NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990.

Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition.
Show detailsDefinition
Blood pressure is the pressure, measured in millimeters of mercury, within the major arterial system of the body. It is conventionally separated into systolic and diastolic determinations. Systolic pressure is the maximum blood pressure during contraction of the ventricles; diastolic pressure is the minimum pressure recorded just prior to the next contraction.
The blood pressure is usually written as the systolic pressure over the diastolic pressure (e.g., 120/80 mm Hg). The minimum acceptable blood pressure is determined by adequate perfusion of the vital organs without symptoms of hypotension. This is usually more than 90 mm Hg systolic and 60 mm Hg diastolic, although there can be great variation between patients. The report of the Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure (1984) gives a recommended scheme for categorizing arterial pressure in individuals age 18 years or over. This scheme is summarized in Table 16.1.
Table 16.1
Interpretation of Blood Pressure Measurements in Individuals 18 Years of Age and Older a.
Technique
The most accurate measurement of arterial blood pressure is obtained by direct methods that involve sophisticated and expensive equipment as well as cannulation of an artery. Although these methods are necessary in some settings, sphygmomanometric measurements are much easier and safer, and are accurate enough for most clinical situations.
The standard blood pressure cuff must be of the proper size to minimize errors in blood pressure determinations. The width of the bladder ideally should be 40% of the circumference of the limb tested. Most standard cuffs have a bladder length that is twice its width. This ensures that the length is the recommended 80% of the limb circumference. Cuffs that are too small give results erroneously high; cuffs that are too large give results erroneously low.
The patient should be comfortably seated and the deflated cuff applied with the bladder centered over the brachial artery. It should be high enough on the arm to allow the stethoscope to be placed in the antecubital fossa without touching the cuff. Pressure is then rapidly increased to at least 30 mm Hg higher than that which eliminates a palpable radial pulse.
With the stethoscope in place over the brachial artery in the antecubital fossa, the cuff is slowly deflated at a rate of 2 mm Hg per second. As the pressure declines, the Korotkoff sounds are noted. These sounds (Table 16.2) are low pitched and are sometimes more easily auscultated with the bell of the stethoscope. Palpating the loss of the radial pulse is essential because some patients, particularly those with hypertension, may have an auscultatory gap. This is a complete loss of Korotkoff sounds at pressures higher than the true diastolic. Careful auscultation in these patients will reveal return of sounds, allowing accurate pressure determinations (Figure 16.1).
Table 16.2
Sequence of Korotkoff Sounds Obtained during Sphygmomanometry.
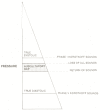
Figure 16.1
Temporary loss of all Korotkoff sounds is called an auscultatory gap.
Systolic blood pressure is best estimated using phase I Korotkoff sounds (i.e., the first sounds auscultated). Phase V Korotkoff sounds (i.e., loss of all sounds) estimates diastolic pressures. Usually phase IV and phase V sounds occur very near each other. If, however, they are widely separated, the blood pressure may be written to signify both (e.g., 128/80/30). Under these circumstances, phase IV sounds more accurately predict diastolic pressures.
Considerable controversy exists concerning prediction of the diastolic blood pressure using Korotkoff sounds. Kirkendall et al. (1981) addresses these controversies and recommends phase V sounds in adults and phase IV in children.
Systolic pressure normally varies with respirations. During inspiration, the negative intrathoracic pressure causes pooling of blood in expanding pulmonary vessels and a delay of flow to the left ventricle. Thus, systolic pressure falls as cardiac output falls momentarily.
The following procedure checks for a paradoxical pulse. During normal respirations, the pressure is noted at which Korotkoff sounds are first heard. Commonly, these first sounds are audible only during expiration. Cuff pressure is slowly lowered until Korotkoff sounds are heard continually. If the difference between these two pressures exceeds 10 mm Hg, a pulsus paradoxus exists. A paradoxical pulse occurs most commonly with clinical situations involving large negative intrathoracic pressures like heavy breathing, asthma, or emphysema. Pulsus paradoxus also occurs in pericardial tamponade, but the mechanisms are more complex and not as well understood.
The blood pressure is usually taken with the patient seated. Additional information may be gained by checking the patient in the lying and standing positions. A supine blood pressure should be compared to that obtained after the patient has been standing for a sufficient time to allow the pulse to stabilize. Normally, systolic blood pressure should not drop more than 10 mm Hg, and diastolic pressure should remain unchanged or rise slightly. Significant orthostatic changes in blood pressure may indicate dehydration or an adverse drug reaction. When correlated with an inadequate rise in pulse, it may indicate autonomic nervous system dysfunction.
All patients should have the blood pressure checked in the left and right arm at least once to detect anatomical abnormalities. Pressure differences greater than 15 mm Hg may indicate obstruction of flow to one of the brachial arteries, such as occurs in coarctation of the aorta.
Basic Science
The overall blood pressure as measured in the brachial artery is maintained by the cardiac output and the total peripheral resistance (TPR) to flow. The mean arterial pressure (MAP) is calculated by the formula:
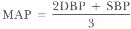
where DBP and SBP are diastolic and systolic blood pressure, respectively. Mean arterial pressure is a useful concept because it can be used to calculate overall blood flow, and thus delivery of nutrients to the various organs. It is a good indicator of perfusion pressure (ΔP).
Blood flow is defined by Poiseuille's law:

where Q is the blood flow, ΔP is the pressure gradient, r is the radius of the vessel, N is the blood viscosity, and L is the length of the vessel. This formula is commonly restated in a more clinically useful expression:

Here CO is the cardiac output in liters/minute and is the clinical equivalent of blood flow (Q). MAP (in mm Hg) is used to approximate the pressure gradient (ΔP). TPR is the resistance to flow in dynes · sec · cm−5 and clinically represents 8 NL/πr4 The conversion factor 80 appears in the formula simply to allow use of more conventional units.
Example 1: BP of 120/80 and normal cardiac output of 5 L/min:
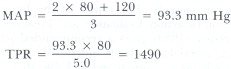
In this example the TPR demonstrated can be used as a standard in evaluating pathologic conditions.
Example 2: Normal cardiac output of 5.0 L/min and BP of 170/110:

In this example of a typical hypertensive, the cardiac output is normal and the elevated blood pressure is thought to occur as a direct result of increased TPR. The TPR is maintained by resistance vessels, small precapillary muscular arterioles that regulate the rate of diastolic runoff in the arterial tree. These resistance vessels regulate blood flow by changes in vascular tone that adjust the radius (r) of the vessel. Since radius appears in the formula to the fourth power (i.e., TPR = 8NL/πr4), small adjustments cause significant changes in TPR.
Example 3: BP of 80/60, TPR of 600:

This example is representative of septic shock. Lax vasomotor tone causes a low TPR, and blood pressure can be maintained only by a substantial rise in cardiac output.
Cardiac output is calculated by multiplying heart rate by stroke volume. In intrinsic cardiac disease the stroke volume may be decreased, but cardiac output can be maintained by a compensatory rise in heart rate. For a given TPR, the blood pressure is maintained unless there is a relative bradycardia or a further fall in stroke volume.
During systole, the volume of blood ejected from the left ventricle must enter the aorta and major arterial branches. The distensibility of the arteries compensates this volume and stores energy in order to perfuse the capillary beds during diastole. If, for example, the aorta is stiff from atherosclerotic disease, the left ventricle generates a higher pressure to eject a given quantity of blood, and so the systolic pressure is higher.
With each heartbeat there are minor adjustments in these factors that are all intricately controlled to provide perfusion of the organs. Baroreceptors in the aorta and carotid body are stretched by the blood pressure and send feedback information to autonomic nervous system centers in the brainstem. Autonomic outflow then controls heart rate, vascular tone, and contractile state of the myocardium to adjust blood pressure accordingly.
Clinical Significance
The ideal blood pressure adequately perfuses all of the various organ systems without causing damage. Any organ not adequately perfused will suffer ischemic damage and/or be unable to perform adequately. Poor brain blood flow can cause a declining mental status, lethargy, somnolence, and even coma. Poor renal perfusion may cause renal failure with wide-ranging metabolic consequences. In contrast, blood pressures that are too high may cause end organ damage with equally disastrous consequences. Heart attack, stroke, hypertensive renal failure, and retinopathy are all too familiar in the hypertensive population.
The earliest clinical manifestation of low blood pressure may be fatigue or shortness of breath on exertion. The increased oxygen and nutrient demand by exercising muscles cannot be met if the perfusion pressure is inadequate. Further declines in blood pressure may lead to lightheadedness, particularly on assuming an upright posture. Urine output is a very helpful indicator of vital organ perfusion and with normal kidneys should not drop below 20 to 30 ml/hr if the intrarenal blood pressure is satisfactory. The most common causes of low blood pressure are dehydration or decreased cardiac output. Dehydration, manifested by postural blood pressure drops and reflex tachycardia, is treated with appropriate volume expansion. This may be blood products in the case of trauma with significant bleeding or salt and water in the case of prolonged exposure to a hot environment. Poor cardiac output may result in hypotension; a thorough examination of cardiac contractility and heart rate will dictate appropriate therapy. Inadequate contractility may be improved with positive inotropic agents such as digoxin. Abnormal heart rates may require antiarrhythmic agents if too rapid, or vagolytic agents such as atropine if too slow. Occasionally, a pacemaker is required to maintain a satisfactory heart rate and blood pressure.
The clinical significance of hypertension has been shown in numerous studies. Prolonged exposure to elevated pressure is associated with an increased incidence of cardiovascular disease (e.g., stroke, dissecting aneurysm, and heart attack), renal failure, and retinopathy. Moreover, there is evidence that morbidity and mortality can be reduced with proper treatment of hypertension. There are perhaps 60 million people in the United States with hypertension, and a proper understanding of this disorder is essential.
Once a diagnosis of hypertension is made, most patients will require lifelong therapy. Spontaneous variations in blood pressure caused by emotional, dietary, or exertional factors make the problem more difficult. If the diagnosis is based on an inaccurate blood pressure determination or a single reading, a lifetime of drug expense and exposure to potential side effects may be endured needlessly. Therefore, except in severe hypertension, at least three readings should be assessed according to Table 16.1 before therapy is initiated.
Most of the therapeutic intervention trials used a sitting pressure and phase 5 diastolic recordings. Our clinical judgments are based on these studies, and so our criteria for determining blood pressure should be the same.
Although more is known about diastolic hypertension with regard to morbidity, mortality, and effects of treatment, isolated systolic hypertension is equally important and has more recently been recognized as a significant clinical problem. Isolated systolic hypertension, as defined in Table 16.1, is not uncommon in the elderly. This same population, however, frequently has significant postural differences in systolic and diastolic pressures both with and without treatment. Meticulous attention to these details is required.
Since Dr. Janeway's review (1915) of the study of blood pressure, a remarkable body of data and therapeutic tools have become available to the modern physician. It behooves us to study these developments and apply them wisely.
References
- Fowler NO. Physiology of cardiac tamponade and pulsus paradoxus. I. Mechanisms of pulsus paradoxus in cardiac tamponade. Mod Concepts Cardiovasc Dis. 1978;47:109–13. [PubMed: 723849]
- Janeway TC. Important contributions to clinical medicine during the past 30 years from the study of human blood pressure. Bull Johns Hopkins Hosp. 1915;26:341–50.
- Kannel WB, Sorlie P. Hypertension in Framingham. In: Paul O, ed. Epidemiology and control of hypertension. New York: Stratton Intercontinental, 1975;553–92.
- *Kirkendall WM, Feinleib M, Freis ED. et al. Recommendations for human blood pressure determination by sphygmomanometers. Hypertension. 1981;3:509A–19A. [PubMed: 7309211]
- The 1984 report of the Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure. Arch Intern Med 1984; 144:1045–57. [PubMed: 6143542]
- Report of the Task Force on Blood Pressure Control in Children. Pediatrics 1977;59(suppl):797–820. [PubMed: 859728]
- Veterans Administration Cooperative Study Group on Anthihypertensive Agents. I. JAMA 1967;202:1028–34. II. JAMA 1970;213:1143–52.
- PubMedLinks to PubMed
- [Arterial hypertension difficult to control in the elderly patient. The significance of the "white coat effect"].[Rev Port Cardiol. 1999][Arterial hypertension difficult to control in the elderly patient. The significance of the "white coat effect"].Amado P, Vasconcelos N, Santos I, Almeida L, Nazaré J, Carmona J. Rev Port Cardiol. 1999 Oct; 18(10):897-906.
- [Comparison of invasive blood pressure measurement in the aorta with indirect oscillometric blood pressure measurement at the wrist and forearm].[Z Kardiol. 1995][Comparison of invasive blood pressure measurement in the aorta with indirect oscillometric blood pressure measurement at the wrist and forearm].Saul F, Aristidou Y, Klaus D, Wiemeyer A, Lösse B. Z Kardiol. 1995 Sep; 84(9):675-85.
- Protamine-induced hypotension in heart operations: application of the concept of ventricular-arterial coupling.[J Thorac Cardiovasc Surg. 1996]Protamine-induced hypotension in heart operations: application of the concept of ventricular-arterial coupling.Oe M, Asou T, Morita S, Yasui H, Tokunaga K. J Thorac Cardiovasc Surg. 1996 Aug; 112(2):462-71.
- Review [Hypertension in pregnancy].[Vnitr Lek. 2006]Review [Hypertension in pregnancy].Cífková R. Vnitr Lek. 2006 Mar; 52(3):263-70.
- Review Bedside Evaluation of the Autonomic System.[Clinical Methods: The History,...]Review Bedside Evaluation of the Autonomic System.Barbato AL. Clinical Methods: The History, Physical, and Laboratory Examinations. 1990
- Blood Pressure - Clinical MethodsBlood Pressure - Clinical Methods
Your browsing activity is empty.
Activity recording is turned off.
See more...