NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990.

Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition.
Show detailsDefinition
Organic impotence refers to the inability to obtain an erection firm enough for vaginal penetration, or the inability to sustain the erection until completion of intercourse. In contrast to psychogenic impotence, which is impotence caused by anxiety, guilt, depression, or conflict around various sexual issues, organic impotence, the more common of the two categories of erectile dysfunction, is caused by physical problems. Ten to 20% of middle-aged men and a much higher percentage of elderly men are impotent. Aside from its importance as a common and distressing sexual problem, organic impotence may herald important medical problems.
Technique
The first step in the evaluation of erectile dysfunction is to determine whether it is due to organic or psychogenic causes. This usually requires clinical and laboratory data. Specialized tests become important when specific diagnoses are considered.
The history can be useful in distinguishing organic from psychogenic impotence (Table 187.1). The patient with organic impotence describes problems with erection that progress over months to years. At first, the patient will have partial erections or seemingly firm erections that become flaccid during intercourse. With time, total erectile failure ensues. Organic impotence is constant and nonselective, meaning it is not better or worse with any specific partner or any type of stimulation.
Table 187.1
Distinguishing Psychogenic from Organic Impotence by the History.
By contrast, psychogenic impotence typically is abrupt in onset, often in relation to psychological trauma, and may wax and wane. Patients with psychogenic impotence may have total erectile failure with one partner but not another, or be impotent during sexual intercourse but not during self-stimulation. Normally occurring spontaneous erections in the morning suggest psychogenic rather than organic causes for impotence.
For the patient whose history suggests organic impotence, further history, physical and laboratory data will help identify the cause. The classification listed in Table 187.2 is based on the pathophysiologic scheme presented above, and includes mechanical problems that can interfere with erection. Vascular disease is the most common cause of impotence. In advanced cases, Lehriche's syndrome of aortoiliac occlusion will be suggested by bilateral thigh or calf claudication, loss of muscle mass in the buttocks and legs, and impotence. However, the majority of patients with vascular impotence have less severe vascular disease and many will have occlusive disease of the hypogastric-cavernous bed only. Even among patients without claudication, vascular disease is still a likely cause of impotence, especially if risk factors for atherosclerosis are present. Nonatherosclerotic disease is a consideration in the patient with a history of trauma or radiation to the pelvis, both of which cause fibrosis of vessels.
Table 187.2
Causes of Organic Impotence.
While impotence may be the presenting symptom of vascular disease, in neurologic disease impotence generally occurs in the setting of an obvious nervous system disorder, typically in patients known to have spinal cord pathology or neuropathy. Impotent patients should be questioned about decreased genital sensation, which would suggest diabetic, alcoholic, or other forms of neuropathy; weakness, which may accompany multiple sclerosis or spinal cord tumors; and back pain, bowel, and bladder symptoms, which raise concern for cauda equina syndrome. A careful drug history is important in the evaluation of impotence. Drugs that cause impotence (Table 187.3) generally do so by interfering with neurotransmission.
Table 187.3
Classes of Drugs That Can Cause Impotence.
Endocrine problems, though uncommon, should be considered in patients presenting with impotence. As a rule, impotence due to hypogonadism will be partial and accompanied by decreased libido. Hypothalmic–pituitary problems, which include tumors, are the most common endocrine disorders causing impotence, followed by primary gonadal failure from one of many causes. Poorly controlled diabetes with polyuria and polydypsia is an important reversible cause of impotence, as is hyperthyroidism. Certain drugs, alcohol included, can lead to impotence as a result of endocrine disturbances.
Finally, the history may suggest one of several mechanical causes of impotence such as Peyronie's disease and congenital or acquired abnormalities of the penis.
Examination of the vascular system is particularly relevant to the evaluation of the impotent patient. Absence of pulses in the feet and presence of femoral bruits suggest atherosclerosis. However, normal femoral and pedal pulses do not exclude selective obstruction to penile blood flow. Direct palpation of the dorsal artery of the penis may be informative if pulsation is absent. The presence of a pulse, however, does not rule out vascular disease, particularly in a patient who is able to achieve normal erections at rest, but unable to maintain them during thrusting. At the same time that the penile pulses are palpated, the examiner should feel for plaques in the corpora cavernosa which would indicate Peyronie's disease.
Neurologic impotence is suggested by the absence of sensation in the sacral dermatomes when tested by pinprick, or by neurologic abnormalities elsewhere. The bulbocavernosus reflex may be assumed to be present if anal sphincter tone is normal on rectal examination. If there is doubt, the reflex can be tested by pinching the glans penis and assessing sphincter contraction during the rectal examination.
Hypogonadism may be suggested by the patient's general appearance. If testosterone deficiency antedates puberty, as in Klinefelter's syndrome, eunuchoid proportions—defined as an arm span 5 cm or more in excess of height, or a sole-to-pubis length exceeding crown-to-pubis length by more than 2 cm—may be present. In postpubertal males whose testosterone levels are markedly depressed, the secondary sexual characteristics may become atrophic. Testicles less than 4 cm in length or a prostate gland that is smaller than expected may be the only clues on physical examination to a pituitary tumor with secondary hypogonadism.
Basic Science
Erection is a vascular event. The penis becomes rigid when blood flow to the corpora cavernosa increases sixfold and venous outflow is physiologically impeded. Penile perfusion is governed by three organ systems—the neurologic, circulatory, and endocrinologic systems—each necessary for potency. The neurologic system accounts for vasodilation and venoconstriction of the corporal blood vessels so that blood is shunted to the erectile tissues; the circulatory system provides adequate blood flow to the hypogastric-cavernous bed, a distal branch off the internal iliac vessels; and the endocrine system, mediated by testosterone, plays a permissive role through mechanisms that have yet to be elucidated.
The neurologic pathways required for erection originate in the cerebral cortex where visual, auditory, and psychic stimuli are processed, and in the pudenal nerve, an afferent nerve that transmits tactile sensations from the genitals to the sacral segments of the spinal cord and cortex. Efferent signals from the spinal cord pass along the pelvic parasympathetic nerves and dilate the corporal vessels. The specific neurotransmitters have not been fully defined; acetylcholine, and perhaps vasoactive intestinal peptide, appears to be important. There are many causes of neurogenic impotence. Anything that disrupts neural pathways or blocks neurochemical transmission will have an adverse effect on erection. Psychologic factors probably interfere with erection by inhibiting corticosacral efferent pathways.
The circulatory system plays a central role in obtaining and sustaining erections. Augmentation of blood flow to the corporal bodies depends on the intravascular pressure in the penile artery. Vascular lesions—typically atherosclerotic, but occasionally fibrotic—and systemic hypotension will limit flow to the corpora. In certain patients, blood flow at rest may be sufficient to obtain an erection but not sufficient to maintain it during intercourse, when the pelvic musculature places greater demands on a compromised blood supply.
Testosterone is necessary for normal libido and plays a permissive role in potency. Hypogonadism, as seen in primary testicular problems or pituitary–hypothalmic abnormalities, is associated with impotence that improves with androgen replacement.
Clinical Significance
An approach to the diagnosis and management of the impotent patient is presented in Figure 187.1. Apparent and likely causes of impotence should be considered first and, if possible, eliminated before the work-up continues. For instance, observing the patient for a few weeks off offending medication may be all that is necessary to establish the cause of impotence. When no obvious or remediable cause is present, the next step is based on the clinical impression of the likelihood of organic versus psychologic impotence. If the latter is considered more likely, it is perfectly reasonable to refer the patient directly for sexual therapy, with the option of reconsidering the diagnosis if, after appropriate therapy, there is no improvement. While an occasional patient with organic impotence will be misrouted, many more with psychogenic impotence will be spared an unnecessary and costly evaluation for organic causes. When organic impotence is likely, a serum testosterone level is the initial screening test for hypogonadism and should be obtained prior to urologic referral. Patients with low testosterone levels require further endocrine evaluations as depicted in Figure 187.1.
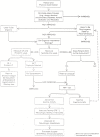
Figure 187.1
Evaluation of erectile dysfunction. (Reproduced with permission: Ende J. Impotence: Organic or Psychogenic? Clin Exper 1984; 1(3):61. Figure by Mr. Albert Miller.)
In the majority of patients the impotence is organic, though not endocrinologic, and there is no easily remedied cause. These patients require physiologic testing and urologic consultation for specific diagnosis. Likely causes of impotence in this group include vascular and neurologic diseases. These patients are candidates for penile prostheses or, in special cases, for revascularization. Patients interested in surgical approaches should be referred for further testing. There is little to be gained by continuing the work-up of patients who prefer not to have an operation.
If surgical intervention is an acceptable option, the work-up then proceeds with a noctural penile tumescense (NPT) test, the single most valuable study to establish the diagnosis of organic impotence. The NPT test exploits the fact that males from birth to old age normally have erections during rapid eye movement (REM) sleep. Psychogenic impotence is associated with normal erections during sleep. In organic impotence there should be no evidence of erection or, if erections are present, they should be limited and poorly sustained.
Penile blood flow is measured using a Doppler probe and a 2.5 cm blood pressure cuff. Systolic pressures in the right and left corpora cavernosa are measured and the penile–brachial index is calculated taking a ratio of penile systolic pressure to brachial systolic pressure. These measures should be repeated before and after 3 minutes of exercising the pelvic and leg muscles. In normal men, the PBI should be 0.9 or greater. Ratios between 0.7 and 0.9 suggest vascular impotence; a ratio below 0.6 is diagnostic. Pelvic arteriography can be done if revascularization is considered.
Measurement of the penile vibration perception threshold provides an inexpensive, reproducible, and painless screening test with acceptable sensitivity for detecting neuropathy. Abnormalities at the level of the sacral cord can be documented by sacral latency testing, while upper motor neuron impotence can be demonstrated with genital-cerebral evoked response testing. These latter procedures are not indicated in unselected patients with impotence.
Treatment of impotence due to hypogonadism is parenteral testosterone replacement. Management of patients in whom impotence is caused by a pituitary tumor is directed at the tumor.
Drug-related impotence is managed by withdrawing the offending agent or, if that is not possible, reducing the dosage. Almost all drugs that cause impotence do so in a dosage-related fashion. A hypertensive patient who is impotent while taking 2 g daily of methyldopa may regain potency on 1 g daily of methyldopa and a second drug.
The prognosis is favorable for alcohol-related impotence. Most patients who stop drinking or reduce their consumption to more moderate levels will see their impotence improve. Exceptions tend to be those who have developed hepatic cirrhosis with gonadal atrophy and feminization.
In diabetics, impotence that develops acutely in the setting of hyperglycemia and poor metabolic control is usually reversible. This is not true of the slowly progressive impotence of long-standing diabetes that is a manifestation of autonomic neuropathy. Intracavernosal self-injection of vasoactive drugs such as papaverine, which relaxes arteriolar smooth muscle is a promising new approach to treatment that is particularly suited for diabetic patients whose erectile dysfunction is on a neuropathic basis. It also has been used with success in spinal cord patients.
The penile prosthesis is suitable treatment for most patients with vascular impotence. While there is currently considerable interest in revascularization techniques, insertion of a semirigid rod, such as the Jones prosthesis, remains the most commonly performed procedure.
References
- Carter JN, Tyson JE, Tolis G. et al. Prolactin-secreting tumors and hypogonadism in 22 men. N Engl J Med. 1978;299:847–52. [PubMed: 211411]
- Goldstein I. Vasculogenic impotence: Its diagnosis and treatment. In: deVere White R, ed., Problems in urology: Sexual dysfunction. Philadelphia: Lippincott, 1987;1:547–63.
- Kolodny RC, Masters WH, Johnson VE. Textbook of sexual medicine. Boston: Little, Brown, 1979.
- Krane RJ, Siroky MB, Goldstein I, eds. Male sexual dysfunction. Boston: Little, Brown, 1983.
- Montague DK, James RE, DeWolf VG. et al. Diagnostic evaluation, classification, and treatment of men with sexual dysfunction. Urology. 1979;14:545–48. [PubMed: 574673]
- Schiavi RC. Male erectile disorders. Annu Rev Med. 1981;32:509–20. [PubMed: 7013686]
- Shabsigh R, Fishman IJ, Scott FB. Evaluation of erectile impotence. Urology. 1988;32:83–90. [PubMed: 3041668]
- Slag MF, Morley JE, Elson MK. et al. Impotence in medical clinic outpatients. JAMA. 1983;249:1736–40. [PubMed: 6827762]
- Spark RF. Neuroendocrinology and impotence. Ann Intern Med. 1983;98:103–5. [PubMed: 6336640]
- PubMedLinks to PubMed
- Psychogenic versus primary organic impotence.[Int J Impot Res. 1994]Psychogenic versus primary organic impotence.Lee WH, Kim YC, Choi HK. Int J Impot Res. 1994 Jun; 6(2):93-7.
- Gonadal dysfunction in diabetic men with organic impotence.[J Clin Endocrinol Metab. 1987]Gonadal dysfunction in diabetic men with organic impotence.Murray FT, Wyss HU, Thomas RG, Spevack M, Glaros AG. J Clin Endocrinol Metab. 1987 Jul; 65(1):127-35.
- Use of the Florida Sexual History Questionnaire to differentiate primary organic from primary psychogenic impotence.[J Androl. 1993]Use of the Florida Sexual History Questionnaire to differentiate primary organic from primary psychogenic impotence.Geisser ME, Murray FT, Cohen MS, Shea PJ, Addeo RR. J Androl. 1993 Jul-Aug; 14(4):298-303.
- Review Arteriogenic erectile impotence.[Dan Med Bull. 1986]Review Arteriogenic erectile impotence.Metz P. Dan Med Bull. 1986 Jun; 33(3):134-50.
- Review [Male impotence in old age].[Minerva Med. 1994]Review [Male impotence in old age].Pentimone F, Del Corso L. Minerva Med. 1994 May; 85(5):261-4.
- Organic Impotence - Clinical MethodsOrganic Impotence - Clinical Methods
- STK_RS05340 [Sulfurisphaera tokodaii str. 7]STK_RS05340 [Sulfurisphaera tokodaii str. 7]Gene ID:1458936Gene
- SNORD113-1 small nucleolar RNA, C/D box 113-1 [Homo sapiens]SNORD113-1 small nucleolar RNA, C/D box 113-1 [Homo sapiens]Gene ID:767561Gene
- INS-IGF2 INS-IGF2 readthrough [Homo sapiens]INS-IGF2 INS-IGF2 readthrough [Homo sapiens]Gene ID:723961Gene
- HSP90AB4P heat shock protein 90 alpha family class B member 4, pseudogene [Homo ...HSP90AB4P heat shock protein 90 alpha family class B member 4, pseudogene [Homo sapiens]Gene ID:664618Gene
Your browsing activity is empty.
Activity recording is turned off.
See more...