NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Ashley EA, Niebauer J. Cardiology Explained. London: Remedica; 2004.
Although few generalists actually perform echocardiograms, most order or have to interpret them at some stage. Our aim then is not to explain how to carry out echocardiography, but how to realize its potential and limitations.
Background
"Ultra" sound has a frequency above the range audible by humans (ie, >20,000 Hz). For adult cardiac imaging, ultrasound waves in the range of 4–7 MHz are used (intravascular ultrasound uses frequencies as high as 30 MHz). These are created within the ultrasound probe by striking piezo-electric crystals with an electric pulse, which stimulates the crystals to release sound waves. The central principle of ultrasound imaging is that, while most waves are absorbed by the body, those at interfaces between different tissue densities are reflected. In addition to emitting the ultrasound waves, the transducer detects the returning waves, processes the information, and displays it as characteristic images. Higher frequency ultrasound waves increase resolution, but decrease tissue penetration.
Imaging modes
There are three basic "modes" used to image the heart:
- two-dimensional (2D) imaging
- M-mode imaging
- Doppler imaging
Two-dimensional imaging
2D imaging is the mainstay of echo imaging and allows structures to be viewed moving in real time in a cross-section of the heart (two dimensions). It is used for detecting abnormal anatomy or abnormal movement of structures. The most common cross-sectional views are the parasternal long axis, the parasternal short axis, and the apical view (see Figure 1). The gastric or subcostal and suprasternal views are also commonly used.
M-mode imaging
The M-mode echo, which provides a 1D view, is used for fine measurements. Temporal and spatial resolutions are higher because the focus is on only one of the lines from the 2D trace (see Figure 2).

Figure 2
M-mode image of (a) the aorta/left atrium and (b) the mitral valve, both in a healthy heart.
Doppler imaging
The concept of Doppler imaging is familiar to all those who have heard the note of a police siren change as it moves past them – as the police siren travels towards you, the frequency of the wave (pitch) appears to be higher than if it was stationary; as the siren travels away, the pitch appears to be lower.
Estimates of blood-flow velocity can be made by comparing the frequency change between the transmitted and reflected sound waves. In cardiac ultrasound, Doppler is used in three ways:
- continuous-wave (CW) Doppler
- pulsed-wave (PW) Doppler
- color-flow mapping (CFM)
Continuous-wave Doppler
CW Doppler is sensitive, but, because it measures velocity along the entire length of the ultrasound beam and not at a specific depth, it does not localize velocity measurements of blood flow. It is used to estimate the severity of valve stenosis or regurgitation by assessing the shape or density of the output (see Figure 3).

Figure 3
Continuous-wave Doppler signal.
Pulsed-wave Doppler
PW Doppler was developed because of the need to make localized velocity measurements of turbulent flow (it measures the blood-flow velocity within a small area at a specified tissue depth). It is used to assess ventricular in-flow patterns, intracardiac shunts, and to make precise measurements of blood flow at valve orifices.
Color-flow mapping
CFM uses measurements of the velocity and direction of blood flow to superimpose a color pattern onto a section of a 2D image (see Figure 4). Traditionally, flow towards the transducer is red, flow away from the transducer is blue, and higher velocities are shown in lighter shades. To aid observation of turbulent flow there is a threshold velocity, above which the color changes (in some systems to green). This leads to a "mosaic" pattern at the site of turbulent flow and enables sensitive screening for regurgitant flow.
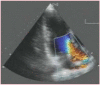
Figure 4
Color-flow mapping.
Transesophageal echocardiography
Transesophageal echocardiography (TEE) is usually carried out under mild sedation with midazolam. A thin probe is passed down the esophagus until it is level with the heart. This position provides especially clear views. It is particularly useful for imaging posterior cardiac structures. The key indications for TEE are:
- infective endocarditis – if vegetations are not seen on transthoracic echo, but suspicion is high, or with prosthetic valves
- to rule out an embolic source (especially in atrial fibrillation)
- acute dissection
- mitral valve (MV) disease preoperatively
Contrast echocardiography
Contrast echo can be useful for confirming a diagnosis of atrial septal defect (ASD). Agitating saline or synthetic contrast create microbubbles. These are very reflective, and when injected intravenously can be seen as opacification in the echo window. They are normally seen on the right side of the heart before being trapped and absorbed by the pulmonary capillaries, so have no route to the left side of the heart. The contrast created by the bubbles allows a left-to-right shunt to be seen as a jet "interrupting" the opacification of the right atrium. However, there is a theoretical risk of systemic air embolism with a right-to-left shunt.
Applications
Echo is the cheapest and least invasive method available for screening cardiac anatomy. Generalists most commonly request an echo to assess left ventricular (LV) dysfunction, to rule out the heart as a thromboembolic source, and to characterize murmurs. The approximate normal values for various cardiac structures are described in Table 1.
Table 1
The approximate normal values for various cardiac structures. IV: interventricular; LV: left ventricular.
Systolic dysfunction
LV systolic dysfunction is assessed using the ejection fraction (the percentage of the end diastolic volume ejected during systole). In most cases, this is estimated by eye from all the available echo views. A normal ejection fraction is 50%–80%, but values as low as 5% are compatible with life (end-stage heart failure).
The E/A ratio
When flow across the MV is assessed with PW Doppler, two waves are characteristically seen. These represent passive filling of the ventricle (early [E] wave) and active filling with atrial systole (atrial [A] wave). Classically, the E-wave velocity is slightly greater than that of the A wave (see Figure 5). However, in conditions that limit the compliance of the LV, two abnormalities are possible:
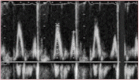
Figure 5
E and A waves representing mitral flow in a healthy heart (E>A).
- reversal – in which the A wave is greater than the E wave. This indicates slow filling caused by older age, hypertension, left ventricular hypertrophy (LVH), or diastolic dysfunction
- exaggeration of normal – a tall, thin E wave with a small or absent A wave. This indicates restrictive cardiomyopathy, constrictive pericarditis, or infiltrative cardiac disease (eg, amyloidosis)
Diastolic dysfunction
A normal LV ejection fraction in the presence of the heart failure syndrome leads to a search for diastolic dysfunction. Typical echo findings in diastolic dysfunction are normal LV cavity size, thickened ventricle, and reversed E/A ratio.
Wall-motion abnormality
When ischemia occurs, contractile abnormalities of segments of the myocardium can be detected by echo prior to the appearance of electrocardiogram (ECG) changes or symptoms. Therefore, echo can be a valuable tool in the diagnosis of both stable coronary artery disease (via stress echo) and acute myocardial infarction. In the former situation, it offers localization of the ischemic region where the ECG cannot; in the latter, it offers some measure of the extent of the infarct and a screen for complications, such as ventricular septal defect (VSD).
Valve assessment
Echo is the tool of choice for the assessment of valvular abnormalities.
Aortic stenosis
The etiology of aortic stenosis (AS) can be confirmed by the visualization of either a bicuspid valve or calcification. The severity of the stenosis can be estimated by measuring high-velocity flow across the valve by Doppler. This can be converted to an estimation of the pressure drop. In addition, the effective orifice area can be measured (see Table 2).
Table 2
Echo characteristics of aortic stenosis.
Aortic regurgitation
CFM is the most useful technique for detecting and quantifying the degree of regurgitation. The width of the regurgitant jet and of the slope of the decline in pressure gradient between the left ventricle and the aorta (which is reduced already compared with normal) are measured.
Mitral stenosis
With mitral stenosis (MS), as with AS, calcified, immobile MV leaflets can be demonstrated with 2D and M-mode echo. Anterior motion of the posterior MV leaflet in diastole (caused by commissural fusion) is characteristic in MS. Doppler demonstrates increased flow velocity and can be used to estimate the effective orifice area (see Table 3).
Table 3
Echo characteristics of mitral stenosis.
Mitral regurgitation
As with aortic regurgitation, mitral regurgitation is assessed using CFM. The severity of mitral regurgitation is commonly reported as the area of the regurgitant jet expressed as a percentage of the area of the left atrium.
Mitral valve prolapse
The criteria for the diagnosis of MV prolapse (MVP) from an echo have changed over the years. Initial reports using the 4-chamber view suggested a population prevalence of almost 20%. However, a more accurate figure of approximately 5% results from stricter criteria. Most diagnose only on the basis of the parasternal long axis view. Some go so far as to suggest it is invalid to diagnose MVP on the 4-chamber view at all.
Paraprosthetic regurgitation
Although metal valves stop ultrasound completely, echo is a useful tool for studying prosthetic valve function. The TEE approach is often used.
Infective endocarditis
Echo is the key investigation in infective endocarditis and, although a low threshold for TEE is warranted by its higher detection rate, transthoracic echo can demonstrate vegetations in approximately 70% of cases (see Chapter 10, Infective endocarditis).
Embolic sources
The primary cardiac sources for embolism are:
- an akinetic ventricular segment
- an LV aneurysm
- the atrial appendage
These are best visualized with TEE.
Hypertrophic cardiomyopathy
Although hypertrophy is variable, echo remains the screening tool of choice in suspected cases. The classic features are asymmetrical hypertrophy of the interventricular septum and anterior movement of the MV in systole. LV function is normal, and there may be dynamic LV outflow tract obstruction.
Further reading
- Chambers JB. Clinical Echocardiography. London: BMJ Books, 1995.
- Feigenbaum HMD. Echocardiography, 5th edn. Philadelphia: Lea & Febiger, 1994.
- Understanding the echocardiogram - Cardiology ExplainedUnderstanding the echocardiogram - Cardiology Explained
- STK_RS09895 [Sulfurisphaera tokodaii str. 7]STK_RS09895 [Sulfurisphaera tokodaii str. 7]Gene ID:1459821Gene
- Ccdc141 coiled-coil domain containing 141 [Mus musculus]Ccdc141 coiled-coil domain containing 141 [Mus musculus]Gene ID:545428Gene
- AXDND1 axonemal dynein light chain domain containing 1 [Homo sapiens]AXDND1 axonemal dynein light chain domain containing 1 [Homo sapiens]Gene ID:126859Gene
- Mbd6 methyl-CpG binding domain protein 6 [Mus musculus]Mbd6 methyl-CpG binding domain protein 6 [Mus musculus]Gene ID:110962Gene
Your browsing activity is empty.
Activity recording is turned off.
See more...

