Included under terms of UK Non-commercial Government License.
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
MacPherson H, Vickers A, Bland M, et al. Acupuncture for chronic pain and depression in primary care: a programme of research. Southampton (UK): NIHR Journals Library; 2017 Jan. (Programme Grants for Applied Research, No. 5.3.)

Acupuncture for chronic pain and depression in primary care: a programme of research.
Show detailsIntroduction
A substantial proportion of the global disease burden involves depression,308 which is a major cause of suicide. Depression involves more than just everyday mood fluctuations; it also involves feelings of severe sadness, anxiety, hopelessness and worthlessness. Those affected individuals lose interest in the activities that they used to enjoy and often have physical symptoms such as chronic pain, fatigue and insomnia.
The front-line treatment for depression in primary care usually involves antidepressants; however, they do not work well for more than half of patients.95 Moreover, the effectiveness of newer antidepressants has recently come into question for patients with mild to moderate depression.309 Non-pharmacological treatment options for depression are of interest to many patients, in part because of concerns about dependency on antidepressants.97
Among non-pharmacological treatments, acupuncture and counselling show some promise in the treatment of depression, yet further evidence is needed. A Cochrane review of acupuncture for depression was inconclusive on whether or not acupuncture is an effective intervention for depression, in part because of the high risk of bias in the majority of studies.310 Counselling is a widely used intervention for patients with depression and is provided in approximately half of the 9000 primary care practices in England.311 A Cochrane review of counselling for mental health and psychosocial problems in primary care found short-term but not long-term benefits from counselling.312 Both Cochrane reviews recommended extending the evidence base to include comparisons not just with usual care but also with other interventions, as this would have the potential to increase patient choice.
The aims of this study were to determine the clinical effectiveness and cost-effectiveness of short courses of either acupuncture or counselling compared with usual care for patients with depression. We also planned to compare acupuncture and counselling on the basis that there would be structural equivalence regarding time and attention. Additional exploratory studies nested within the trial focused on (1) the experience of treatment from the patient perspective; (2) the impact of comorbid pain on depression outcomes; (3) the approaches that practitioners use to enhance longer-term benefits; and (4) a health-economic analysis to investigate HRQoL and the costs of these treatments, and understand whether or not they should be considered a good use of limited health resources.
Methods
Design
Patients were randomised by the York Trials Unit to one of three arms in a pragmatic RCT (registration number ISRCTN63787732), as detailed in a published protocol.313 An allocation ratio of 2 : 2 : 1 was used for the randomised groups: acupuncture plus usual care, counselling plus usual care and usual care alone, respectively. The York Trials Unit ensured that the allocation was securely concealed from the researchers who subsequently informed patients of their allocation. The unit recorded patient details prior to using Structured Query Language software for computer-generated block randomisation, with block sizes of five and 10. Randomisation was conducted by an investigator with no clinical involvement in the trial. The York NHS Research Ethics Committee (reference number 09/H1311/75) provided ethical approval on 21 September 2009.
Population
Patients were recruited from a primary care population who had consulted with depression within the past 5 years, who were continuing to experience depression and who were aged ≥ 18 years. We identified potential participants from general medical practice databases. Signed consent forms and baseline questionnaires were returned by patients. Patients were not eligible if they were receiving acupuncture or counselling at the time, had a terminal illness, significant learning disabilities, haemophilia, hepatitis or human immunodeficiency virus infection, were pregnant or had confounding psychiatric conditions (bipolar disorder, post-partum depression, adjustment disorder, psychosis, dementia or personality disorder). Patients who had suffered a close personal bereavement or given birth during the previous 12 months were also excluded. Spoken English was a requirement. Patients were eligible if they scored ≥ 20 on the Beck Depression Inventory-II (BDI-11),314 which is classified within this scale as ‘moderate’ or ‘severe’ depression.
Interventions
Up to 12 sessions were offered, usually on a weekly basis, to patients allocated to the acupuncture or counselling groups. Practitioners providing acupuncture were registered with the BAcC, with at least 3 years of post-qualification experience. In consultation with participating acupuncturists, an acupuncture treatment protocol was developed, which allowed for customised treatments within a standardised theory-driven framework.315 Practitioners providing counselling were members of the British Association for Counselling and Psychotherapy with accreditation or who were eligible for accreditation having completed 400 supervised hours post qualification. Counselling competences using a humanistic approach drawn from those independently developed for Skills for Health316 were incorporated into a manualised protocol. All practitioners recorded in logbooks the number and length of sessions, treatment provided and adverse events. Further details of the two interventions are presented in Appendix 6. In all three patient groups, usual care, both NHS and private, was available according to need and was monitored for all for the purposes of comparison.
Outcome measures
The Patient Health Questionnaire-9 items (PHQ-9)317 at 3 months was the primary outcome measure. We also evaluated the overall impact over the 12-month period. PHQ-9 scores range from 0 to 27, with depression considered mild (5–9), moderate (10–14), moderately severe (15–19) or severe (≥ 20). As a preference-based measure of health outcome, we used the EQ-5D.226 Medication use was ascertained by asking patients if they had taken any prescribed medication for depression or any prescribed analgesics/painkillers. Patients reported health service use, including the number of times that they had consulted a health professional because of their depression. Patients also reported out-of-pocket spending on acupuncture, counselling or psychotherapy, including cognitive–behavioural therapy. Data were collected at baseline and by postal questionnaire at 3, 6, 9 and 12 months. Because these data were self-reported by patients independently of the research team, we minimised potential bias associated with unblinded researchers or clinicians measuring outcomes. We also collected demographic data and patients’ prior preferences and expectations of the interventions at baseline and BDI-II data at baseline and 12 months. We measured patients’ perceptions of their practitioners’ empathy at 3 months using the Consultational and Relational Empathy (CARE) measure14 in both the acupuncture group and the counselling group. A payment of £5 as reimbursement was enclosed with the final questionnaire to enhance the response rate.15
Sample size
We sought an effect size of 0.39 on the PHQ-9 when comparing either acupuncture with usual care alone or counselling with usual care alone, an effect size that was taken to be both moderate and realistic. We used the allocation ratio of 2 : 2 : 1 to increase the power to detect statistically significant differences between acupuncture and counselling. A smaller effect size of 0.32 was sought when comparing acupuncture and counselling, although the anticipated difference between these two treatments was expected to be small and not clinically meaningful. With a two-sided significance level of 5% and 90% power the required group sizes were 204, 204 and 102 in the acupuncture, counselling and usual care alone arms, respectively. The total sample size required was 640 (i.e. groups of 256, 256 and 128 respectively) when allowing for 20% attrition.
Analysis
Primary comparisons were between acupuncture plus usual care and usual care alone, and between counselling plus usual care and usual care alone. A secondary comparison was between acupuncture plus usual care and counselling plus usual care. The PHQ-9 was the primary outcome measure and 3 months was the primary end point, and we used ANCOVA, with baseline PHQ-9 score as covariate. For missing data we used multiple imputation by chained regression using treatment group, baseline measures (PHQ-9, BDI-II, SF-36, EQ-5D anxiety/depression) and demographics (age and sex). We used imputed rather than raw data for the primary analysis to take account of the profile of non-responders.
In a secondary analysis we assessed the overall clinical impact over 12 months, using the AUC method for the PHQ-9 by linear regression, predicting the average AUC while controlling for baseline PHQ-9. We also explored in more detail the PHQ-9 outcomes across all time points using random intercept linear mixed models with fixed effects for treatment arm, time and arm–time interaction for each treatment comparison. The models nested time points within patients and controlled for baseline PHQ-9 score and potential mediators including patients’ prior expectations and preferences regarding the treatments. Potential mediators were identified by univariate regressions (p < 0.1) of the PHQ-9 at 3 months for the whole patient sample, controlling for baseline PHQ-9 score. We controlled for treatment time (combined length of sessions) and quality of attention (CARE score) when comparing acupuncture and counselling. We used ANCOVA to evaluate treatment differences between BDI-II depression scores at 12 months, while controlling for BDI-II baseline scores and covariates for depression as identified above. We used multiple imputation for missing data as for the PHQ-9.
Using an intention-to-treat basis, all analyses were carried out in Stata 12.1. Statistical tests were at a two-sided 0.05 significance level. To assess model assumptions, analysis of residuals was undertaken for all regression models.
Patient and public involvement
In preparation for conducting this research into acupuncture for depression, we conducted a feasibility study that included a prospective case series of 10 patients who received acupuncture treatment for their depression and a focus group with six patients with experience of depression. We used a focus group because as a research team we wanted to learn from patients about their depression and experiences of treatment. We also needed guidance on how best to address the question of whether or not acupuncture is a suitable treatment option for people with depression.
A local patient-centred mental health group, York & District Mind, agreed to work with us on this research and became a long-term partner in its support of research into acupuncture for depression. As a first step we drew on this support in forming a focus group, which met once for 2 hours. Participants in the group were two researchers and six volunteers, identified through York & District Mind, who had experienced depression and were either staff or users of mental health services. A topic guide provided structure for the meeting, covering personal experiences of depression, experiences of both conventional and alternative treatments for depression, and feedback on our research plans. It is the last of these that is most relevant to the patient and public impact on our research.
With regard to feedback on our research plans, participants were concerned about recruitment through GPs on the basis that people who do not consult their GP could not be part of the study. It was agreed that reaching out to those not consulting their GP was a good idea; however, the methods of recruitment would be challenging as there was no way of identifying this hard-to-reach group in sufficient numbers for a RCT.
Another issue raised was to do with the definition of depression amid concerns that there might be some cut-off in severity, for example having a cut-off point so that only people with mild to moderate depression could be recruited. There was a strong feeling among participants that people with severe depression, particularly those who had exhausted all other treatment options, would want to be included in the offer to participate in a trial. The feelings regarding discrimination against mental health users were clearly resonating in this discussion; nobody wanted to be excluded.
This point about not including more severely depressed patients in the trial had a major impact on our trial design when finalising the eligibility criteria. The resulting design included a cut-off to exclude mild depression; however, there was no cut-off for the more severely depressed. This was operationalised with the BDI-II, which we used to recruit patients with both moderate (score of 20–28) and severe (score 29–63) depression. This eligibility requirement led to 62% of patients recruited being categorised as having severe depression and the remaining 38% of patients being categorised as having moderate depression.
York & District Mind continued to be involved with our research into acupuncture for depression. Two lay members and their chief executive joined our independent steering group, which met roughly every 6 months throughout the duration of the trial. Beyond the steering group, their contributions also involved editing the wording in documentation related to the questionnaires that were to be filled in by patients. The chief executive took responsibility for consulting members of his organisation, including users of mental health services, and then aggregated the feedback, which led to improvements in the wording of the questionnaires. Once we had agreed the documentation, and received ethics approval, there was less scope for the York & District Mind participants to contribute, as the trial became primarily a logistic task for the next 3 years. In 2011 York & District Mind merged with another charity called Our Celebration to become York Mind. This change also brought a new chief executive, a transition that took some time to be completed. The new chief executive attended one independent steering committee meeting in June 2011. The combination of this change of personnel and the associated participation gap led to a reduced involvement by patients and the public in the trial from this point on.
Methods for substudy 1: experience of treatment from the patient perspective
The aim of this substudy was to explore patients’ experiences of depression, both with and without comorbid pain, and the perceived changes as a result of receiving the treatments of acupuncture or counselling and usual care. A secondary aim was to report the aspects of treatment that patients reported might have had a positive influence on any long-term change.
In terms of methods, this was a nested qualitative substudy within the Acupuncture, Counselling or Usual Care for Depression (ACUDep) trial. To recruit patients for interview, we selected only from those who had already consented to interview. We used a purposive sampling frame and recruited in the same 2 : 2 : 1 proportions as in the main trial from the treatment groups of acupuncture, counselling and usual care, respectively. We balanced the proportions of men and women and whether or not in pain at baseline. On receipt of their final 12-month postal questionnaire, and based on a sampling frame, a sample of participants who had previously consented to be contacted for an interview was invited to engage in a telephone interview of approximately 30 minutes’ duration. Altogether, 52 people consented to a one-to-one, audio-recorded, semistructured telephone interview for this study.
A researcher (AH) interviewed all participants and all interviews were conducted between February and May 2012. The researcher was unknown to the participants prior to the interview and therefore the interview opened with an introduction designed to set the participant at ease, reveal the context for their depression and draw out their account of treatment received as part of the trial. Prompts from a prepared topic guide were used to elicit the participants’ experiences of depression and treatment. On average, the interviews lasted approximately 25 minutes (range 11–46 minutes). To encourage participants to relax, participants were asked to introduce themselves by speaking about things they like to do or hoped to do and then how depression had entered their lives, before moving on to the research-related questions within the topic guide. Interviews were audio taped, transcribed verbatim and checked for accuracy. All recordings were of sufficient clarity and content that no repeat interviews were necessary. Each transcription was checked to remove any names and was then assigned a participant identification number.
Across the data set of 52 transcribed interviews we used an inductive thematic analysis.318 With a constructivist approach to grounded theory,319 data were analysed initially by AH. Coding was performed sequentially on each transcript by working systematically through the entire data set. Coding and extractions were checked by JE to verify that the participants’ experiences were reflected and summarised accurately. Coding was conducted within each interview and across interviews resulting in themes associated with the experience of depression and further themes associated with the experience of the treatment. Further details of the methods are provided in a separate publication.320
Methods for substudy 2: impact of comorbid pain on depression outcomes
The aim of this substudy was to find out whether people with depression who were also in pain had better or worse depression outcomes than those without pain. We documented the prevalence of pain in this trial population, the demographic profile of patients in pain and the relationship between pain and depression. We determined depression and pain outcomes following treatment with acupuncture or counselling compared with usual care alone. A full report has been published elsewhere.321
In terms of methods, the participants were first divided into two groups according to their response to the EQ-5D pain statements at baseline. People who reported either ‘moderate’ or ‘extreme pain’ were considered together as the ‘pain group’; the remainder were assigned to a ‘no-pain comparator group’.
Analysis of variance (ANOVA) was used to compare the mean baseline PHQ-9 scores between the pain group and the no-pain comparator group. For the pain group alone, a Kendall’s tau correlation was used to test the association between the baseline scores of the PHQ-9 and SF-36 bodily pain score. A series of regression models was applied to determine the influence of baseline pain and other demographic variables on the PHQ-9 depression outcome at 3 months, the primary end point of the trial. To take into account the additional impact of other demographic predictors of PHQ-9 depression at 3 months, a systematic univariate analysis of demographic variables was conducted on the BDI-II depression items and the five EQ-5D items while controlling for PHQ-9 scores at baseline. For this scoping exercise, the level of significance was set at p < 0.1 to maintain consistency with the analysis within the main ACUDep trial. The variables identified by univariate analysis were then included in a linear regression model (p < 0.05); the odds ratios and 95% CIs of the variables identified by the regression models are presented within the results section.
Using any remaining significant predictors and controlling for baseline PHQ-9 depression scores, ANCOVA was used to test if baseline pain affected treatment outcomes measured by the PHQ-9 at 3 months. An interaction term between treatment and pain group in this model was used to establish whether or not patients in pain responded differently to the treatments with regard to their depression from patients reporting no pain. Also, using any remaining significant predictors and controlling for baseline PHQ-9 depression scores, ANCOVA was used to test whether or not baseline pain affected treatment outcome measured by the number of depression-free days at 3 months; an approximate summary measure was derived from PHQ-9 cut-off scores averaged over the period between measurements.322
An ANCOVA model controlling for baseline depression and baseline SF-36 bodily pain was used to assess the impact of treatment for depression on the bodily pain scores at 3 months. Descriptive analysis of the depression and pain scores was conducted over the 12-month follow-up period. Finally, a comparison of the adverse events reported between baseline and 12 months’ follow-up was conducted using proportions and odds ratios.
Methods for substudy 3: approaches that practitioners used to enhance longer-term benefits
The aim of this qualitative substudy was to explore practitioners’ experiences of providing treatment within the trial and to specifically identify the strategies that practitioners reported using to promote longer-term benefits for their patients.
Nested within the trial, this substudy involved in-depth interviews and focus groups with acupuncturists and counsellors who provided treatments to at least two patients within the trial. Our aim was to recruit up to 30 counsellors and acupuncturists (approximately 15 in each group). All participants provided written consent. The interviews and focus groups were informed by topic guides, which were developed by the research team to address the substudy aims. Along with questions, the topic guides also included prompts.
The interviews and focus group were conducted by two experienced health services researchers from the research team who were not involved in the conduct of the trial itself (Liz Newbronner and Ruth Chamberlain). The interviews commonly lasted around 45 minutes (range 40–90 minutes) and the focus group 90 minutes. They were all audio-recorded (with participants’ permission) and transcribed verbatim.
The transcripts were analysed thematically.318 A framework approach facilitated the thematic content analysis, which involved analysing the data across the two groups of practitioners contributing to the study.323 An inductive process was used to identify themes, drawing on shared experiences or points of difference identified from the data. A full report of the methods has been published separately.324
Methods for substudy 4: cost-effectiveness analysis
The main outcome of the cost-effectiveness analysis was the cost per QALY, which takes into account the treatment differences in HRQoL and mortality. HRQoL was measured using the EQ-5D325 at baseline and at months 3, 6, 9 and 12. The cost perspective of the NHS was used, although out-of-pocket expenses were also identified. Using patient questionnaires in the trial, resource use data were collected at 3, 6, 9 and 12 months. The sum of the resource use collected during each 3-month period was used to determine the total annual resource use. The total annual cost was calculated by multiplying the total annual resource use by the unit costs using publicly available 2012 national unit costs (see Appendix 6). We used the costs of acupuncture as estimated previously326 and the average of the ranges reported by NHS Choices:327 £47.50 for an initial session and £37.50 for subsequent sessions. The costs of counselling were those currently used in the NHS: £65 per hour of client contact.291
Multiple imputation methods were used to manage the uncertainty caused by the missing data. Chained imputation using predictive mean matching was undertaken using resource use data, PHQ-9 and BDI scores, QALYs and patient characteristics such as age, sex and education. EQ-5D data were analysed using ordered logit models on each of the five dimensions of the instrument. Analysis at 3 months controlled for the baseline response and analysis over 12 months used random-effects models and controlled for the baseline response and the timing of each response (i.e. the day from randomisation). HRQoL weights on the 0 (equivalent to death) to 1 (full health) scale, including negative values (health states worse than death), were calculated using an independent pre-defined algorithm obtained by the elicitation of societal preferences for the health dimensions in a random population sample through a time trade-off technique.328 QALYs were calculated by applying an individual’s HRQoL weights and the time between EQ-5D measures using the AUC approach.329 For all cost-effectiveness analyses, seemingly unrelated regressions were used to account for the correlation between costs and QALYs.330 QALYs were regressed on baseline HRQoL and treatment arm, and costs were regressed on the treatment arm only. We estimated ICERs using fully incremental analysis.
Using total costs we calculated base-case results taking into account the uncertainty from the multiple imputation and the seemingly unrelated regression. Probabilistic sensitivity analysis was used to reflect uncertainty in mean total costs and QALYs, and we estimated the probability of cost-effectiveness conditional on alternative cost-effectiveness thresholds. Further exploratory scenario analyses were undertaken to understand the influence on cost-effectiveness of (1) the differential cost of the acupuncture and counselling interventions, (2) depression-related resource use, (3) the complete case and (4) a population for whom acupuncture is not appropriate or unavailable. All analyses considered the published NICE cost-effectiveness thresholds of £20,000 and £30,000 per QALY gained.224
Results
Participants
We exceed our recruitment target of 640, recruiting 755 patients in total. Patients registered with 27 general medical practices were recruited between December 2009 and April 2011 in Yorkshire and north-east England. These practices recruited an average of 28 patients (range 0–122 patients). The baseline characteristics of patients were balanced between the trial arms and are presented in Table 34. Notably, baseline expectations of treatment effectiveness were lowest for acupuncture yet, by contrast, a majority (58%) expressed a baseline preference to be allocated to acupuncture. These baseline variations were taken into account in the linear mixed-model analysis. Comparison of baseline data between patients with and without missing data at 3 months is presented in Appendix 6. Figure 26 presents the patient flow in the trial.
TABLE 34
Demographics and variables of interest at baseline

FIGURE 26
Consolidated Standards of Reporting Trials (CONSORT) flow diagram. HIV, human immunodeficiency virus.
Interventions
Of the patients allocated to acupuncture, 266 (88.1%) received one or more treatment sessions (mean 10.3, SD 3.14 treatment sessions) with one of 23 acupuncturists. The average number of sessions received at 3 months was 8.7 (SD 3.34), with 133 patients (50.0%) having completed all of their sessions. Of the patients allocated to counselling, 231 (76.5%) received one or more treatment sessions (mean 9.0, SD 3.74 treatment sessions) with one of 37 therapists. The average number of sessions received at 3 months was 7.5 (SD 3.60), with 114 patients (49.4%) having completed all of their sessions. The mean time from randomisation to last treatment was 117 days in both treatment arms (SD 47.0 and 51.2 days, respectively), a period that included time to first appointment. An average of 13 patients were allocated to each acupuncturist (range 2–45 patients) and an average of eight patients were allocated to each counsellor (range 1–27 patients).
We collected data on acupuncturists’ and counsellors’ self-reports of intervention protocol violations in logbooks. There were reports of four cases of violation of the acupuncture protocol (which incidentally did not involve counselling), one of which was deemed to be a true case involving prescription of a herbal lotion application to reduce swelling and pain. There were seven reports of violation of the counselling protocol, of which two were deemed to be true cases; one case involved goal setting and in another the counsellor reported being analytical and interpretative beyond the scope of humanistic counselling.
Details of all three interventions are provided in Appendix 6, with usual care documented in the following categories: patients seeing health professionals; patients attending hospital accident and emergency departments; patients admitted to hospital; patients paying for private health care. Medication use is detailed later in this chapter. A more complete report on acupuncture provision has been published331 as well as a report reflecting on experiences of providing the counselling.332
Clinical outcomes
For the PHQ-9, unadjusted mean scores at all time points are presented in Table 35 and Figure 27. Table 36 provides the primary outcome results for between-group differences in PHQ-9 depression at 3 months using ANCOVA. With regard to missing data at 3 months, patients for whom no data were available tended to be younger with higher levels of baseline depression. Imputed data were used to take their profile into account. Compared with usual care, patients in the acupuncture arm experienced an average additional reduction in depression of –2.46 points on the PHQ-9 (95% CI –3.72 to –1.21 points; p < 0.001), an observed effect size equivalent to a Cohen’s d of –0.39 (95% CI –0.58 to –0.19). Compared with usual care, patients allocated to the counselling arm experienced an average additional reduction in depression of –1.73 points (95% CI –3.00 to –0.45 points; p = 0.008), equivalent to a Cohen’s d of –0.27 (95% CI –0.47 to –0.07). There was no statistically significant difference between acupuncture and counselling (–0.76 points on the PHQ-9, 95% CI –1.77 to 0.25 points; p = 0.41). These data are conservative as non-imputed data showed slightly larger treatment effects (see Appendix 6).
TABLE 35
Unadjusted depression outcomes

FIGURE 27
Unadjusted PHQ-9 mean scores from baseline to 12 months.
TABLE 36
Effect of trial arm on PHQ-9 depression
In the AUC analysis over the 12-month period, the statistically significant benefit of acupuncture and counselling over usual care alone in terms of PHQ-9 score reduction seen at 3 months remained: acupuncture reduced the PHQ-9 score by –1.55 (95% CI –2.41 to –0.70) and counselling by –1.50 (95% CI –2.43 to –0.58) (see Table 36).
In a secondary analysis exploring potential mediators, PHQ-9 scores at 3 months were found to be associated with two factors: expectations of counselling (p = 0.064) and expectations about the treatment that patients were allocated to (p = 0.015). These factors were included as potential mediators of the effect of trial arm in further analyses. Related to the comparison of the acupuncture and counselling arms, additional significant factors were total session time at 3 months (p < 0.001) and perceived empathy of practitioners (p < 0.001), which were added as further covariates.
From the linear mixed modelling, PHQ-9 depression scores in the acupuncture and counselling groups were reduced compared with usual care at 3 and 6 months (see Table 36). The scores in the usual care group continued to reduce over time, such that differences were no longer statistically significant at 9 and 12 months. There was no evidence of significant differences between acupuncture and counselling throughout.
Using ANCOVA, depression scores on the BDI-II were found to be reduced in the acupuncture arm (–2.88, 95% CI –5.68 to –0.08) and the counselling arm (–2.74, 95% CI –5.50 to 0.02) to a greater extent than by usual care alone at 12 months, but with no statistically significant difference between acupuncture and counselling (Table 37).
TABLE 37
Effect of trial arm on BDI-II depression
Prescribed medication
Among all patients, the majority (68.7%) were taking antidepressants at baseline (Table 38) and prescribed antidepressant utilisation decreased steadily by an average of 12% over the 12-month study period, a rate comparable between trial arms. Around half of patients (47.9%) were taking analgesics at baseline, which decreased on average to 41.0% over 12 months. Patients in the acupuncture arm showed a marked decrease in the use of analgesics in the first 3 months.
TABLE 38
Numbers of patients taking prescribed medication in the preceding 3 months
Adverse events
Over the 12 months, the number of patients experiencing a serious adverse event, as judged by a clinician (IW), was 16 out of 302 (5.3%) in the acupuncture group, 26 out of 302 (8.6%) in the counselling group and nine out of 151 (6.0%) in the usual care group, of whom nine had more than one serious adverse event (range 2–4). None of the serious adverse events, including three deaths, was known to be related to treatment. Over the 12 months, the number of patients experiencing a non-serious adverse event was 56 (18.5%), 47 (15.6%) and 40 (26.5%), respectively, of whom 17 had more than one non-serious adverse event (range 2–4).
Results for substudy 1: experience of treatment from the patient perspective
Of the 61 participants invited, four declined participation and three did not respond; in addition, two recordings failed for technical reasons. In total, 52 participants, 24 men and 28 women, with an age range of 22–89 years (mean 46 years, SD 13.8 years), were interviewed. At baseline, 26 of these participants had reported having moderate or extreme pain or discomfort on the EQ-5D questionnaire; these people formed the pain group, with the remainder forming the no-pain comparator group. As part of the ACUDep trial, 22 of the 52 had been randomised to receive acupuncture, 20 had been randomised to receive counselling and 10 had been randomised to receive usual care alone. A summary is presented in the sampling frame in Appendix 6. On average, those allocated to acupuncture attended 11 sessions (range 4–12 sessions) and those allocated to counselling attended 10 sessions (range 6–12 sessions).
Participants’ experiences of depression varied considerably between those with comorbid pain and those with depression alone. Those participants with depression and comorbid pain commonly experienced a number of other physical symptoms concurrently such as fatigue, low energy and sleep problems. For some this meant withdrawing from social and day-to-day activities. This reduced ability to engage in social activity was one of the factors that led to this group having less in the way of internal and external resources available to manage their depression effectively. The majority in the no-pain comparator group were in full- or part-time employment, or were relatively affluent retired professional people. For many, their experience of depression concerned feelings of low self-esteem brought about by high expectations of themselves within their working life or hectic social schedules.
Those with physical symptoms who were receiving acupuncture commonly reported that these broader symptoms were usually addressed as part of the treatment. As treatment progressed, many participants reported that their acupuncturist began guiding them to make changes to their lifestyle to engender beneficial long-term outcomes. For most people with pain, fear of pain and potential injury posed a barrier to engaging in physical activity. Nevertheless, the majority of the pain group reported being encouraged to take up gentle exercise for their overall health. The advice given to the no-pain comparator group more often focused on dietary change and a reduction in caffeine and alcohol intake, as well as encouragement of some form of relaxation. Overall, longer-term improvement in depression was developed through the participants’ active engagement in health-promoting behaviours, supported by a positive therapeutic relationship.
For those receiving counselling there was less emphasis on physical symptoms and more on help with gaining an understanding of themselves and their situation. Despite many having low expectations of counselling based on their previous experiences, the majority of participants engaged with the counselling process. Most reported feeling relieved to have someone to talk to in confidence. For both the pain and the no-pain groups, the process of change followed a common pathway, beginning with the participants’ disclosure of personal information and being listened to and leading to an exploration of their past, which helped to clarify their understanding of themselves and their situation. The final stage in the process of change for many was directed towards enabling them to maintain their progress and recovery independently.
In summary, longer-term change was encouraged by most practitioners over the course of treatment. This was facilitated by strong support to cope with depression and pain independently of treatment, with a focus on relevant lifestyle and behaviour changes. Participants identified as important components of treatment the therapeutic relationship with their practitioner and their active engagement in the treatment process, whether they were receiving acupuncture or counselling, A full report on the experiences of treatment has been published separately.320
Results for substudy 2: impact of comorbid pain on depression outcomes
Patients reporting moderate and extreme pain or discomfort on the EQ-5D questionnaire were merged together to form a single pain group (n = 384, 51%) with the remainder forming the no-pain comparator group (n = 371, 49%). A summary of the demographic variables in the subgroups allocated to the pain and no-pain groups at baseline is presented in Appendix 6. The variables were comparable for most items with the following notable exceptions: (1) the pain group members tended to be older than the no-pain comparator group members (mean 47 years vs. 40 years); and (2) in terms of health and employment, 56% of the pain group (vs. 9% of the no-pain group) reported a painful health condition or illness that predated the onset of depression, for which 64% (vs. 31%) used analgesic medication regularly, and 32% (vs. 9%) were unable to work or were retired.
The baseline PHQ-9 depression scores indicate that the pain group reported higher levels of depression at baseline (mean 17.0, SD 5.2) than the no-pain comparator group (mean 14.9, SD 5.2). Results of the ANOVA confirmed the difference to be highly significant (mean difference 2.02, 95% CI 1.28 to 2.76). For the pain group alone, the correlation between the PHQ-9 scores and SF-36 bodily pain scores was weak but highly significant (Kendall’s tau –0.172; p < 0.001).
Using the average across all treatment groups, participants in the pain group showed a smaller reduction in depression score at 3 months compared with baseline (mean reduction from 16.70 to 12.06 at 3 months) than the no-pain comparator group (mean reduction from 14.06 to 9.10 at 3 months). A linear regression model found that the presence of moderate or extreme pain at baseline predicted a poorer outcome of depression treatment at 3 months (mean difference –1.72, 95% CI –2.64 to –0.80; p < 0.001) when controlling for baseline depression scores. An ANCOVA model controlling for significant predictors and baseline PHQ-9 score revealed that the effect of pain group remained significant, with patients with baseline pain having poorer depression outcomes (mean difference –1.16, 95% CI –2.2 to –0.12; p = 0.028).
Regarding PHQ-9 depression scores by pain group and by trial arm at baseline and all follow-up time points, relevant data are shown in Figure 28. Controlling for baseline depression and covariates, an ANCOVA model including a pain group–treatment interaction term showed that, in the pain group, participants showed a larger reduction in depression with acupuncture at 3 months (mean reduction in PHQ-9 score from baseline 6.0, 95% CI 5.07 to 7.11), with smaller reductions associated with counselling (mean reduction 4.3, 95% CI 3.3 to 5.4) and usual care (mean reduction 2.7, 95% CI 1.50 to 4.06). In comparison, no notable differences were seen between treatment arms within the no-pain comparator group.

FIGURE 28
Mean PHQ-9 scores by treatment, comparing the pain and no-pain groups: (a) patients with moderate to extreme pain at baseline (n = 384); and (b) patients pain free at baseline (n = 371).
Using the SF-36 bodily pain score at 3 months’ follow-up as the end point, and controlling for baseline SF-36 bodily pain and baseline PHQ-9 depression scores, the results of the ANCOVA show that the pain group continued to experience significantly worse pain after treatment for depression compared with the no-pain comparator group (mean difference 14.57, 95% CI 9.73 to 19.40). There was also a significant interaction between pain group and treatment arm (F2,1 = 3.3; p = 0.036), with pain group patients who received acupuncture for depression experiencing a greater reduction in SF-36 bodily pain (represented by an increase in scores) between baseline and 3 months’ follow-up (mean reduction 11.2, 95% CI 7.1 to 15.2) than those who received counselling (mean reduction 7.6, 95% CI 3.6 to 11.6) or usual care (mean reduction 7.2, 95% CI 2.3 to 12.1). The reduction in pain at 3 months persisted through to the 12-month follow-up point (Figure 29); however, the median score in the pain group after 12 months (median 41, interquartile range 1 = 31, interquartile range 3 = 62) remained below the trial baseline median score of 52 on the SF-36 bodily pain scale. Further details of the results have been published separately.321
Results for substudy 3: approaches that practitioners used to enhance longer-term benefits
Forty-one therapists consented to be involved in the study but five therapists later withdrew or did not respond when the fieldwork was being set up. The substudy included individual telephone interviews with 15 counsellors and 13 acupuncturists (n = 28), and one focus group with four counsellors and four acupuncturists (n = 8) (see Appendix 6). The sample for the qualitative substudy included over half (56%) of the total number of therapists involved in the main trial. The 17 acupuncturists were predominantly male (39% were female), with an average duration of practice of 12 years. In the trial they treated on average nine patients, who attended on average for 10 sessions. The 19 counsellors were predominantly female practitioners (79%), with an average duration of practice of 7 years. In the trial they treated on average seven patients, who attended on average for nine sessions.
A cluster of eight themes emerged from the framework analysis. Almost all of the acupuncturists and counsellors stressed the importance that they attached to promoting longer-term benefits.
- Importance of a long-term focus. Almost all of the practitioners mentioned the long-term perspective as inherent to the way they worked. For longer-term impact, both acupuncturists and counsellors encouraged insight into root causes of depression on an individual basis and saw small incremental changes as precursors to sustained benefit.
- Identifying root causes. The commitment to identifying and addressing the root causes of depression within the treatment process was a commonly expressed factor among both acupuncturists and counsellors. Acupuncturists commonly used the theoretical concept of ‘root’ (ben) and ‘branch’ (biao). The counsellors were more interested in ‘going deeper’ and ‘further back (in time)’ with their clients as a way of getting to the root causes.
- Individualisation. When practised within the theoretical framework of traditional Chinese medicine, acupuncture treatment has been customised to the individual, such that treatment varies not only between patients but also, for the same patient, over time. Likewise for the counsellors in the trial, all of whom were committed to working within the humanistic tradition, a person-centred approach was provided.
- Valuing incremental change. Practitioners reported that they did not expect change to happen all at once. Rather than seeking cathartic experiences, ideally improvement in symptoms would develop slowly with small incremental changes.
- Addressing concurrent physical symptoms. Acupuncturists generally stressed the importance of addressing concurrent physical symptoms, for example helping patients relax or sleep better to be more receptive to change. Counsellors were less focused on the physical symptoms and worked more on the assumption that by treating the underlying causes of depression there should be a knock-on effect in terms of reducing physical symptoms.
- Lifestyle changes. Acupuncturists tended to highlight the importance of giving advice about lifestyle change that was relevant to the Chinese medicine perspective. By contrast, the counsellors had a more non-directive style, consistent with the humanistic tradition.
- Therapeutic relationship. More often than the acupuncturists, the counsellors stressed the importance of the therapeutic relationship as a facilitator of change.
- Careful ‘pacing’ based on ‘readiness to change’. Many of the counsellors also emphasised the need for careful ‘pacing’ such that the processes and tools that they employed were tailored and timed for each individual, depending on the ‘readiness’ to change. A number of acupuncturists reflected on the best way of sustaining benefit over the longer term, suggesting that ideally appointments should be spread out towards the end of the course of treatment and beyond.
The above themes capture both similarities and differences in approaches between acupuncture and counselling, with most practitioners of both interventions having a shared sense of the prerequisites for sustained long-term benefit. The impression formed from the interviews is that the various approaches do not operate in isolation. The themes appear to be integrated into a coherent combination that uniquely informs the practice of each practitioner, although the emphasis may vary. A full report of the results has been published separately.324
Results for substudy 4: cost-effectiveness analysis
At 3 months patients treated with acupuncture or counselling were less likely than patients treated with usual care to report that they were moderately or extremely anxious or depressed rather than not anxious or depressed (Table 39). The 3-month improvement in anxiety and depression was sustained over the trial period to 12 months. Combining the EQ-5D dimension results with the UK population health state preferences resulted in the HRQoL scores over time and by treatment presented in Figure 30. For all treatment arms HRQoL increased between baseline and 3 months, with the acupuncture and counselling arms having a higher HRQoL than usual care and remaining higher at 12 months. QALYs were estimated to be 0.604, 0.663 and 0.666 for the usual care, acupuncture and counselling arms, respectively, using imputed data and seemingly unrelated regression and controlling for baseline HRQoL.
TABLE 39
EuroQoL-5 Dimensions data: the proportional odds of being at level 2 or 3 compared with level 1 – comparing acupuncture or counselling with usual care
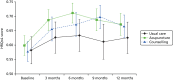
FIGURE 30
Health-related quality-of-life scores over time and by treatment.
Mean NHS resource use is reported in Table 40. Total costs and depression-related costs are reported in Table 41. Patients reported the amount spent on out-of-pocket acupuncture, counselling or usual care. Patients in the acupuncture arm reported spending a mean of £32 (SD £93) on acupuncture, whereas those in the counselling and usual care arms reported spending £7 (SD £41) and £6 (SD £57), respectively. Patients in the counselling arm reported spending a mean of £42 (SD £173) on counselling, whereas those in the acupuncture and usual care arms reported spending £6 (SD £42) and £5 (SD £32), respectively. Patients spent on average £2 (SD £33), £15 (SD £87) and £3 (SD £23) on psychotherapy in the acupuncture, counselling and usual care arms, respectively. The mean number of days off work over 12 months was similar across arms: 238 (SD 115), 240 (SD 112) and 231 (SD 113) for the acupuncture, counselling and usual care arms, respectively.
TABLE 40
Complete case and imputed resource use over 12 months
TABLE 41
Complete case and imputed costs over 12 months
When comparing acupuncture, counselling and usual care, acupuncture was found to be the cost-effective alternative with an ICER of £4560 per additional QALY compared with usual care alone, with probabilities of being cost-effective of 0.68, 0.62 and 0.56 at thresholds of £13,000, £20,000 and £30,000 per QALY, respectively (Table 42). Counselling resulted in higher costs and benefits than acupuncture, with an ICER of £71,757 per additional QALY compared with acupuncture.
TABLE 42
Incremental cost-effectiveness of usual care, acupuncture and counselling
In a scenario analysis which assumed that each session of acupuncture was the same price as each session of counselling (£65), counselling had higher QALYs and lower costs than acupuncture, that is, acupuncture was dominated (Table 43). Restricting the analysis to the complete case data resulted in an ICER for acupuncture of £10,979 per QALY and counselling having higher costs and lower QALYs than acupuncture. For patients in whom acupuncture is inappropriate or unavailable, the incremental cost-effectiveness of counselling compared with usual care was £7935 per additional QALY.
TABLE 43
Incremental cost-effectiveness scenario analyses
Discussion
Principal findings
For patients continuing to experience depression in primary care, we found statistically significant benefits at 3 months associated with both acupuncture and counselling interventions when provided as adjuncts to usual care. Prior to recruitment to the trial, these patients experienced recurring bouts of depression (76% having had four or more episodes), with the first episode on average occurring at age 25 years, some 19 years previously, and 69% were on antidepressant medication. We also found statistically significant benefits for patients over the 12-month period as a whole in an AUC analysis. At 12 months the benefits of acupuncture and counselling were no longer significantly better than those of usual care for our primary outcome measure, the PHQ-9, but statistically significant differences remained when depression was measured by the BDI-II. No serious adverse events related to treatment were reported.
Strengths and limitations
This study design of a pragmatic RCT had a clear and practical research question with an appropriate trial design to model closely what would happen if patient referrals to acupuncturists and counsellors were routine. With an emphasis on external validity, our pragmatic trial was designed to have findings that are generalisable to typical patients and settings. We recruited patients in primary care from among those who had consulted with depression and who continued to be depressed, thereby excluding patients whose symptoms had been alleviated sufficiently by other treatment.
The attrition of patient-reported data between randomisation at baseline and the follow-up time-points was typical of trials that recruit through primary care databases. We used multiple imputation to compensate in part for the limitations related to the loss of follow-up data. Our design controlled for temporal effects, such as the natural history of depression, and other factors across all patients that might have influenced outcomes beyond the treatment itself through the randomisation into groups. The standardised treatment protocols for the acupuncturists and counsellors were designed to reflect routine practice, allowing individualisation to match patient variability while ensuring that all practitioners met appropriate standards of qualification and experience. No attempt was made to standardise usual care; however, we were careful to document the usual care that was provided to patients in all arms of the trial. The majority of patients continued with antidepressants and differences between groups in usual care at all time points were minimal (see Appendix 6). For this reason we can assume that the differences in outcomes between arms can largely be ascribed to the treatments provided by the acupuncturists and the counsellors.
Our study was not designed to determine which aspects of the interventions might be most or least beneficial. In contrast to pragmatic trials, explanatory trials are designed to separate out the relative contributions of specific or non-specific components of treatment. Nevertheless, we took into account in our regression model the expectations and preferences reported by all patients in the trial, components that are often considered non-specific effects. Moreover, for two treatment-related components in the acupuncture and counselling groups of our trial that are often considered ‘non-specific’, namely session time and quality of therapist attention, we found that specific treatment effects remained when these were accounted for. Despite the limitation that a pragmatic approach has in ascribing outcomes to different treatment components, a pragmatic trial design provides a useful estimate of the overall effect, an estimate of most interest to patients, practitioners and providers.
Relationship to the literature
In a recent Cochrane review of acupuncture for depression,310 no studies focused on the BDI-II-related categories of moderate to severe depression, unlike patients in our trial who, for eligibility, had to have a score of ≥ 20 on the BDI-II. Moreover, only two trials in the Cochrane review, by the same research team, used a usual care comparator, which was based on a wait list.333,334 A meta-analysis of these two trials involving 94 patients showed a reduction in the SMD of –0.73 (95% CI –1.18 to –0.29).310 This is a larger effect size than we found (we found a point estimate of –0.39); however, we need to be cautious in the interpretation of the result, as the patients in these studies were less depressed and the patient numbers were small.
From a Cochrane review of counselling for mental health and psychosocial problems in primary care,312 there is evidence from six trials of counselling for mild to moderate depression including 772 patients that counselling is more effective than usual care in terms of mental health outcomes over 1–6 months (SMD –0.28, 95% CI –0.43 to –0.13). These advantages were not shown to endure over the longer term from 7 to 12 months (SMD –0.09, 95% CI –0.27 to 0.10). Their number needed to treat for short-term benefit was six, somewhat less than the 10 we found for moderate to severely depressed patients. We found no counselling trial equivalent to the one that we report here, namely one based in primary care that evaluated counselling for moderate to severe depression. In a review of psychological interventions for depression, four cognitive–behavioural therapy studies based in primary care covering 259 patients found a similar short-term effect (SMD –0.33, 95% CI –0.60 to –0.06).335
In this report we present the first evidence on acupuncture and counselling for patients in primary care who are representative of those continuing to experience symptoms of moderate to severe depression. At 3 months, which is approximately at the end of the course of 12 treatment sessions, both acupuncture and counselling were shown to be effective treatments compared with usual care alone. There was also evidence that there are benefits over the 12-month period in terms of clinical symptoms.
Implications for clinical practice
To interpret the results for clinical practice, we found that 33% of acupuncture patients, 29% of counselling patients and 18% of usual care patients achieved a successful treatment outcome when this is defined as improvement from a depressed PHQ-9 score (≥ 10) to a non-depressed score (≤ 9), with an improvement of at least 50%.336 These percentages apply to the total number of patients with a baseline PHQ-9 score of ≥ 10 and for whom data were available at 3 months. The number needed to treat is also a useful way to interpret results. We found that for one additional treatment success, as defined above, the number needed to treat was 7 for acupuncture (95% CI 4.3 to 17.4) and 10 for counselling (95% CI 5.3 to 47.3). A further illustration of the impact on patient experience can be provided in terms of ‘depression-free days’,322 which is a summary measure derived from PHQ-9 cut-off scores averaged over the period between measurements. The mean number of depression-free days over 3 months was 34 (95% CI 31 to 38) for the acupuncture group, 27 (95% CI 24 to 30) for the counselling group and 23 (95% CI 19 to 27) for the usual care group.
We used the BDI-II as a screening tool, with patients having to score ≥ 20 for eligibility, a score that is classified by this measure as moderate or severe depression. Other classification systems, such as the Diagnostic and Statistical Manual of Mental Disorders [see www.psychiatry.org/psychiatrists/practice/dsm (accessed 13 October 2016)], have different categories of severity. Our trial did not determine whether acupuncture or counselling performed better or worse for the more mild forms of depression. Our trial also did not determine whether or not patients not receiving antidepressant medication (one-third of our sample) do better or whether fewer sessions would be sufficient for mild to moderate depression or more sessions would improve outcomes for those with severe depression (approximately 60% of our sample). It is not clear from our trial whether or not there was any impact on outcomes because, for those allocated to acupuncture, it was usually their first experience of this intervention, whereas for many randomised to counselling, it was an intervention they had received before.
Discussion for substudy 1: experience of treatment from the patient perspective
Patients commonly reported that their acupuncturists appeared to have a more physical perspective on treatment, with a focus on directly relieving the symptoms of depression as well as concurrent physical symptoms. This was particularly welcomed by patients who reported comorbid pain at baseline, who appreciated having their physical symptoms treated alongside their depression. In conjunction with the acupuncture sessions, the acupuncturists often helped patients engage in health behaviours that had a positive influence on long-term change. In contrast, patients typically reported that their counsellors helped them identify and confront underlying causes of depression and then helped them find their own way forward. For both treatment modalities, most participants reported that the establishment of a therapeutic relationship and their active engagement as patients helped them develop coping strategies, which in turn helped them be more effective in reducing their depression in the longer term.
These qualitative findings are concordant with, and supplement, the quantitative data on depression and comorbid pain within the trial.321 Notably, the patients with moderate or extreme pain at baseline (as reported on the EQ-5D) had worse outcomes at 3 months for depression than the no-pain comparator group in all three treatment arms. Our findings extend the findings of the trial’s quantitative data in two ways. First, there are identifiable differences in the experiences of depression when comorbid pain is present. Second, acupuncture appears to involve an approach that more directly addresses physical symptoms, including the comorbid pain, whereas counselling more directly addresses the underlying psychological causes of depression, which may or may not be linked to comorbid pain.
Our study has some limitations. Participants may have attributed changes directly to treatment rather than concurrent, coincidental contextual changes. We accept that there is a possibility of recall bias as it has long been known that there is a significant, stable association between depression and memory impairment,337 which may have altered what was recalled and how it was recalled. The lack of face-to-face contact during the telephone interviews prevented the interviewer gathering non-verbal contextual information, such as social cues, body language, appearance and setting, to supplement the verbal answers of the interviewees. A full report of the discussion related to this substudy has been published separately.320
Discussion for substudy 2: impact of comorbid pain on depression outcomes
Participants with moderate to extreme pain at baseline had worse outcomes for depression than the no-pain comparator group in all three treatment arms after controlling for baseline depression. Participants in the pain group had greater reductions in depression symptoms with acupuncture from baseline to 12 months than those who received counselling or usual care, whereas those who were pain free did relatively well whichever group they were assigned to. Participants in the pain group receiving acupuncture found that their pain reduced markedly in the first 3–6 months compared with those in the other two groups, but by the end of the 12-month trial these differences disappeared. It should be noted that this study, as a substudy of a larger trial, was not powered to detect differences between the subgroups with moderate to extreme pain and no pain.
The estimated prevalence of moderate to extreme pain within our study population of depressed patients was 51%, which is comparable to the 50% identified in previous literature.92 Evidence from an English longitudinal study of ageing identified pain and mobility disability at baseline as predictors of comorbid pain and depression.338 In a large European study, a higher number of pain locations, pain of the joints and longer duration of pain (for ≥ 90 days), daily use of pain medication and more severe pain at baseline were found to be associated with a significantly increased risk of still having a depressive or anxiety disorder after 2 years.338 Together, these factors are known to adversely affect the outcomes of treatment for depression.338 Consistent with previous research, the majority of painful complaints within the study sample were of musculoskeletal origin and accompanied by poor mobility and a loss of energy. Pain from osteoarthritis is known to determine subsequent depressed mood through its effect on fatigue and disability.339
That patients reported reduced pain following acupuncture is not surprising given that 32% of patients had chronic musculoskeletal pain and acupuncturists within the trial were encouraged to work how they normally would, incorporating treatment for pain alongside treatment for the symptoms of depression. Moreover, there is a growing body of evidence supporting the efficacy of acupuncture for chronic pain.196 Patients who received counselling reported a more gradual reduction in pain over the 12-month follow-up period. This finding is consistent with a Cochrane review340 which reports that psychological therapies, primarily cognitive–behavioural therapy, can help people with chronic pain reduce negative mood (depression and anxiety), disability and, to a lesser degree, pain over a 6-month period.
Frequently patients with comorbid pain and depression will attribute their condition to one or other of these two symptoms and seek help accordingly.341 For treatment success, our trial provides some evidence that both pain and depression should be both recognised and treated from the outset. Overall, the evidence emerging in the current study is that both acupuncture and counselling appear to have the potential to reduce symptoms associated with pain and depression when treated concurrently, with the potential to relieve symptoms of depression and reduce the intensity of pain in both the short and the longer term. Further discussion related to this substudy can found elsewhere.321
Discussion for substudy 3: approaches that practitioners used to enhance longer-term benefits
Encouraging longer-term change was integral to the work of both acupuncturists and counsellors. Although both types of practitioners reported on the need to address the root causes, the approach differed. For the acupuncturists there was a focus drawn from Chinese medicine theory on treating the root cause as well as the manifesting symptoms, with the precise details of the intervention customised to their patients at an individual level. By contrast, the approach of the counsellors was to get below the surface of the clients’ problems and to ‘go deeper’ and ‘further back (in time)’ as a way of getting a handle on the root cause. For both types of practitioners, this required an individualised approach.
Further differences in approach to facilitating more sustained benefits were noted, in that acupuncturists were more focused on physical symptoms, on whether or not these could be resolved by acupuncture to speed up the improvements in the symptoms of depression and on providing lifestyle advice linked to the Chinese medicine diagnosis. Meanwhile, counsellors were more explicit about the importance of a strong therapeutic relationship accompanied by a careful consideration of what might be a manageable pace of change.
The methods used in this substudy, involving interviews and focus groups with verbatim transcripts and thematic analysis, were consistent with many of the markers of quality in qualitative research.342 By involving an independent research team, we have helped establish the credibility and dependability of the results. With regard to the transferability of the results, we have provided details of the practitioners as well as the patients who were the focus of this substudy, such that readers can draw conclusions regarding relevance for other areas. In terms of limitations, our data are limited to patients receiving acupuncture as practised by those using the theories of traditional Chinese medicine and to clients receiving counselling as provided in the humanistic and non-directive and person-centred style.
Within the wider literature there is a dearth of evidence on the acupuncture treatment factors that might be associated with longer-term change in the symptoms of depression. The findings from a small study involving interviews with six practitioners in a trial of acupuncture for back pain found that these acupuncturists had a goal of a positive long-term outcome and developed a therapeutic partnership to support the active engagement of patients in their own recovery.343 Consistent with some of the findings we report here, the authors reported that the key elements were establishing a rapport, using an interactive diagnostic process, matching treatment to the patient and using explanatory models from Chinese medicine to aid a shared understanding and motivate lifestyle changes to reinforce the potential recovery.343
There is also limited evidence in the counselling literature from qualitative studies on the factors that improve the long-term effects of counselling. One report contains client interview data drawn from 15 clients who had received counselling from between 1 and 3 years previously.344 The authors’ interpretation of the interview data led them to describe a model of the change process and mechanisms that were perceived as essential to produce a lasting benefit. They identified as key elements of the counselling process the active engagement of the client during and between sessions, and the acquisition of a ‘box of skills’ to be built on further after the counselling was finished.344 A full report of the discussion related to this substudy has been published separately.324
Discussion for substudy 4: cost-effectiveness analysis
This economic analysis demonstrated that the HRQoL results are consistent with the clinical results. The cost-effectiveness results, taking into account the uncertainty in the estimates, suggest that acupuncture is the cost-effective option. In the base-case analysis, acupuncture had an ICER of £4560 per additional QALY and was cost-effective with a probability of 0.62 at a cost-effectiveness threshold of £20,000 per QALY.
Currently, acupuncture for depression is not provided by the NHS. To understand the cost-effectiveness of counselling in a population for whom acupuncture is not appropriate (e.g. those who are needle phobic), a scenario analysis of counselling compared with usual care, excluding acupuncture as a comparator, was undertaken. In this population counselling had an estimated ICER of £7935 and a 0.91 probability of being cost-effective.
It is possible that the regulation of acupuncture may increase the per-session costs. A sensitivity analysis was undertaken assuming that each acupuncture session costs £65, the same as the cost of counselling. In this scenario counselling was preferred to acupuncture because not only were the expected benefits higher but the expected costs were lower. This demonstrates that the cost-effectiveness of acupuncture in this study is reliant on it having a lower cost than that of counselling.
Recommendations for future research
Further research could usefully identify the optimal populations for acupuncture and counselling. It would also be useful to explore the impact of different recruitment methods on the characteristics of those recruited. For example, patients recruited at the point of consultation will be different from those recruited through databases, as we did in this trial, and different again from those with depression who do not consult their GP at all. What was important in the trial that we report here was that all patients had consulted in primary care, all continued to be depressed and all were seeking other interventions that might reduce their depression. Other recruitment methods could be used, for example to assess whether the interventions would be more effective for patients at the time of consulting their GP or for patients who were experiencing their first episode of depression, rather than after many episodes, as was the case in the present study, in which 76% of participants had four or more previous episodes, or for patients who have given up consulting in primary care yet continue to be depressed.
Further research into optimal treatment regimens would also be useful. With regard to acupuncture provision, there is some evidence from the literature that a uniform combination of points can work for depressed patients.345,346 However, a large-scale head-to-head trial or extensive synthesis in an IPD meta-analysis would be required to determine if a uniform approach for all acupuncture provision might be more beneficial than a style of acupuncture in which treatment is individualised for each patient and with changes over time, as was the case with the trial that we report here.
Although our findings are that both acupuncture and counselling for depression appear to be associated with longer-term benefits, it would be useful to explore the different ways that the interventions work. For example, we found that acupuncturists include in their treatment of patients with depression a focus on physical symptoms, yet it is not clear how important this is for outcomes related to depression. Further research is needed into the patient perspective on the treatment of depression with comorbidities and specifically the value that patients place on their comorbid symptoms being addressed concurrently. Further research is also needed from the perspective of patients on their experiences of treatment from these two modalities. To assist referral, a clearer understanding is needed of which type of person with depression would benefit from acupuncture and which from counselling. When taking into account patient preference, such a typology would provide referring clinicians with valuable guidance on suitability for referral.
Further analyses are needed to explore variations in the time horizon and the related impact on the cost-effectiveness of acupuncture and counselling. In this trial patients were followed up for 12 months and our analysis considered only this 12-month time frame, which assumed no differences between treatment arms beyond 12 months. This is a conservative assumption as there would be no further intervention costs, but our trial results suggest that a continued difference in treatment outcomes after 12 months is plausible, even though these treatment differences seem to be converging (see Figure 30). Extrapolating these differences beyond 12 months would result in a lower ICER for acupuncture. Further evaluation of the cost-effectiveness of acupuncture and counselling when compared with other physical and psychological interventions as well as with different levels of usual care will provide a better understand of how to best allocate scarce health-care resources.
Conclusion
In this report we present what is to our knowledge the first study to rigorously evaluate the clinical and economic impacts of acupuncture and counselling for patients who are representative of those who continue to experience depression in primary care. Our evidence on acupuncture compared with usual care and counselling compared with usual care shows that both treatments are associated with a statistically significant reduction in symptoms of depression in the short to medium term, with no reported serious adverse events related to treatment. Acupuncture is cost-effective compared with counselling or usual care alone, although the ranking of counselling and acupuncture depends on the relative costs of delivering these interventions. For patients in whom acupuncture is unavailable or perhaps inappropriate, counselling has an ICER that is less than most cost-effectiveness thresholds.
- Acupuncture, Counselling or Usual Care for Depression (ACUDep): a randomised con...Acupuncture, Counselling or Usual Care for Depression (ACUDep): a randomised controlled trial - Acupuncture for chronic pain and depression in primary care: a programme of research
- major allergen mal d 1 [Malus domestica]major allergen mal d 1 [Malus domestica]gi|4590368|gb|AAD26548.1|AF124825_1Protein
- Executive Summary - Medication-Assisted Treatment for Opioid Addiction in Opioid...Executive Summary - Medication-Assisted Treatment for Opioid Addiction in Opioid Treatment Programs
- The Motor Unit - NeuroscienceThe Motor Unit - Neuroscience
- NeuroscienceNeuroscience
Your browsing activity is empty.
Activity recording is turned off.
See more...
