NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Institute of Medicine (US) Forum on Microbial Threats; Knobler S, Mahmoud A, Lemon S, et al., editors. The Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities: Workshop Summary. Washington (DC): National Academies Press (US); 2006.

The Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities: Workshop Summary.
Show detailsToday, diseases as common as the cold and as rare as Ebola are circling the globe with near telephonic speed, making long-distance connections and intercontinental infections almost as if by satellite. You needn’t even bother to reach out and touch someone. If you live, if you’re homeothermic biomass, you will be reached and touched.
—Angier, 2001
The increasing cross-border and cross-continental movements of people, commodities, vectors, food, capital, and decision-making power that characterize globalization, together with global demographic trends, have enormous potential to affect the emergence and spread of infectious diseases. This chapter summarizes the workshop presentations and discussions on these various aspects of globalization and their implications for the prevention and control of emerging and reemerging infectious diseases.
The unprecedented volume and speed of human mobility are perhaps the most conspicuous manifestations of the present era of globalization. From international tourists to war-displaced refugees, more people are on the move than ever before. They are also traveling faster and are regularly visiting what used to be very remote parts of the world. This movement has the potential to change dramatically the factors involved in the transmission of infectious disease. Of particular concern, over the next 15 years, as the global population continues to grow and economic and social disparities between rich and poor countries intensify, the world will likely continue to witness rapidly growing numbers of migrants in search of employment or a better quality of life. In fact, many political scientists and demographers already refer to the twenty-first century as the “century of migration” (Leaning, 2002). Migrant populations are among the most vulnerable to emerging and reemerging infectious diseases and have been implicated as a key causal factor in the global spread of such diseases, most notably multidrug-resistant tuberculosis (TB). Workshop presentations and discussions addressing this increased human mobility and its effect on infectious disease transmission are summarized here; those addressing the need for improved surveillance of mobile populations are reported in Chapter 2.
Just as modern modes of transportation allow more people and products to travel around the world at a faster pace, they also open the airways to the transcontinental movement of infectious disease vectors. That mosquitoes can cross the ocean by riding in airplane wheel wells is a commonly cited example of this phenomenon and is one of several hypotheses proposed to explain the introduction of West Nile virus into New York City in 1999, the first known incidence of this disease in North America. Beyond such transport of disease vectors, controversial evidence suggests that global warming, much of which is generated by human activities, has caused or is causing changes in vector distributions worldwide and affecting the incidence rates of various tropical infectious diseases, such as malaria and dengue.
Consumers in much of the developed world expect constant access to a wide variety of high-quality, safe food products, regardless of the season or the product’s geographic origin. This demand for a global food market and the resulting transnational movement of food have important implications for foodborne infectious diseases. The global transport of food also raises concerns about the risk of the emergence of antibiotic resistance in humans. Food-producing animals are often given antibiotic drugs for important therapeutic, disease prevention, or production reasons; however, these drugs can cause microbes to become resistant to drugs used to treat human illness.
Although the movement of people and products may be the most conspicuous manifestation of the present era of globalization, the phenomenon’s main driving force is the global expansion of capitalism and the free-market system. Thus, it is useful to examine how the global flow of capital affects emerging and reemerging infectious diseases. The most direct effect results from the financing of environmental projects, such as dams and other water or land development efforts, that alter local vector ecologies and increase the potential for human exposure to infectious diseases. The movement of capital is often accompanied by movements or shifts in decision-making power, another manifestation of globalization with implications for infectious disease transmission.
The following sections address in turn each of these aspects of globalization and its implications for the transmission and spread of infectious disease. The last section summarizes the workshop presentation on the geographic spread of HIV/AIDS. As one participant argued, not only is the HIV/AIDS pandemic a devastating example of how global forces can cause or alter the emergence and spread of infectious disease, but, given its public health and economic impacts, it should probably also be a particular focus of any dialogue on global public health.
THE MOVEMENT OF PEOPLE1
A century and a half ago, it took about 365 days to circumnavigate the globe by ship; today it takes less than 36 hours. Thus the incubation period of many infectious diseases is now longer than the time it takes the infected to travel from one location to another. In the past, infectious disease outbreaks were readily detected on ships as they pulled into port, and the ships were quarantined until the diseases had burned themselves out. Now, should a local outbreak spread silently and globally via an infected traveler or tourist, cases will likely start emerging only days or weeks later in clinics and communities worldwide. Human movement has become a process that involves much more than what happens during the trip itself; the impact persists long afterward, particularly with regard to HIV, TB, and other latent infections.
In the meantime, the world’s population has grown exponentially and more people have been on the move than ever before, especially during the past decade. According to Cetron (2002) migration volumes increased fourfold for the period 1960 through the 1990s. In 2001, an estimated 800 million people traveled; were forcibly displaced; or moved to new countries to work, study, join family members, or escape persecution. These individuals included international travelers (698 million), migrant workers (70–80 million), refugees and uprooted people (22 million), undocumented migrants (10–15 million), and migrant victims of human trafficking (0.7 million). This explosion in the rate of human mobility is almost certainly how HIV was introduced into North America and how fluoroquinolone-resistant gonococci were introduced into North America from Asia.
One participant noted that people on the move not only transmit infectious diseases, but also spread antimicrobial-resistant genetic material. A traveler’s immunological system may afford protection from certain strains but not others. Thus, although there is a tendency to think of travelers as targets for infectious disease per se, it was suggested that perhaps they should also be thought of as interactive biological agents that pick up microbes and drug-resistant microbial genetic material in one part of the world and transport them to another. Although the global spread of drug-resistant microbes was not discussed at length during the workshop, with the exception of multidrug-resistant TB (an especially acute problem in Russia), the globalization of antimicrobial-resistant pathogens was identified as a serious, major issue. Another recent Forum workshop, Issues of Resistance: Microbes, Vectors, and the Host, held in February 2002, was devoted to this topic.
International Travel
International travel is one of the fastest-growing industries worldwide; yearly international tourist arrivals are expected to pass the one billion mark by 2010. Every region of the world is experiencing this increase. An estimated 700 million tourists cross international borders each year. About 60 million people from other countries travel annually to the United States; around the same number of U.S. citizens travel internationally and then return. Between July 1998 and June 1999, the three New York City area airports experienced nearly five million international arrivals. The most rapid increases in international air travel, however, have been in Africa and the Middle East, places where many new infectious diseases are emerging.
Not only do international travelers themselves pose the risk of spreading infectious disease, but the airplanes on which they travel and the cargo that accompanies them also serve as potential sources of vector introduction. Decades ago, international arrivals were subject to vector spraying (i.e., inside the cabin, before the passengers exited the aircraft); participants suggested that it may not be long before routine vector surveillance on airplanes is reinstated. Beyond increasing the risk of the global spread of accidentally introduced infectious disease, international travel also increases society’s vulnerability to acts of terrorism and their potentially devastating economic, psychological, and social repercussions. Part of the impact of the terrorist attacks on September 11, 2001, stemmed from the fact that air travel had until then been taken for granted. When a vehicle used for everyday business was turned into a weapon of destruction and terror, society was psychologically disrupted, and people’s level of comfort with air travel has now declined.
Like air travel, cruise ship travel has increased dramatically, with nearly seven million people in North America traveling by this mode annually. In addition, although cruise ships are increasing in size and becoming more complex in design, they are still fairly densely populated. The average duration of stay on one of these ships is about two average incubation periods, which range from three to 10 days, for the microorganisms responsible for many emerging infectious diseases. These “floating cities,” where people gather from all over the world for short periods of time, represent a unique environment for disease transmission, amplification, and dispersal (see Figure 1-1). Large aggregates of tourist populations not only serve as a potential source for the rapid spread of disease, but are also very difficult to monitor. Moreover, while the travelers on board a cruise ship are at risk of contracting infectious diseases, the people with whom they come into contact when they leave the ship are also at risk. For example, the 1999 outbreak of influenza A virus Sydney in Alaska, which affected about 30,000 people, was preceded by the introduction of an influenza A virus Sydney strain via a cruise ship the previous year (IOM, 2005). It would therefore behoove all nations to be mindful of the ongoing threat of pandemic influenza and the fact that flu strains spread by cruise ships could be an important point of introduction.

FIGURE 1-1
Cruise ship paradigm. SOURCE: Cetron (2002).
Migration and Migrant Health
A 1998 National Geographic article describes human migration as “the dynamic undertow of population change; everyone’s solution, everyone’s conflict” (Parfit and Kasmauski, 1998, p. 11). Migration is propelled by a complex, dynamic interplay of various push and pull factors. Push factors are events such as war, strife, persecution, and famine that drive populations out of regions; pull factors are lures such as peace, freedom, sustenance, economic opportunity, and pleasure that cause populations to move to new locations. This section summarizes the workshop discussions on the latter factors; Chapter 2 summarizes the discussions on forced migration as a consequence of globally driven communal armed conflict.
The four major immigrant-receiving countries are the United States, Canada, Australia, and, more recently, Israel; European countries are seeing waves of immigration as well. The United States is experiencing the third-largest wave of immigration in history—twice as large as the previous peak, which occurred at the turn of the last century. Over the last 30 years, the number of foreign-born individuals in the United States has tripled. Over the past 10 years, 70 percent of U.S. population growth has been due to new Americans, including both direct immigrants (11.2 million people) and children born to immigrants (6.4 million). By 2000, 10.4 percent of the U.S. population (28.4 million) were foreign-born; of these, 51 percent were from Latin America, 25 percent from Asia, 15 percent from Europe, and the remainder from elsewhere.
In addition to individuals seeking permanent residency or citizenship status, migrant labor and work obtained through temporary work visas are significant sources of human movement, particularly between the United States and Mexico. There are an estimated 400 million legal northbound crossings annually along the 2,000-mile-long border between these two nations.
The United States is a nation of immigrants, a legacy that accounts for the country’s economic prosperity and cultural diversity. Although that legacy must be recognized, the health of immigrants, their neighbors, and all populations in U.S. communities must be protected. Migrant health has emerged as a major, unresolved public health issue worldwide, especially in those countries that receive immigrants. Susceptibility to infection usually increases during transit and while living in the destination country, particularly if individuals are separated from their families, partners, or the social and cultural norms to which they are accustomed and that guide behavior in a stable community.
Recent trends in TB, particularly the incidence of multidrug-resistant TB, demonstrate the critical relationship between emerging infectious diseases and population mobility. TB has reemerged as the world’s leading curable infectious killer. An estimated one-third of the world’s population is infected with Mycobacterium tuberculosis, the organism that causes the disease. A three percent increase in new TB cases occurs every year, and approximately 10 percent of these infections develop into active disease. If left untreated, a single infectious person can infect as many as 10 to 15 other people each year.
Fully 95 percent of TB cases occur in the developing world, with a 10 percent increase in Africa being due to coinfection with HIV. (People coinfected with HIV and TB are up to 800 times more likely to develop active TB, and TB kills 15 percent of HIV-infected persons.) TB is reemerging even in the developed world, however, where its prevalence has previously been low, largely because of migration from poorer, high-prevalence countries. In Russia, for example, TB has become the leading cause of death from infectious and parasitic diseases; although the reasons are unclear, immigration is probably an important factor.
Countries that receive migrants generally report that although the number of TB cases among their domestically born populations has declined or stabilized over the last 10 years, the number of cases among their foreign-born populations has increased.
- In the United States, more than 50 percent of new TB cases occur in foreign-born populations. Between 1995 and 1998, the decrease in TB case rates among people born in the United States was three and a half times that of people born elsewhere.
- A 1994 British study showed that the incidence of reported active TB in entrant populations was 20 times higher than the national incidence (Rieder et al., 1994).
- In Denmark, the number of cases of TB has doubled in the past decade, mostly because of immigration (Dragsted et al., 1999).
- In Australia, the prevalence of TB among immigrants is comparable to that in each immigrant’s home country and much higher than that in Australia.
- On the basis of preliminary data from a 2000 International Organization for Migration health assessment of more than 76,000 migrants and refugees, the TB incidence rate among migrant populations is generally five to six times higher than the average rates among the populations of the countries of destination (i.e., the United States, Canada, and Australia); these findings are consistent with reports from the host countries.
Receiving countries of migrants also report increased occurrence of multidrug-resistant TB in their foreign-born populations. Up to 92 percent of such cases in Canada, 90 percent of such cases in Australia, and 76 percent of such cases in the Netherlands were among foreign-born individuals.
The majority (61 percent) of migrants with active TB requiring treatment come from Southeast Asia, corresponding to an incidence of 1,235 per 100,000 population; this figure is eight to nine times higher than the reported cumulative prevalence rates of these countries based on 1999 World Health Organization data. According to other recent estimates, countries with the highest number of annual new multidrug-resistant TB cases worldwide include India (238,806), China (158,813), Russia (11,430), Peru (2,906), Ivory Coast (2,190), Argentina (1,598), Brazil (1,591), Zimbabwe (1,508), South Korea (1,233), Romania (985), Dominican Republic (794), and Sierra Leone (586).
Several factors account for the extreme vulnerability of mobile populations to infectious disease: lack of access to health care and social services in the receiving countries; the conditions and structures of the migration process itself, including social instability, poverty, powerlessness, discrimination, sexual exploitation, and the absence or paucity of social and legal protections; and behavioral changes that are typical of mobile populations. The problem is compounded by the polarity that exists within the health care community: on the one hand, efforts are being made to cure illnesses for which migrant patients are seeking care, but on the other hand, the same health care providers are being asked to screen individuals who are at tremendous risk if the outcome of the screening process is unfavorable. Most migrants generally have no desire to be screened or to visit a health care provider, even when they are experiencing problems, and they often avoid making or keeping appointments as a result. Gaining their trust and convincing them that health care and screening are to their benefit is difficult but necessary. If, for example, individuals do not tell their providers that they are being treated for TB—or worse, if they have stopped treatment—they may not receive adequate, continued care. In addition, many undocumented migrants will not seek medical care because of their illegal status and the risk of being reported to immigration authorities, or even deported.
The United States and other developed nations are not in an ideal position to receive the massive influx of migrants. This is true not only from a public health perspective (e.g., see Chapter 2 for a discussion of mobile health screening and surveillance efforts), but also because of growing tensions between residents and “foreigners” that are creating an in-group versus out-group social phenomenon. Even though individual countries have made liberal and humane attempts to adapt to the influx of people, political and human interactions are becoming more difficult because of this growing tension, particularly in Europe.
GLOBAL DEMOGRAPHIC TRENDS2
Changing world demographics, especially the rapidly increasing size of the world’s population, play a key role in the impact of globalization on the emergence and spread of infectious diseases. In fact, as one participant emphasized, the dynamic interplay between poverty and global population growth is the single most important factor responsible for many infectious disease problems. Even though global population growth is declining at an ever-increasing rate, there will still be a billion more people living on the planet by 2015. As detailed in Global Trends 2015 (NIC, 2001), other important global demographic trends that will likely have a direct impact on infectious disease threats include increasing urbanization in poor countries, the growth of the developed world’s aging population (see below), the demographic consequences of the HIV/AIDS pandemic, and the growing proportion of youth in poor countries. All of these trends are expected to have profound effects on the already sharp demographic and public health disparities between rich and poor countries and fuel even more migration, both legal and illegal, from poor to rich countries.
Diverging Age Distributions
Fully 95 percent of the population growth that is expected to occur over the next 15 years will be in poor countries, especially in urban areas. Meanwhile, population growth rates in rich countries are declining rapidly, and as noted, the proportion of elderly populations in these countries is increasing significantly. This is especially true in Europe and Japan, as elaborated at the April 2002 United Nations Conference on Aging, but it is also the case in the United States. As a result, it is expected that spending on health care for the elderly will threaten to crowd out spending in other areas; there will be intense political pressure from aging cohorts to fund research on treatments for diseases associated with aging rather than on the prevention and control of infectious diseases associated with youth. Garnering the willingness and capability to devote the necessary resources to infectious diseases, particularly those that affect poor regions of the world, will be a political challenge.
The major causes of death in the poorest 20 percent of the world’s population are AIDS, respiratory diseases, diarrheal diseases, and a range of other infectious diseases. In fact, infectious diseases, many of which are associated with youth, are responsible for 80 percent of the differences in the causes of death between the poorest 20 percent and the richest 20 percent of the world’s population—in other words, the excess premature deaths that occur in the poorest parts of the world. An increasing proportion of youth in poor countries is another major global demographic feature expected to emerge by 2015, stemming in part from the profound impact of the global AIDS epidemic on the age distribution of the populations in the hardest-hit countries.
Urbanization in Poor Countries
Urbanization in poor countries is expected to become a key demographic feature of the world over the next 15 years, as more than 90 percent of the population growth in poor countries will be in cities. Already, about half of the world’s population lives in urban areas—more than ever before. By contrast, in most parts of the developed world (e.g., in the eastern United States), the size of the urban population is not expected to change substantially over the next 30 years.
The increasing urbanization in poor countries has significant implications for the transmission and spread of infectious disease.
- About two-thirds of all fatal infectious diseases are spread person to person; greater population density increases transmission by bringing people into closer contact with each other.
- The stress on already weak health systems in many poor countries is increasing.
- Water and sanitation systems are weak or lacking in many urban areas of poor countries, thus increasing susceptibility to contaminated waterborne diseases.
- The huge periurban slums that tend to develop around many major cities in developing countries are typically poor areas that lack infrastructure and resources. This, combined with the warm weather and low latitudes of most of these regions, makes these slums ideal sites for the spread of infectious diseases.
- Because urban centers serve as stopping-off points for international travelers, an infectious traveler could potentially and unknowingly set off a worldwide epidemic. More than 5,000 urban center airports worldwide have regularly scheduled international flights.
- Urban areas in poor countries also serve as temporary or permanent residences for the many people who migrate from their rural homes in search of work; an infected migrant could spread a disease that might otherwise have been locally contained.
The worldwide resurgence of dengue illustrates the impact urban growth can have on the emergence of infectious disease. Sustained transmission of the dengue virus requires a population of between about 150,000 and one million people. A growing number of subtropical and tropical urbanized areas are becoming large enough to favor the ongoing transmission of one or more of the four dengue serotypes. These areas are typically littered with many discarded, nonbiodegradable items (e.g., glass, plastic, and old tires) that provide ideal vector breeding sites. In fact, Aedes aegypti, which carries both the dengue and yellow fever viruses, lives almost exclusively in cohabitation with humans; one could even say that humans have evolved to serve this mosquito since they so readily provide it with the means to propagate. Urbanization, combined with the subtropical and tropical temperatures that favor viral mobility (the extrinsic incubation period is shorter in warmer areas), creates a perfect setting for the emergence of dengue.
Dengue has caused massive epidemics in the United States in the past; however, it has not reemerged because current living conditions, including the use of screens and air conditioning, limit its transmission. Interestingly, in 1985 another vector, Aedes albopictus, was introduced into the United States, and since then it has spread to at least 12 states via used tires. Dengue has, moreover, reemerged with a vengeance in most of the rest of the Americas, where the number of cases has risen from only a few to nearly one million (see Figure 1-2). Not surprisingly, its reemergence coincides with the environmental presence of glass, plastics, and tires. This region is witnessing all four dengue serotypes, all of which can cause illness and have caused pandemics in the past. When individuals are infected with any of the serotypes for the first time, they usually develop classic dengue, a less severe form of the disease. Once they have been infected with another serotype, however, they are at risk for a more severe form of the disease; infection with one serotype offers no protection against another. One of the more severe forms of the disease, dengue hemorrhagic fever, or dengue shock syndrome, is one of the worst possible outcomes and has about a 10 percent mortality rate. The Caribbean is experiencing an epidemic of DEN-3, a dengue virus serotype that has not been present in the area for the past 30 years and that was recently reintroduced from Asia. Because the Caribbean has experienced epidemics involving other serotypes, the likelihood that dengue hemorrhagic fever will appear in the region over the next few years is even greater than it would otherwise be.

FIGURE 1-2
Dengue cases, 1980–2001. SOURCE: Corber (2002).
Although infection with dengue virus is not associated with HIV/AIDS, as far as is known, it does cause activation of certain cell surface molecules (HLA class II molecules). This phenomenon may play a role in the HIV/ AIDS epidemic in the Caribbean by providing HIV with more cellular targets to attack. This may explain why the average time interval between HIV infection and the onset of AIDS is shorter in the Caribbean, where the recent emergence of dengue is a major public health problem, than in North America and Europe (Cleghorn, 2002).
The history of dengue in the Caribbean demonstrates how a false sense of security can breed reemergence. In the 1930s it was believed that if Aedes aegypti could be eradicated, so, too, could disease. Although a number of countries participated in eradication efforts and had achieved local success by about 1970, not all countries participated, and the mosquito was not entirely eradicated from the region (see Figure 1-3). However, because the numbers of mosquitoes had diminished in most areas and because funding had dried up, surveillance ceased. As a result, over the last 30 years, with the increasing intensity of globalizing forces such as trade and travel, Aedes aegypti has reinfested nearly every country in the American region except for Canada (see Figure 1-4).
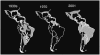
FIGURE 1-3
Reinfestation of Aedes aegypti. SOURCE: Corber (2002).

FIGURE 1-4
World distribution of dengue, 2005. SOURCE: CDC (2005).
THE MOVEMENT OF VECTORS3
Increased vector movement may be just as important as increased human movement in contributing to the global spread of infectious diseases. There is perhaps no better illustration of this point than the global spread of Aedes aegypti and the worldwide resurgence of dengue, as described above. This same mosquito has also been responsible for yellow fever outbreaks worldwide; endemic zones include every country in South America except for Brazil (see Figure 1-5a) and more than half the countries in Africa (see Figure 1-5b).

FIGURE 1-5a
Yellow fever-endemic zones in the Americas, 2005. SOURCE: CDC (2005).

FIGURE 1-5b
Yellow fever-endemic zones in Africa, 2005. SOURCE: CDC (2005).
Vectors are usually introduced into new areas inadvertently via vehicles used to transport people or commodities (e.g., airplanes) or via commodities that are being transported. It has been demonstrated experimentally that a number of different disease vectors can survive in the wheel wells of jet aircraft at high altitudes for long intercontinental flights. Mosquitoes also hitchhike on used car tires that are being transported for retreading or other purposes. For example, the Asian tiger mosquito, Aedes albopictus, a dengue virus vector, was introduced to the North American continent on rubber tires shipped to Houston. The United States–Mexico border, a dumping ground for used tires, is an important breeding site for Aedes mosquitoes.
Animal importations are another potential source of introduced zoonoses. Each year many U.S. ports of entry receive millions of animal importations from countries where a variety of diseases are endemic. In a single year (i.e., August 1998 to July 1999), there were more than 2.8 million international animal importations into New York City; most of these were amphibians (61 percent) and birds (36 percent). In 1996, the port of Miami received more than 30 million animal imports, most of which (96 percent) were fish and aquatic invertebrates. It should be noted, moreover, that these figures represent only legally imported animals and that a large trade in illegally imported animals exists as well.
Before its first appearance in New York City in 1999, West Nile virus was not present in the western hemisphere. It has now spread throughout the North American continent, into Canada, Mexico, Central America, and the Caribbean. This example of the potential for the introduction of a vectorborne infectious disease into a new hemisphere also illustrates how a multitude of factors can converge to provide a ripe opportunity for emergence: the most common vector of West Nile virus in the United States, the common household mosquito (Culex pipiens), was already ubiquitous in the New York metropolitan area; the marshy habitat where the disease emerged was an ideal mosquito breeding ground; the location of emergence was near a major international airport; and international travelers are constantly arriving in Queens, which houses perhaps one of the most ethnically diverse populations in the world.
Although the virus was almost certainly introduced via a transportation vehicle, it is unclear whether it was introduced via a vector mosquito or some other means. Other possibilities include the arrival of an infected human, an infected bird on an airplane or other transportation vehicle, an infected migrating bird, or an infected animal reservoir in the New York City area. At this point, there may be no way to trace the precise means of introduction, which in any case is somewhat immaterial, as the virus is well established in animal populations and has spread rapidly down the East Coast of the United States.
Effects of Global Temperature Change on Vector Movement
Few would argue at this point in time that global warming is occurring and is generated primarily by human activities. Conclusive evidence suggests that industrialization, the burning of fossil fuels for heat and transportation, and deforestation cause global warming by increasing the levels of greenhouse gasses and eliminating carbon sinks. It is also known that many aspects of vector behavior, including the range of habitability, are at least partially driven by temperature. Thus, there is some concern that as global temperatures rise, vectorborne diseases could spread to areas where they have not previously existed (i.e., they would move north in the northern hemisphere, south in the southern hemisphere, and higher in mountainous areas).
However, empirical studies investigating changes in the distribution of vectors and vectorborne diseases due to global warming have yielded highly contradictory results. Some studies have shown that higher temperatures have led to increased rates of malaria, dengue, and other vectorborne diseases in temperate areas; others have not. Moreover, although temperature-dependent mathematical models predict that the prevalence of vectors and vectorborne diseases, particularly malaria, will increase in temperate zones and at higher altitudes as temperatures rise, multivariate models incorporating other variables, such as rainfall and humidity, show that higher temperatures do not necessarily result in increased incidence and global redistribution of mosquito vectors (Rogers and Randolph, 2000). In fact, the worldwide incidence of malaria may actually decrease with global warming, as many climatic factors that accompany higher temperatures appear to counteract the effects of temperature; for example, the increased rainfall that often accompanies higher temperatures could wash out the breeding pools of anopheline mosquitoes. Some scientists who believe that the resurgence of malaria in the East African highlands is not climate related argue that the resurgence is more likely associated with other factors, such as declining surveillance and treatment (Hay et al., 2002).
El Niño Southern Oscillations (ENSOs) would appear to provide a natural opportunity for investigating the effects of increased temperature and rainfall fluctuations on the incidence of vectorborne diseases. Because the phenomenon lasts only one to two years, however, it is difficult to extrapolate ENSO findings to global warming. The social, architectural, and engineering adaptations that would be expected to occur with increased global warming cannot take place during such short time periods. Over the next century, when temperatures worldwide are expected to increase by as much as 5–10ºC, human behavior will likely change in unforeseen ways. Moreover, as with other studies of the effects of temperature changes, the results of studies of ENSO-related temperature increases are contradictory: some studies suggest that temperature increases do in fact lead to greater incidence of malaria, dengue, and other diseases in Africa, Asia, and elsewhere, but others show that there is very little change.
As important as it is to take a global perspective, it is also very difficult to make global generalizations about diseases, such as malaria, that are so shaped by local conditions and could emerge under any of an infinite variety of local circumstances. As Hackett (1937, p. 226) observed: “Everything about malaria is so molded by local conditions that it becomes a thousand epidemiological puzzles. Like chess, it is played with a few pieces but is capable of an infinite variety of situations.” Malaria is transmitted by dozens of anopheline species; some breed preferentially in warmer temperatures, whereas others prefer cooler temperatures and cannot even survive in warmer conditions. Mathematical–spatial models generally lack sufficient geographic resolution to account for local ecological conditions.
The Movement of Livestock
Although the movement of livestock is not recognized as a cause of zoonotic diseases, it was cited by workshop participants as an important manifestation of globalization with significant economic and psychological impacts. The emergence of foot-and-mouth disease in England wiped out an entire market, closed export doors, and had devastating economic consequences. It also had a tremendous psychological impact; indeed, it resulted in a number of suicides. In one case, a third-generation cattle breeder had just received an award in the mail for having the number-one herd in England; his cattle were killed later that day. The outbreak also affected health care, schooling, and food distribution in general. If foot-and-mouth disease were introduced into the United States, either accidentally or intentionally, the consequences would be devastating, both economically and psychologically.
Direct contact with livestock and other animals can also have an impact on human health. Between September 1998 and June 1999, a large outbreak of encephalitis occurred among pig farmers in Malaysia, and Nipah virus was identified as the causal agent. There were 265 cases of the illness reported to the Malaysian Ministry of Health, including more than 100 deaths. Transmission of the Nipah virus to humans occurs primarily through direct contact with infected pigs or swine tissue; no evidence of human-to-human transmission has been found. As a result of this outbreak, more than 900,000 pigs were culled.
Livestock are used and moved around for other reasons besides food. Too often people forget how closely they are interrelated with animals through the use of animal products, from leather shoes to cosmetics. The United States was very concerned, for example, about the importation of gluten by-products, which are included in cosmetics and other products, during the European outbreak of bovine spongiform encephalophy (mad cow disease) in the 1990s.
THE MOVEMENT OF FOOD4
The way people eat is changing the way food is transported around the world. In the 1950s, supermarket shelves were filled with hundreds of items; today they are filled with tens of thousands of food products from all over the world. Consumers expect to be able to choose from a wide range of safe, high-quality food items, including fresh meat and produce, year-round. To meet these expectations, the food industry must import items from many different parts of the world. A globalized food supply raises questions about food safety and opens the door for potential bioterrorist attacks. For example, are people being exposed to new and different pathogens? What factors can lead to an increased risk of infectious disease under these circumstances? What controls are in place to manage this potential risk? The globalization of the food supply also raises many important questions about antibiotic resistance. For instance, what drugs are being used to treat food animals? What local controls exist? What effect does the indiscriminate use of antibiotics in certain parts of the world have on enteric pathogens that may enter the United States (or other countries) through the food supply?
Several hundred known foodborne microbial agents, including bacteria, viruses, and parasites, pose potential dangers everywhere in the world, including the United States. Added to these are a multitude of chemical hazards (i.e., antibiotics, carcinogens, and heavy metals), physical hazards, prions, allergens, and various other agents that threaten human health. New food-transmitted agents are continually being identified. Threats identified since 1977 include Campylobacter jejuni; Campylobacter fetus subsp. fetus; Cryptosporidium parvum; Cyclospora cayetanensis; Shiga toxin-producing Escherichia coli; Listeria monocytogenes; noroviruses5; Salmonella bongori; Salmonella enterica serovar Enteritidis; Salmonella enterica serovar Typhimurium; transmissible spongiform encephalopathic agents; Vibrio cholerae O139; Vibrio vulnificus; Vibrio parahaemolyticus; and Yersinia enterocolitica. Although all of these potential hazards occur worldwide, some, such as parasites, are more problematic in some areas than in others. No one country or community has the capability to test for all possible hazardous agents in its imported food products, which makes local control very important.
Each year, a growing number of different foods are imported into countries throughout the world. Recent outbreaks have demonstrated the impact of imported produce on the occurrence of foodborne disease. In 1998, for example, an outbreak of multidrug-resistant Shigella sonnei infection occurred among patrons of restaurants in Minnesota (CDC, 1999). The culprit in this case was imported parlsey.
Guatemalan raspberries are a classic example of a cash crop that is introduced into a poor country with unsafe cultivation practices and then reintroduced into the North American market as a contaminated fresh produce item. A herald wave of 35 cases of cyclosporiasis occurred in 1996, followed by about 1,400 cases the next year, with clusters occurring in both the United States and Canada. Careful case-controlled studies determined that the outbreaks were associated with contaminated raspberries; laboratory-confirmed cases demonstrated that the clusters occurred seasonally, following the importation of Guatemalan raspberries. At the end of May 1997, the Guatemalan Berry Commission voluntarily suspended shipments of raspberries to the North American market, and the impact was profound: the outbreaks ceased. The following year, however, even though the commission had imposed voluntary controls on cultivation (because it was believed that contaminated groundwater had been used to spread insecticides on the raspberry plants, and there was no way to decontaminate the berries), Canada continued to import the raspberries and continued to experience cyclosporiasis outbreaks. The United States, on the other hand, prohibited the importation of Guatemalan raspberries and experienced no further outbreaks. As this example demonstrates, local conditions, local controls, and import controls all play significant roles in the prevention and control of outbreaks of foodborne disease.
Local conditions set the stage for a pathogen to enter the food supply. The health of the workforce, the health of animals, local sanitary conditions, process controls in the food production plant, water quality, and refrigeration control all play a role. Of these, workforce health and local sanitary conditions are the most critical; both are believed to have contributed to the 1996–1998 cyclosporiasis outbreak. The presence of parasites in either the water or the workforce has also been implicated in cryptosporidiosis and giardiasis outbreaks, while bacterial agents in either the water or the workforce have been associated with diseases caused by vibrios and other enteric organisms.
From the perspective of the U.S Department of Agriculture, local inspectors are responsible for safeguarding their food exports. In 1999 and 2000, there were 5,972 inspectors in the 34 countries exporting food products to the United States, including 1,493 inspectors in Canada, 504 in Australia, 586 in Denmark, and 910 in New Zealand. The United States typically imports 2.4–2.8 billion pounds of meat and poultry annually. In fiscal year 2001, the United States imported food products from 33 different countries, with the amounts imported varying greatly by country. For example, more than 1,500 million pounds of meat and poultry was imported from Canada, but only 18,000 pounds from Switzerland. On the basis of 1999 data, most imports come from Canada (49 percent), Australia (22 percent), New Zealand (14 percent), and Denmark (four percent). Of these imports, 85 percent are fresh meat, 13 percent processed meat, and two percent poultry. The imports come from 1,200 authorized plants distributed among the 33 countries; more than 70 percent of these plants are in Canada (470), Italy (115), Denmark (100), Australia (99), and New Zealand (81).
A country wishing to export meat, poultry, or eggs to the United States must establish and maintain a two-step inspection system equivalent to that of the United States. First, the system must be assessed by means of a document review, which involves the evaluation of five risk factors: sanitation controls, animal disease controls, slaughter and processing controls, residue controls, and enforcement controls. If this first step is successful, the second is an onsite audit of the risk factors, plant facilities, equipment, laboratories, training programs, and in-plant inspection operations. Countries must be recertified annually, and the U.S. Food Safety and Inspection Service (FSIS) regularly conducts onsite audits to ensure that this system equivalency is maintained. Problems may lead to the suspension of eligibility.
All imported products require a foreign inspection certificate. When products arrive in the United States for importation, the following must be documented on the certificate: product name, establishment number, country of origin, name and address of manufacturer, quantity and weight of contents, list of ingredients, species of animal, and identification marks. Should a recall be necessary, this information allows control of the contaminated product. In addition, importers must file an entry form with the U.S. Customs Service within five days of product arrival.
FSIS also requires an original certificate from the country of origin indicating that the product has passed local inspection. Even after passing local inspection, all meat and poultry shipments must be held and reinspected upon arrival. This includes a visual inspection, certification check, and product examination for chemical or microbiological contamination. Egg products are reinspected at the processing facility, not at the holding warehouse.
Microorganisms for which tests are routinely conducted include Listeria monocytogenes and Salmonella in ready-to-eat foods; Escherichia coli O157:H7, Salmonella, L. monocytogenes, and Staphylococcus aureus in dried and semidried sausage; and E. coli O157:H7 in raw ground beef. Residue sampling plants randomly sample animal products for drug residues as part of the National Residue Program.
THE MOVEMENT OF CAPITAL6
The movement of capital refers, in its simplest sense, to the transferability of money and the increasing linkages within the world’s financial system. While having received scant attention in the public health literature, the global flow of capital and the international unification of markets have been emphasized by social scientists and in the more economically oriented globalization literature. Their importance is reflected in the fact that the “development of global financial markets” is Soros’s (2002) operational definition of globalization.
In fact, many would argue that the movement of capital is a crucial component of the very definition of globalization. Although the term is commonly used to describe contemporary society, it is often ill defined and misunderstood (Buse and Walt, 2002). In the health sciences literature, it usually refers to the process of growing global interdependence, particularly as manifested by increasing international transportation; at least for social scientists, however, this interdependency is only part of the process of globalization. A workshop participant suggested that the health sciences field could benefit from an explicit understanding of the concept of globalization as developed in the literature in such fields as international relations, political economy, and political geography. As was noted in a recent article on the implications of the globalization of cholera for global governance, “This is a rich and highly relevant literature. It documents what structural changes are occurring toward a global political economy, how power relationships are embedded within this process of change, what varying impacts this may have on individuals and groups, and to what extent global governance could effectively mediate this process” (Lee and Dodson, 2000, p. 213). Globalization encompasses much more than an increase in international interdependency and connectivity; in particular, it also includes the movement of capital.
The most direct consequence of the international movement of capital for emerging infectious diseases is the financing of environmental projects in a country with external funds. These projects, frequently planned by a coalition of local and international environmental planners, usually have either intended or unintended environmental effects and alter human–environment relations in ways that have significant implications for host–pathogen interactions and potential human exposure to vectorborne or waterborne diseases.
Water Projects
Water projects perhaps provide the best example of how the global movement of capital affects the emergence and transmission of infectious disease as a result of the alteration of local conditions. The explicit purpose of dams and other water projects is to fuel local and regional economies through the generation of hydroelectric power, to generate new capital, and to integrate countries into the global economy. The massive Three Gorges Dam project, for example, is designed explicitly to power Chinese industrial growth and further China’s position in the global economy. The costly construction of dams usually entails large investments of outside capital. Even when financing comes almost exclusively from domestic sources, as in the case of the Three Gorges Dam, at least some funding usually derives indirectly from business growth due to globalization.
The construction of dams has many known deleterious public health consequences. For example, construction of the Aswan Dam in Egypt has been implicated in increased rates of schistosomiasis (Abdel-Wahab, 1982; El Alamy and Cline, 1997). Likewise, the development of dams in the Senegal River basin is among the major factors leading to a significantly increased prevalence of schistosomiasis over a period of only three years (Gryseels et al., 1994). As another example, the construction and anticipated completion of the Three Gorges Dam—presumably the largest dam in the world and, some would suggest, the largest public works project in the history of the world—will almost certainly lead to the introduction of schistosomiasis. This concerns many scientists because schistosomiasis will be introduced into an area upstream of the dam where the disease is not endemic, where ecological conditions will be highly conducive to its transmission, and where human exposure is expected to be substantial. Moreover, construction of the Three Gorges Dam is resulting in massive population displacement, forced migration, and very high population densities in certain regions, all of which further increase the likelihood of the emergence of infectious disease.
Land Modification Projects
Land modification and clearance projects that involve capital flow can also have significant consequences for the emergence and transmission of infectious diseases through their alteration of local human–environment relations. For example, the clearance of land in Malaysia for the construction of rubber plantations, economic development, and the promotion of an export economy have resulted in notable increases in the rates of malaria transmission among plantation laborers. Environmental conditions have been altered to such an extent that the landscape has became conducive to anopheline mosquito breeding, and the level of human contact with anopheline mosquitoes has greatly increased.
As another example, deforestation in the Amazon, both for logging and for gold mining, has been linked to increased incidence of Anopheles darlingi mosquitoes, the primary vector of malaria in South America. These mosquitoes were not present in the area before the mid-1960s. The situation is exacerbated by the fact that mercury, which is used to extract gold from the ore, acts as an immunosuppressive agent, increasing the likelihood of contracting malaria (Patz, 2002; Silva et al., 2004). Moreover, the migration of laborers into and out of these areas contributes to the spread of disease throughout South America.
It should be noted that, although the clearing of land results in an increase in malaria in most instances, it can also lead to a decrease in the rate of malarial transmission. For example, the clearing of land in Thailand for tapioca farming led to a decrease in malarial transmission by destroying the habitat of the vector, Anopheles dirus (Bockarie and Paru, 1993).
THE MOVEMENT OF DECISION-MAKING POWER7
Workshop participants identified as another important manifestation of globalization shifts in the locus of power in global decision making, whereby some localities are marginalized in their ability to control what happens to local society and others have more central control and are able to project power over great distances. The increasing uniformity of society, the erosion of locally controlled commodities and markets, and the general loss of societal control all reflect these shifts in power.
It is this dimension of globalization—the shift in decision-making power—that is so politically controversial and was responsible for protests at the World Trade Organization’s meeting in Seattle in 1999 (Sassen, 1998). Although many people, such as Friedman (2000), perceive globalization as a phenomenon that promotes well-being and economic opportunity, others view it as an alienating social force that marginalizes those already at the periphery of society. Even if one does not agree with the latter sentiment, a workshop participant suggested that it might be helpful to understand this perspective, as it may elucidate the nature of some of the underlying social factors in the global emergence of infectious diseases. Ultimately, these underlying social factors—including poverty, population growth, and the massive displacement of people—must be addressed to ensure a sustainable global capacity to prevent and control the emergence and spread of infectious diseases.
THE GEOGRAPHIC EVOLUTION OF HIV/AIDS8
Not only does the global spread of HIV/AIDS serve as a paradigm for the effect of globalization on emerging infectious diseases, but HIV/AIDS has also emerged as an overriding concern because it makes people more susceptible to other infectious diseases, particularly TB. Because of its economic impact, moreover, it has a major effect on the absorptive capacities of the public health systems of developing countries. In fact, as one workshop participant noted, most global health issues can truly be understood only within the larger context of the HIV/AIDS pandemic.
Since its emergence in the early-1980s, HIV has infected about 60 million people worldwide, 40 million of whom were estimated still to be living by the end of 2001. The global spread of HIV is attributed mainly to the movement of people.
Even though southern Africa and the Great Lakes region of eastern Africa remain the areas of the world hardest hit by the HIV/AIDS pandemic, growing rates of infection in other areas, particularly elsewhere in Africa, are of increasing concern. Nigeria and Ethiopia, the largest African countries, may be at a point where the epidemic is about to become much more serious over the next five years. If this is the case and if the situation in Nigeria and Ethiopia parallels that of southern Africa in the early 1990s, it is not inconceivable that the number of HIV/AIDS cases in Africa could double in the next five years.
The current official HIV/AIDS rate in Nigeria is six percent, but it is likely that the real number is closer to 10 percent. The Nigerian government has shown some commitment to dealing with the problem, but there has been very little progress in terms of destigmatization. Continuing social, political, and economic tensions associated with this highly populated nation are diverting attention away from the threat of AIDS.
In other parts of the world, India has the greatest potential for a widespread increase in the number of people with HIV/AIDS, given that 70 to 80 percent of the population lives in poor rural areas where the education rates are low and the public health infrastructure is weak. HIV/AIDS is already costing India substantially in terms of lost productivity and treatment costs.
Although Russia has one of the fastest-growing rates of HIV infection in the world, with the number of official cases roughly doubling each year since 1998, it is not facing quite the same level of threat as the countries of sub-Saharan Africa and India. The rapid spread of HIV into Russia, as well as Ukraine, has been associated with the opening up of the Eastern European countries and the subsequent movement of people between zones where the populations have various rates of HIV infection. Most new infections in Russia appear to be linked to injection drug use, but several other factors—including high rates of unemployment, a disintegrating public health infrastructure, and the general poor status of health care services—make the country vulnerable to further increases. On the other hand, given the high rate of literacy and general education throughout Russia, there is reason for optimism. Russia’s extensive media links could be used to develop an active education program that could have a significant impact in a fairly short period of time. The country’s demographic profile, which is skewed toward an older population, is also likely to blunt the impact of HIV/AIDS.
The Chinese government and news media have recently focused much more attention on HIV/AIDS than in the past, suggesting that the situation is worrisome and that the government is becoming aware of the potential risks. Still, China has far to go in terms of acknowledging the scope of the problem. Officially, 850,000 people in China are infected with HIV, but this number is obviously far at odds with reality.
The spread of HIV/AIDS, both in sub-Saharan Africa and elsewhere, is likely to hinder prospects for a transition to democracy by undermining civil society, hampering the evolution of sound political and economic institutions, and polarizing the struggle for power and the control of resources in poor countries.
REFERENCES
- Abdel-Wahab MF. Schistosomiasis in Egypt. Boca Raton, FL: CRC Press Inc; 1982.
- Acheson D. Globalization of the Food Supply; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Angier N. Together, in Sickness and in Health, New York Times Magazine. May 6, 2001. [accessed on January 18, 2006]. http://www
.nytimes.com /2001/05/06/magazine/06INTRO.html. - Bockarie MJ, Paru R. Forest Clearing, Mosquitoes and Malaria; Report of the Jubilee International Colloquium, Papua New Guinea Institute of Medical Research, Madang. 1993.
- Buse K, Walt G. Globalisation and multilaterial public-private health partnerships: Issues for health policy. In: Lee K, Bruce K, Fustukian S, editors. Health Policy in a Globalising World. Cambridge, UK: Cambridge University Press; 2002. pp. 41–62.
- CDC (Centers for Disease Control and Prevention). Outbreaks of Shigella sonnei infection associated with eating fresh parsley—United States and Canada, July–August 1998. MMWR. 1999;48(14):285–290. [PubMed: 10227795]
- CDC. Map: World Distribution of Dengue. 2005. [accessed October 18, 2005]. [Online]. Available: http://www
.cdc.gov/ncidod /dvbid/dengue/map-distribution-2005.htm. - CDC. Map: Yellow Fever Endemic Zones in the Americas. 2005. [accessed October 18, 2005]. [Online]. Available: http://www2
.ncid.cdc .gov/travel/yb/utils/ybGet .asp?section=dis&obj =yellowfever.htm. - CDC. Map: Yellow Fever Endemic Zones in Africa. 2005. [accessed October 18, 2005]. [Online]. Available: http://www2
.ncid.cdc .gov/travel/yb/utils/ybGet .asp?section=dis&obj =yellowfever.htm. - Cetron M. The World and Its Moving Parts; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Cleghorn F. Considering the Resources and Capacity for the Response; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Corber S. Response to the Shifting Trends; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Dragsted UB, Bauer J, Poulsen S, Askgaard D, Andersen AB, Lundgren JD. Epidemiology of tuberculosis in HIV-infected patients in Denmark. Scand J Infect Dis. 1999;31(1):57–61. [PubMed: 10381219]
- El Alamy MA, Cline BL. Prevalence and intensity of Schistosoma haematobium and S. mansoni infection in Qalyub, Egypt. Am J Trop Med Hyg. 1997;26(3):470–472. [PubMed: 869100]
- Friedman TL. The Lexus and the Olive Tree: Understanding Globalization. New York: Anchor Books; 2000.
- Gordon D. The Global Infectious Disease Threat; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Grondin D. Global Migration and Infectious Diseases; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Gryseels B, Stelma FF, Talla I, van Dam GJ, Polman K, Sow S, Diaw M, Sturrock RF, Doehring-Schwerdtfeger E, Kardorff R. Epidemiology, immunology and chemotherapy of Schistosoma mansoni infections in a recently exposed community in Senegal. Trop Geogr Med. 1994;46(4):209–219. [PubMed: 7825223]
- Hackett LW. 1937Malaria in Europe: An Ecological Study London, England: Oxford University Press; 226.
- Hay SI, Cox J, Rogers DJ, Randolph SE, Stem DI, Shanks GD, Myers MF, Snow RW. Climate change and the resurgence of malaria in the East African highlands. Nature. 2002;415(6874):905–909. [PMC free article: PMC3164800] [PubMed: 11859368]
- IOM (Institute of Medicine). The Threat of Pandemic Influenza: Are We Ready? Washington, D.C: The National Academies Press; 2005. [PubMed: 20669448]
- Kimball AM. Considering the Resources and Capacity for Response; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Leaning J. Health, Human Rights, and Humanitarian Assistance: The Medical and Public Health Response to Crises and Disasters; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- LeDuc J. The Global Application of Tools, Technology, and Knowledge to Counter the Consequences of Infectious Diseases: A Discussion of Priorities and Options; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 17, 2002.
- Lee K, Dodson R. Globalization and cholera: Implications for global governance. Global Governance. 2000;6(2):213–236.
- Mayer J. Changing Vector Ecologies: Political Geographic Perspectives; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- NIC (National Intelligence Council). Global Trends 2015. 2001. [accessed January 24, 2005]. [Online]. Available: http://www
.cia.gov/cia /publications/globaltrends2015/ - Parfit M, Kasmauski K. Human migration. National Geographic. 1998;194(4):6–35.
- Patz J. Invited Discussion: Considering the Resources and Capacity for Response; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
- Rieder HL, Zellweger J-P, Raviglione MC, Keizer ST, Migliori GB. Tuberculosis Control in Europe and International Migration. Report of a Working Group. Eur Respir J. 1994;7(8):1545–1553. [PubMed: 7957845]
- Rogers DJ, Randolph SE. The global spread of malaria in a future, warmer world. Science. 2000;289(5485):1763–1766. [PubMed: 10976072]
- Sassen S. Globalization and Its Discontents. New York: New Press; 1998.
- Silva IA, Nyland JF, Gorman A, Perisse A, Ventura AM, Santos EC, Souza JM, Burek CL, Rose NR, Silbergeld EK. Mercury exposure, malaria, and serum antinuclear/ antinucleolar antibodies in Amazon populations in Brazil: A cross-sectional study. Environmental Health. 2004;3(1):11. [PMC free article: PMC538267] [PubMed: 15522122]
- Soros G. George Soros on Globalization. New York: Public Affairs; 2002.
- Widdus R. Partnering for Success: The Role of Private-Public Sector Collaboration; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 17, 2002.
- Wilson M. Invited Discussion: A Response to the Shifting Trends; Presentation at the Institute of Medicine Workshop on the Impact of Globalization on Infectious Disease Emergence and Control: Exploring the Consequences and Opportunities; Washington, D.C.. Institute of Medicine Forum on Emerging Infections; Apr 16, 2002.
Footnotes
- 1
This section is based on the workshop presentations by Cetron (2002), Grondin (2002), Mayer (2002), and Wilson (2002).
- 2
This section is based on the workshop presentations by Cetron (2002), Cleghorn (2002), Corber (2002), Gordon (2002), Leaning (2002), LeDuc (2002), Widdus (2002), and Wilson (2002).
- 3
This section is based on the workshop presentations by Cetron (2002) and Mayer (2002).
- 4
This section is based on the workshop presentations by Acheson (2002) and Kimball (2002).
- 5
Formerly known as Norwalk-like viruses.
- 6
This section is based on the workshop presentations by Mayer (2002) and Patz (2002).
- 7
This section is based on the workshop presentation by Mayer (2002).
- 8
This section is based on the workshop presentation by Gordon (2002).
- A World in Motion: The Global Movement of People, Products, Pathogens, and Power...A World in Motion: The Global Movement of People, Products, Pathogens, and Power - The Impact of Globalization on Infectious Disease Emergence and Control
- Fatty Acid Hydroxylase-Associated Neurodegeneration - GeneReviews®Fatty Acid Hydroxylase-Associated Neurodegeneration - GeneReviews®
- Memory and Plasticity in the Olfactory System: From Infancy to Adulthood - The N...Memory and Plasticity in the Olfactory System: From Infancy to Adulthood - The Neurobiology of Olfaction
- Antenatal and Postnatal Mental HealthAntenatal and Postnatal Mental Health
- Drug Class Review: Second-Generation AntidepressantsDrug Class Review: Second-Generation Antidepressants
Your browsing activity is empty.
Activity recording is turned off.
See more...