This book is distributed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0) ( http://creativecommons.org/licenses/by-nc-nd/4.0/ ), which permits others to distribute the work, provided that the article is not altered or used commercially. You are not required to obtain permission to distribute this article, provided that you credit the author and journal.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.

StatPearls [Internet].
Show detailsContinuing Education Activity
Abrasion is the superficial denudation of the epithelium due to scraping, impact, or pressure. The majority of abrasions heal without leaving any scars. However, the abrasions that extend into the dermis may result in tissue scarring after healing. Abrasions appear in all forms of blunt trauma, with friction and impact being the most common mechanisms. While managing abrasions is relatively simple, there can be significant medico-legal considerations. This activity discusses the evaluation and management of abrasion and highlights the role of the interprofessional team in managing this condition.
Objectives:
- Identify the characteristics and features of abrasions, including their appearance, size, location, and associated injuries.
- Assess the severity and extent of abrasions, including involvement of deeper structures, to determine the need for further evaluation, referral, or specialized care.
- Select and utilize appropriate tools, instruments, and materials for wound management, including dressings, sutures, adhesive agents, and topical medications, based on patient-specific needs and wound characteristics.
- Coordinate multidisciplinary care for patients with severe or complicated abrasions, involving specialists from various disciplines, such as orthopedic surgery, dermatology, or infectious disease, to provide comprehensive and coordinated care.
Introduction
Abrasions are superficial injuries that occur on the skin and visceral linings of the body, disrupting tissue continuity. They are typically minor wounds, mainly limited to the epidermis, and usually do not cause significant bleeding. Most abrasions heal without leaving any scars. However, if the abrasion extends into the dermis, it may result in scar tissue formation during the healing process.
Abrasions most commonly occur due to friction against the epidermis, leading to the denudation of the outer layer. Abrasions appear in various forms of blunt trauma, with friction and impact being the most common mechanisms. While less frequent, pressure abrasions can have a greater medicolegal significance, especially for identifying the causative material.
Etiology
Abrasions are classified into 3 types based on clinical presentations and etiological factors. These include linear or scratch abrasions, grazed or brush abrasions, and patterned abrasions. Impact abrasions result from a swift blow and forceful blow. Patterned abrasions resulting from blows, collisions, and auto versus pedestrian accidents are examples of impact abrasions.[1][2]
Linear or Scratch Abrasions
Linear abrasions occur when tangential forces cause the epidermis to be stripped away. They are the simplest injuries that typically heal by primary intention, without any sequelae.[3] Linear abrasions hold significant medicolegal importance, especially in specific areas such as the neck, inner thighs, and genitalia. Linear or semicircular injuries are classically seen as a result of nail scratches, and their presence on the inner aspect of thighs and around female genitalia may indicate resistance in cases of sexual assault. Likewise, nail scratch abrasions on the neck may suggest strangulation.[4][5][6]
Grazed or Brush Abrasions
Grazed abrasions usually occur in multiple presentations and result from friction against a broad, rough surface. These are most commonly observed in incidents such as road traffic accidents and falls during sports activities. Grazed abrasions are caused by the body being dragged against a rough surface, leading to the scraping off of the epidermis. The depth of grazed injuries varies depending on the surface's irregularity and the body's speed. Extensive, grazed abrasions are sometimes referred to as "brush burns."[7]
Patterned Abrasion
Patterned abrasions occur when perpendicular force is applied to the epidermis, resulting in an impression of the offending object. Depending on the duration of contact with the offending object, they can be further subclassified as pressure abrasion and impact abrasion. Pressure abrasions result from prolonged compression of the epidermis, and they require minimal force to occur. For example, a ligature mark produced using roughing material for hanging leaves an imprint of the material used.[8]
Epidemiology
Abrasions can occur at any stage of life without a specific preference for any age or sex. They are primarily accidental across all age groups. However, abrasions caused by intentional injuries are more prevalent among individuals in middle age compared to those in the extremes of age. Intentional injuries related to sexual offenses are more common in females. Unintentional abrasions are frequently associated with falls and sports-related injuries in children, while falls are a prevalent cause among older patients.
Abrasions are the most common form of injury in children accounting for 70.7% of all reported injuries. The head and torso are the primary sites, comprising 50% of all recorded abrasions. The upper limbs account for 15.4%, while the lower limbs comprise about 34.6% of all reported cases.[9] However, there exists a potential for significant underreporting of the overall prevalence of abrasions and their predilection for a particular site, as people sustaining minor abrasions or scratches on nonvital parts of the body do not often seek medical attention at clinics and hospitals for their management.
Pathophysiology
Abrasions can vary in severity, ranging from a break in the superficial epithelial lining to damage affecting deeper structures, including nerves, blood vessels, muscles, tendons, organs, and even bone.[10][11]
Forensic investigations may be necessary to assess the extent of the injury and the antemortem or postmortem nature of the wound. The presence of vital reactions, such as hemorrhage, cell infiltration, and granulation tissue, provide valuable indicators of the antemortem quality of an abrasion.[12]
Histopathology
While histopathology of abrasions is rarely performed, it can be valuable in determining the healing stage of the injury. This information can be correlated with the patient's history, particularly in medicolegal cases, to establish the date and time of the injury occurrence. [13]
History and Physical
When evaluating a patient with abrasions, relevant history should be documented, including the time, cause, and mechanism of injury. Gathering additional details related to the factors contributing to the injury is also crucial. Additionally, the patients' tetanus vaccine status should be determined as well.
Abrasions are frequently linked to physical trauma, often due to falls, impacts against hard or uneven surfaces, and the pressure exerted by objects. They are commonly observed with other forms of blunt force trauma, including contusions and lacerations.
While a physical examination of abrasions is essential for treatment, the medicolegal examination holds even greater significance. Abrasions can be found on any body part but are commonly observed on exposed areas such as the head, neck, and extremities. When located on the neck or genitalia, abrasions may have a particular significance that requires further evaluation.
The physical examination of abrasions should include assessing their type, size, shape, color, location, depth, and potential association with other injuries. Assessing for the presence of extraneous material is crucial. Scientifically collecting and evaluating these extraneous materials can yield valuable information for crime scene investigation, establishing a connection between the suspect and the crime.
The systematic management of injuries, for medical and medicolegal purposes, will ensure not just treatment of the injury but also may support potential future legal proceedings. The medicolegal examination is critical when dealing with injuries to the head, neck, and genitalia. Injuries around the genitalia could be vital in identifying cases of sexual violence, while minor injuries over the head and neck may indicate the presence of more serious underlying injuries.
Evaluation
The evaluation of minor wounds begins by determining the mechanism and timing of the injury while also considering the possible presence of a foreign body. A comprehensive visual inspection of the affected area is performed to identify any visible foreign objects. In some settings, radiographs may be necessary to detect radiopaque foreign bodies, while ultrasound can help identify non-radiopaque ones.
If the wound is full thickness, the extent of the abrasion should be determined, including any damage to neurovascular structures, muscles, or tendons. This assessment may involve checking pulses and capillary refills in the area of the wound. A neurological evaluation should also be conducted, encompassing motor and sensory testing. Depending on the nature and location of the abrasion, there may be aesthetic concerns that warrant further evaluation for cosmesis.
The medicolegal investigation may require a biopsy of the abrasion to conduct a histological examination. The histological examination investigates the stage of wound healing to provide an estimate of the time of injury. The wound healing process involves coordinated cellular changes, including bleeding and coagulation, inflammatory response, regeneration, and remodeling. The regeneration process further involves migration and proliferation, while remodeling involves extracellular matrix protein and collagen synthesis and the formation of new parenchymal and connective tissue. These processes are four time-dependent phases:
- Bleeding and coagulation, which initiate immediately
- Inflammation also begins promptly.
- Regeneration commences within days and lasts throughout the primary part of the acute healing phase.
The information may be further augmented by histochemical analysis of inflammatory cells and cell mediators. This analysis can assist in determining the time of injury, providing insights to law enforcement. Histopathology of an injury can provide vital information for any potential investigation.[15][16][17][18]
Treatment / Management
Abrasions are usually uncomplicated and frequently small in size. The first step in treatment is to irrigate the area with water or saline. These abrasions usually heal through primary intention and do not leave any scarring. However, the involvement of a large surface area may lead to healing by secondary intention, resulting in scar formation. This is mainly observed in individuals susceptible to keloid hyperplasia, and intralesional corticosteroid therapy may be considered to prevent keloid formation in these patients.
Abrasions are usually minor injuries that do not require extensive medical intervention. A sponsored study has shown that wet healing, using polyurethane and hydrocolloid plasters, is a more efficient and effective approach to wound healing.[19]
Due to the loss of the protective epidermal layer, abrasions are particularly vulnerable to Clostridium tetani and Staphylococcus aureus infection, particularly in sports-related injuries. Tetanus toxoid immunization should continually be updated if needed. Abrasions should be cleansed and dressed to protect the area against reinjury. Debridement may be necessary, especially if dirt or other contaminants are embedded. Prevention of infection is the primary objective of medical intervention. In cases where there are no known allergies, antibiotic ointments may be applied.
The use of dressings depends on the location and depth of the injury. Systemic antibiotics may be indicated for some patients. However, given the increasing prevalence of antibiotic resistance among various organisms, it is essential to maintain strict follow-up to assess compliance and adherence to the complete treatment protocol. Swabbing and sending the injury for culture and sensitivity analysis may also be necessary to guide appropriate antibiotic therapy.
Facial abrasions are considered more serious due to the increased risk of cicatrization and should be cleaned, debrided, and dressed daily. Dressings may require skin adhesives such as a combination of gum mastic, styrax, alcohol, methyl salicylate, or tincture of benzoin.[20]
Differential Diagnosis
The patient's history and the mechanism of injury often provide important clues for diagnosing an abrasion. The presence of foreign material may offer insights into the cause and nature of the injury. Abrasions occurring over the eyes, including the conjunctiva, may be mistakenly attributed to various ocular conditions, including conjunctivitis, corneal ulcer, and endophthalmitis.[21][22]
During medico-legal examinations, the nature of the abrasion is more important than the severity of the injury. The location of the abrasion may present significant findings and could be a vital piece of evidence. Injuries observed on the neck may suggest an (attempted) homicide case. Similarly, injuries present over the thighs and genitalia could indicate a case of sexual assault.
Prognosis
Abrasions are generally minor injuries that tend to heal within 2 weeks without any resultant scarring. However, in cases of extensive and deep abrasions or if infection occurs, scarring may result. This can be prevented by daily cleaning and dressing. Debridement should be performed to avoid extensive cicatrization.
Complications
Wound infection is a common complication associated with abrasions.[23] Proper wound cleaning is essential. Local antibiotic ointments may be applied to superficial, contaminated wounds. However, systemic antibiotics may be necessary to prevent secondary infections in large and deep abrasions.[24] Weighing the need to prevent infection against increased antibiotic resistance is essential. The patient's tetanus immunization should be assessed and updated as needed.
Extensive and deep abrasions can form wide and persistent scars that may last for months or years. Individuals prone to keloid formation may develop extensive scarring, especially on the chest and shoulders.[25]
The nature and context of abrasions are essential aspects that require adequate attention from clinicians to avoid potential negligence claims. Proper documentation, including photography of the injuries, should be preserved for a specified period.
Deterrence and Patient Education
Abrasions occur due to various causes, ranging from innocuous incidents to grievous injuries. Patients and relatives must be educated about the medicolegal importance of these seemingly inconsequential injuries. Clinicians should also recognize the importance of thorough documentation. In sports, abrasions can be reduced by implementing protective measures such as using protective gear, padding, and appropriate clothing.
Simple abrasions caused by falls can be managed with first aid. Patients and their relatives should receive education on proper first aid procedures, which include cleaning the wound, removing any foreign material, and dressing with a non-adhesive material.
Enhancing Healthcare Team Outcomes
Abrasions are among the most frequently encountered physical injuries. While many are superficial and can be managed at home with simple treatments, healthcare workers will likely encounter patients with abrasions requiring medical attention. It is important to note that abrasions often coexist with other injuries. The presence of abrasions should initiate a thorough investigation, and the abrasions should be managed with clinical and medicolegal considerations.
Emergency medical technicians, trauma nurses, and clinicians may conduct the initial assessment of abrasions. Emergency department and ambulatory care nurses provide direct care and educate patients. Pharmacists may counsel patients regarding over-the-counter and prescription medications for abrasions. Maintaining vigilant monitoring and documentation throughout the care process is essential for clinical and medicolegal case management.
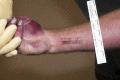
Figure
Parallel, Linear Abrasions of the Ventral Aspects of the Right Wrist Contributed by Andrea L Wiens, DO

Figure
Abrasion caused by sliding fall on concrete Contributed by Wikimedia Commons (Public Domain)

Figure
A patient with bruises and abrasion. Contributed by Depositphotos (Royalty free, non-copyrighted for fair and commercial use)

Figure
A patient with scratch abrasions. Contributed by Depositphotos (Royalty free, non-copyrighted for fair and commercial use)
References
- 1.
- Kramer L, Nadjem H, Glardon M, Kneubuehl BP, Pollak S, Große Perdekamp M, Pircher R. A patterned abrasion caused by the impact of a cartridge case may simulate an atypical muzzle imprint mark. Int J Legal Med. 2016 May;130(3):751-7. [PubMed: 26496804]
- 2.
- Wankhede AG. Patterned injuries caused by wooden plank. J Forensic Leg Med. 2008 Feb;15(2):118-23. [PubMed: 18206830]
- 3.
- Koenig DW, Dvoracek B, Vongsa R. In vitro prediction of in vivo skin damage associated with the wiping of dry tissue against skin. Skin Res Technol. 2013 Feb;19(1):e453-8. [PubMed: 22882623]
- 4.
- Sommers MS. Defining patterns of genital injury from sexual assault: a review. Trauma Violence Abuse. 2007 Jul;8(3):270-80. [PMC free article: PMC3142744] [PubMed: 17596344]
- 5.
- Cavanaugh RM. Self-mutilation as a manifestation of sexual abuse in adolescent girls. J Pediatr Adolesc Gynecol. 2002 Apr;15(2):97-100. [PubMed: 12057532]
- 6.
- Crane J. Interpretation of non-genital injuries in sexual assault. Best Pract Res Clin Obstet Gynaecol. 2013 Feb;27(1):103-11. [PubMed: 23200739]
- 7.
- Boos SC, Rosas AJ, Boyle C, McCann J. Anogenital injuries in child pedestrians run over by low-speed motor vehicles: four cases with findings that mimic child sexual abuse. Pediatrics. 2003 Jul;112(1 Pt 1):e77-84. [PubMed: 12837911]
- 8.
- Gratteri S, Ricci P, Tarzia P, Fineschi V, Sacco MA, Aquila I. When a suicide becomes a forensic enigma: The role of hanging marks and tools of suspension. Med Leg J. 2017 Sep;85(3):141-144. [PubMed: 28849696]
- 9.
- Tiagi C, Walia I, Singh A. Prevalence of minor injuries among underfives in a Chandigarh slum. Indian Pediatr. 2000 Jul;37(7):755-8. [PubMed: 10906808]
- 10.
- Velnar T, Bailey T, Smrkolj V. The wound healing process: an overview of the cellular and molecular mechanisms. J Int Med Res. 2009 Sep-Oct;37(5):1528-42. [PubMed: 19930861]
- 11.
- Alonso JE, Lee J, Burgess AR, Browner BD. The management of complex orthopedic injuries. Surg Clin North Am. 1996 Aug;76(4):879-903. [PubMed: 8782479]
- 12.
- Rivera AE, Spencer JM. Clinical aspects of full-thickness wound healing. Clin Dermatol. 2007 Jan-Feb;25(1):39-48. [PubMed: 17276200]
- 13.
- Robertson I, Hodge PR. Histopathology of healing abrasions. Forensic Sci. 1972 Apr;1(1):17-25. [PubMed: 5054821]
- 14.
- Gantwerker EA, Hom DB. Skin: histology and physiology of wound healing. Facial Plast Surg Clin North Am. 2011 Aug;19(3):441-53. [PubMed: 21856533]
- 15.
- Betz P. Histological and enzyme histochemical parameters for the age estimation of human skin wounds. Int J Legal Med. 1994;107(2):60-8. [PubMed: 7529545]
- 16.
- Fronczek J, Lulf R, Korkmaz HI, Witte BI, van de Goot FR, Begieneman MP, Schalkwijk CG, Krijnen PA, Rozendaal L, Niessen HW, Reijnders UJ. Analysis of inflammatory cells and mediators in skin wound biopsies to determine wound age in living subjects in forensic medicine. Forensic Sci Int. 2015 Feb;247:7-13. [PubMed: 25506669]
- 17.
- Raekallio J. Determination of the age of wounds by histochemical and biochemical methods. Forensic Sci. 1972 Apr;1(1):3-16. [PubMed: 4341073]
- 18.
- Uzün I, Akyildiz E, Inanici MA. Histopathological differentiation of skin lesions caused by electrocution, flame burns and abrasion. Forensic Sci Int. 2008 Jul 04;178(2-3):157-61. [PubMed: 18472235]
- 19.
- Wigger-Alberti W, Kuhlmann M, Ekanayake S, Wilhelm D. Using a novel wound model to investigate the healing properties of products for superficial wounds. J Wound Care. 2009 Mar;18(3):123-28, 131. [PubMed: 19247233]
- 20.
- Lanzi GL. Facial Injuries in Sports, Soft Tissue Injuries (Abrasions, Contusions, Lacerations). Clin Sports Med. 2017 Apr;36(2):287-298. [PubMed: 28314418]
- 21.
- Sliwicki AL, Orringer K. Corneal Abrasions. Pediatr Rev. 2023 Jun 01;44(6):343-345. [PubMed: 37258882]
- 22.
- Meer E, Grob S, Antonsen EL, Sawyer A. Ocular conditions and injuries, detection and management in spaceflight. NPJ Microgravity. 2023 May 16;9(1):37. [PMC free article: PMC10188687] [PubMed: 37193709]
- 23.
- Diaz JH. Skin and soft tissue infections following marine injuries and exposures in travelers. J Travel Med. 2014 May-Jun;21(3):207-13. [PubMed: 24628985]
- 24.
- Chin YK, Ina-Salwany MY, Zamri-Saad M, Amal MNA, Mohamad A, Lee JY, Annas S, Al-Saari N. Effects of skin abrasion in immersion challenge with Vibrio harveyi in Asian seabass Lates calcarifer fingerlings. Dis Aquat Organ. 2020 Jan 16;137(3):167-173. [PubMed: 31942862]
- 25.
- Knowles A, Glass DA. Keloids and Hypertrophic Scars. Dermatol Clin. 2023 Jul;41(3):509-517. [PubMed: 37236718]
Disclosure: Rijen Shrestha declares no relevant financial relationships with ineligible companies.
Disclosure: Kewal Krishan declares no relevant financial relationships with ineligible companies.
Disclosure: Husnain Ishaq declares no relevant financial relationships with ineligible companies.
Disclosure: Tanuj Kanchan declares no relevant financial relationships with ineligible companies.
- [Observations on injuries by blunt objects].[Nihon Hoigaku Zasshi. 2010][Observations on injuries by blunt objects].Terazawa K. Nihon Hoigaku Zasshi. 2010 Dec; 64(2):103-20.
- Evaluation of a liquid dressing for minor nonbleeding abrasions and class I and II skin tears in the emergency department.[J Emerg Med. 2015]Evaluation of a liquid dressing for minor nonbleeding abrasions and class I and II skin tears in the emergency department.Singer AJ, Chale S, Taylor M, Domingo A, Ghazipura S, Khorasonchi A, Bienenfeld A. J Emerg Med. 2015 Feb; 48(2):178-85. Epub 2014 Nov 20.
- Bone abrasions due to the dragging force of a moving vehicle: two unusual case reports.[Arch Med Sadowej Kryminol. 2020]Bone abrasions due to the dragging force of a moving vehicle: two unusual case reports.Keshav Tumram N. Arch Med Sadowej Kryminol. 2020; 70(4):251-256.
- Review Scar-free healing: from embryonic mechanisms to adult therapeutic intervention.[Philos Trans R Soc Lond B Biol...]Review Scar-free healing: from embryonic mechanisms to adult therapeutic intervention.Ferguson MW, O'Kane S. Philos Trans R Soc Lond B Biol Sci. 2004 May 29; 359(1445):839-50.
- Review Children's Abrasions in Recreational Beach Areas and a Review of Possible Wound Infections.[Int J Environ Res Public Healt...]Review Children's Abrasions in Recreational Beach Areas and a Review of Possible Wound Infections.Tomenchok LE, Gidley ML, Mena KD, Ferguson AC, Solo-Gabriele HM. Int J Environ Res Public Health. 2020 Jun 6; 17(11). Epub 2020 Jun 6.
- Abrasion - StatPearlsAbrasion - StatPearls
- Cardiac Glycosides - LiverToxCardiac Glycosides - LiverTox
- Snora9 small nucleolar RNA, H/ACA box 9 [Mus musculus]Snora9 small nucleolar RNA, H/ACA box 9 [Mus musculus]Gene ID:115487884Gene
- LINC00705 long intergenic non-protein coding RNA 705 [Homo sapiens]LINC00705 long intergenic non-protein coding RNA 705 [Homo sapiens]Gene ID:338588Gene
Your browsing activity is empty.
Activity recording is turned off.
See more...