbital tumors may result in decreased visual acuity and diplopia.
Mono- and polyneuropathy. A recognized feature of NF2 is a mononeuropathy occurring particularly in childhood [Evans et al 1999] and frequently presenting as a facial palsy that usually only partially recovers, a squint (third nerve palsy), or a foot or hand drop. The foot drop may mimic polio.
A progressive polyneuropathy of adulthood not directly related to tumor masses is also recognized [Sperfeld et al 2002].
Further evidence for the mononeuropathy of childhood and the polyneuropathy of adulthood has come from sural nerve biopsies [Hagel et al 2002].
Other. Renal vascular disease similar to that occurring in neurofibromatosis type 1 (NF1) has been reported once [Cordeiro et al 2006] but is probably coincidental, as it has not been reported again. However, renal disease does occur with use of bevacizumab (see Targeted Therapy).
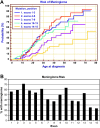
Prognosis. Variable expressivity of NF2 among individuals results in varying size, location, and number of tumors. Although these tumors are not malignant, their anatomic location and multiplicity lead to great morbidity and early mortality. The average age of death is 36 years. Actuarial survival from the time of establishing the correct diagnosis has extended from 15 years to more than 30 years. Survival is improving with earlier diagnosis and better treatment in specialty centers [Hexter et al 2015, Forde et al 2021].
Somatic mosaicism for pathogenic variants in NF2. Mosaicism has been suspected in individuals with unilateral vestibular schwannoma and multiple other, often ipsilateral, tumors [Mohyuddin et al 2003, Evans et al 2008, Evans et al 2019]. This has now been confirmed for most individuals in which DNA from multiple tumors has been analyzed [Evans et al 2008, Evans et al 2019].
Histopathology. The tumors of NF2 are derived from Schwann cells, meningeal cells, and glial cells. They are uniformly benign. Approximately 40% of NF2 vestibular tumors have a lobular pattern that is uncommon in tumors from individuals without a diagnosis of NF2.
NF2-associated vestibular schwannomas tend to be more invasive and to have a higher degree of dividing cells than non-NF2 tumors.
NF2-associated meningiomas have a higher degree of dividing cells than non-NF2 meningiomas. NF2 meningiomas are usually of the fibroblastic variety.
No histologic differences have been observed between glial tumors in individuals with NF2 and individuals who do not have NF2.