All rights reserved. Publications of the World Health Organization can be obtained from WHO Press, World Health Organization, 20 Avenue Appia, 1211 Geneva 27, Switzerland (tel.: +41 22 791 3264; fax: +41 22 791 4857; e-mail: tni.ohw@sredrokoob). Requests for permission to reproduce or translate WHO publications – whether for sale or for noncommercial distribution – should be addressed to WHO Press, at the above address (fax: +41 22 791 4806; e-mail: tni.ohw@snoissimrep).
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Infant and Young Child Feeding: Model Chapter for Textbooks for Medical Students and Allied Health Professionals. Geneva: World Health Organization; 2009.

Infant and Young Child Feeding: Model Chapter for Textbooks for Medical Students and Allied Health Professionals.
Show details2.1. Breast-milk composition
Breast milk contains all the nutrients that an infant needs in the first 6 months of life, including fat, carbohydrates, proteins, vitamins, minerals and water (1,2,3,4). It is easily digested and efficiently used. Breast milk also contains bioactive factors that augment the infant's immature immune system, providing protection against infection, and other factors that help digestion and absorption of nutrients.
Fats
Breast milk contains about 3.5 g of fat per 100 ml of milk, which provides about one half of the energy content of the milk. The fat is secreted in small droplets, and the amount increases as the feed progresses. As a result, the hindmilk secreted towards the end of a feed is rich in fat and looks creamy white, while the foremilk at the beginning of a feed contains less fat and looks somewhat bluish-grey in colour. Breast-milk fat contains long chain polyunsaturated fatty acids (docosahexaenoic acid or DHA, and arachidonic acid or ARA) that are not available in other milks. These fatty acids are important for the neurological development of a child. DHA and ARA are added to some varieties of infant formula, but this does not confer any advantage over breast milk, and may not be as effective as those in breast milk.
Carbohydrates
The main carbohydrate is the special milk sugar lactose, a disaccharide. Breast milk contains about 7 g lactose per 100 ml, which is more than in most other milks, and is another important source of energy. Another kind of carbohydrate present in breast milk is oligosaccharides, or sugar chains, which provide important protection against infection (4).
Protein
Breast milk protein differs in both quantity and quality from animal milks, and it contains a balance of amino acids which makes it much more suitable for a baby. The concentration of protein in breast milk (0.9 g per 100 ml) is lower than in animal milks. The much higher protein in animal milks can overload the infant's immature kidneys with waste nitrogen products. Breast milk contains less of the protein casein, and this casein in breast milk has a different molecular structure. It forms much softer, more easily-digested curds than that in other milks. Among the whey, or soluble proteins, human milk contains more alpha-lactalbumin; cow milk contains beta-lactoglobulin, which is absent from human milk and to which infants can become intolerant (4).
Vitamins and minerals
Breast milk normally contains sufficient vitamins for an infant, unless the mother herself is deficient (5). The exception is vitamin D. The infant needs exposure to sunlight to generate endogenous vitamin D – or, if this is not possible, a supplement. The minerals iron and zinc are present in relatively low concentration, but their bioavailability and absorption is high. Provided that maternal iron status is adequate, term infants are born with a store of iron to supply their needs; only infants born with low birth weight may need supplements before 6 months. Delaying clamping of the cord until pulsations have stopped (approximately 3 minutes) has been shown to improve infants' iron status during the first 6 months of life (6,7).
Anti-infective factors
Breast milk contains many factors that help to protect an infant against infection (8) including:
- immunoglobulin, principally secretory immunoglobulin A (sIgA), which coats the intestinal mucosa and prevents bacteria from entering the cells;
- white blood cells which can kill micro-organisms;
- whey proteins (lysozyme and lactoferrin) which can kill bacteria, viruses and fungi;
- oligosacccharides which prevent bacteria from attaching to mucosal surfaces.
The protection provided by these factors is uniquely valuable for an infant. First, they protect without causing the effects of inflammation, such as fever, which can be dangerous for a young infant. Second, sIgA contains antibodies formed in the mother's body against the bacteria in her gut, and against infections that she has encountered, so they protect against bacteria that are particularly likely to be in the baby's environment.
Other bioactive factors
Bile-salt stimulated lipase facilitates the complete digestion of fat once the milk has reached the small intestine (9). Fat in artificial milks is less completely digested (4).
Epidermal growth factor (10) stimulates maturation of the lining of the infant's intestine, so that it is better able to digest and absorb nutrients, and is less easily infected or sensitised to foreign proteins. It has been suggested that other growth factors present in human milk target the development and maturation of nerves and retina (11).
2.2. Colostrum and mature milk
Colostrum is the special milk that is secreted in the first 2–3 days after delivery. It is produced in small amounts, about 40–50 ml on the first day (12), but is all that an infant normally needs at this time. Colostrum is rich in white cells and antibodies, especially sIgA, and it contains a larger percentage of protein, minerals and fat-soluble vitamins (A, E and K) than later milk (2). Vitamin A is important for protection of the eye and for the integrity of epithelial surfaces, and often makes the colostrum yellowish in colour. Colostrum provides important immune protection to an infant when he or she is first exposed to the micro-organisms in the environment, and epidermal growth factor helps to prepare the lining of the gut to receive the nutrients in milk. It is important that infants receive colostrum, and not other feeds, at this time. Other feeds given before breastfeeding is established are called prelacteal feeds.
Milk starts to be produced in larger amounts between 2 and 4 days after delivery, making the breasts feel full; the milk is then said to have “come in”. On the third day, an infant is normally taking about 300–400 ml per 24 hours, and on the fifth day 500–800 ml (12). From day 7 to 14, the milk is called transitional, and after 2 weeks it is called mature milk.
2.3. Animal milks and infant formula
Animal milks are very different from breast milk in both the quantities of the various nutrients, and in their quality. For infants under 6 months of age, animal milks can be home-modified by the addition of water, sugar and micronutrients to make them usable as short-term replacements for breast milk in exceptionally difficult situations, but they can never be equivalent or have the same anti-infective properties as breast milk (13). After 6 months, infants can receive boiled full cream milk (14).
Infant formula is usually made from industrially-modified cow milk or soy products. During the manufacturing process the quantities of nutrients are adjusted to make them more comparable to breast milk. However, the qualitative differences in the fat and protein cannot be altered, and the absence of anti-infective and bio-active factors remain. Powdered infant formula is not a sterile product, and may be unsafe in other ways. Life threatening infections in newborns have been traced to contamination with pathogenic bacteria, such as Enterobacter sakazakii, found in powdered formula (15). Soy formula contains phyto-oestrogens, with activity similar to the human hormone oestrogen, which could potentially reduce fertility in boys and bring early puberty in girls (16).
2.4. Anatomy of the breast
The breast structure (Figure 3) includes the nipple and areola, mammary tissue, supporting connective tissue and fat, blood and lymphatic vessels, and nerves (17,18).
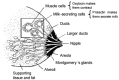
FIGURE 3
Anatomy of the breast.
The mammary tissue – This tissue includes the alveoli, which are small sacs made of milk-secreting cells, and the ducts that carry the milk to the outside. Between feeds, milk collects in the lumen of the alveoli and ducts. The alveoli are surrounded by a basket of myoepithelial, or muscle cells, which contract and make the milk flow along the ducts.
Nipple and areola – The nipple has an average of nine milk ducts passing to the outside, and also muscle fibres and nerves. The nipple is surrounded by the circular pigmented areola, in which are located Montgomery's glands. These glands secrete an oily fluid that protects the skin of the nipple and areola during lactation, and produce the mother's individual scent that attracts her baby to the breast. The ducts beneath the areola fill with milk and become wider during a feed, when the oxytocin reflex is active.
2.5. Hormonal control of milk production
There are two hormones that directly affect breastfeeding: prolactin and oxytocin. A number of other hormones, such as oestrogen, are involved indirectly in lactation (2). When a baby suckles at the breast, sensory impulses pass from the nipple to the brain. In response, the anterior lobe of the pituitary gland secretes prolactin and the posterior lobe secretes oxytocin.
Prolactin
Prolactin is necessary for the secretion of milk by the cells of the alveoli. The level of prolactin in the blood increases markedly during pregnancy, and stimulates the growth and development of the mammary tissue, in preparation for the production of milk (19). However, milk is not secreted then, because progesterone and oestrogen, the hormones of pregnancy, block this action of prolactin. After delivery, levels of progesterone and oestrogen fall rapidly, prolactin is no longer blocked, and milk secretion begins.
When a baby suckles, the level of prolactin in the blood increases, and stimulates production of milk by the alveoli (Figure 4). The prolactin level is highest about 30 minutes after the beginning of the feed, so its most important effect is to make milk for the next feed (20). During the first few weeks, the more a baby suckles and stimulates the nipple, the more prolactin is produced, and the more milk is produced. This effect is particularly important at the time when lactation is becoming established. Although prolactin is still necessary for milk production, after a few weeks there is not a close relationship between the amount of prolactin and the amount of milk produced. However, if the mother stops breastfeeding, milk secretion may stop too – then the milk will dry up.
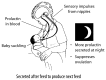
FIGURE 4
Prolactin.
More prolactin is produced at night, so breastfeeding at night is especially helpful for keeping up the milk supply. Prolactin seems to make a mother feel relaxed and sleepy, so she usually rests well even if she breastfeeds at night.
Suckling affects the release of other pituitary hormones, including gonadotrophin releasing hormone (GnRH), follicle stimulating hormone, and luteinising hormone, which results in suppression of ovulation and menstruation. Therefore, frequent breastfeeding can help to delay a new pregnancy (see Session 8 on Mother's Health). Breastfeeding at night is important to ensure this effect.
Oxytocin
Oxytocin makes the myoepithelial cells around the alveoli contract. This makes the milk, which has collected in the alveoli, flow along and fill the ducts (21) (see Figure 5). Sometimes the milk is ejected in fine streams.

FIGURE 5
Oxytocin.
The oxytocin reflex is also sometimes called the “letdown reflex” or the “milk ejection reflex”. Oxytocin is produced more quickly than prolactin. It makes the milk that is already in the breast flow for the current feed, and helps the baby to get the milk easily.
Oxytocin starts working when a mother expects a feed as well as when the baby is suckling. The reflex becomes conditioned to the mother's sensations and feelings, such as touching, smelling or seeing her baby, or hearing her baby cry, or thinking lovingly about him or her. If a mother is in severe pain or emotionally upset, the oxytocin reflex may become inhibited, and her milk may suddenly stop flowing well. If she receives support, is helped to feel comfortable and lets the baby continue to breastfeed, the milk will flow again.
It is important to understand the oxytocin reflex, because it explains why the mother and baby should be kept together and why they should have skin-to-skin contact.
Oxytocin makes a mother's uterus contract after delivery and helps to reduce bleeding. The contractions can cause severe uterine pain when a baby suckles during the first few days.
Signs of an active oxytocin reflex
Mothers may notice signs that show that the oxytocin reflex is active:
- a tingling sensation in the breast before or during a feed;
- milk flowing from her breasts when she thinks of the baby or hears him crying;
- milk flowing from the other breast when the baby is suckling;
- milk flowing from the breast in streams if suckling is interrupted;
- slow deep sucks and swallowing by the baby, which show that milk is flowing into his mouth;
- uterine pain or a flow of blood from the uterus;
- thirst during a feed.
If one or more of these signs are present, the reflex is working. However, if they are not present, it does not mean that the reflex is not active. The signs may not be obvious, and the mother may not be aware of them.
Psychological effects of oxytocin
Oxytocin also has important psychological effects, and is known to affect mothering behaviour in animals. In humans, oxytocin induces a state of calm, and reduces stress (22). It may enhance feelings of affection between mother and child, and promote bonding. Pleasant forms of touch stimulate the secretion of oxytocin, and also prolactin, and skin-to-skin contact between mother and baby after delivery helps both breastfeeding and emotional bonding (23,24).
2.6. Feedback inhibitor of lactation
Milk production is also controlled in the breast by a substance called the feedback inhibitor of lactation, or FIL (a polypeptide), which is present in breast milk (25). Sometimes one breast stops making milk while the other breast continues, for example if a baby suckles only on one side. This is because of the local control of milk production independently within each breast. If milk is not removed, the inhibitor collects and stops the cells from secreting any more, helping to protect the breast from the harmful effects of being too full. If breast milk is removed the inhibitor is also removed, and secretion resumes. If the baby cannot suckle, then milk must be removed by expression.
FIL enables the amount of milk produced to be determined by how much the baby takes, and therefore by how much the baby needs. This mechanism is particularly important for ongoing close regulation after lactation is established. At this stage, prolactin is needed to enable milk secretion to take place, but it does not control the amount of milk produced.
2.7. Reflexes in the baby
The baby's reflexes are important for appropriate breastfeeding. The main reflexes are rooting, suckling and swallowing. When something touches a baby's lips or cheek, the baby turns to find the stimulus, and opens his or her mouth, putting his or her tongue down and forward. This is the rooting reflex and is present from about the 32nd week of pregnancy. When something touches a baby's palate, he or she starts to suck it. This is the sucking reflex. When the baby's mouth fills with milk, he or she swallows. This is the swallowing reflex. Preterm infants can grasp the nipple from about 28 weeks gestational age, and they can suckle and remove some milk from about 31 weeks. Coordination of suckling, swallowing and breathing appears between 32 and 35 weeks of pregnancy. Infants can only suckle for a short time at that age, but they can take supplementary feeds by cup. A majority of infants can breastfeed fully at a gestational age of 36 weeks (26).
When supporting a mother and baby to initiate and establish exclusive breastfeeding, it is important to know about these reflexes, as their level of maturation will guide whether an infant can breastfeed directly or temporarily requires another feeding method.
2.8. How a baby attaches and suckles at the breast
To stimulate the nipple and remove milk from the breast, and to ensure an adequate supply and a good flow of milk, a baby needs to be well attached so that he or she can suckle effectively (27). Difficulties often occur because a baby does not take the breast into his or her mouth properly, and so cannot suckle effectively.
Good attachment
Figure 6 shows how a baby takes the breast into his or her mouth to suckle effectively. This baby is well attached to the breast.

FIGURE 6
Good attachment – inside the infant's mouth.
The points to notice are:
- much of the areola and the tissues underneath it, including the larger ducts, are in the baby's mouth;
- the breast is stretched out to form a long ‘teat’, but the nipple only forms about one third of the ‘teat’;
- the baby's tongue is forward over the lower gums, beneath the milk ducts (the baby's tongue is in fact cupped around the sides of the ‘teat’, but a drawing cannot show this);
- the baby is suckling from the breast, not from the nipple.
As the baby suckles, a wave passes along the tongue from front to back, pressing the teat against the hard palate, and pressing milk out of the sinuses into the baby's mouth from where he or she swallows it. The baby uses suction mainly to stretch out the breast tissue and to hold it in his or her mouth. The oxytocin reflex makes the breast milk flow along the ducts, and the action of the baby's tongue presses the milk from the ducts into the baby's mouth. When a baby is well attached his mouth and tongue do not rub or traumatise the skin of the nipple and areola. Suckling is comfortable and often pleasurable for the mother. She does not feel pain.
Poor attachment
Figure 7 shows what happens in the mouth when a baby is not well attached at the breast.

FIGURE 7
Poor attachment – inside the infant's mouth.
The points to notice are:
- only the nipple is in the baby's mouth, not the underlying breast tissue or ducts;
- the baby's tongue is back inside his or her mouth, and cannot reach the ducts to press on them.
Suckling with poor attachment may be uncomfortable or painful for the mother, and may damage the skin of the nipple and areola, causing sore nipples and fissures (or “cracks”). Poor attachment is the commonest and most important cause of sore nipples (see Session 7.6), and may result in inefficient removal of milk and apparent low supply.
Signs of good and poor attachment
Figure 8 shows the four most important signs of good and poor attachment from the outside. These signs can be used to decide if a mother and baby need help.

FIGURE 8
Good and poor attachment – external signs.
The four signs of good attachment are:
- more of the areola is visible above the baby's top lip than below the lower lip;
- the baby's mouth is wide open;
- the baby's lower lip is curled outwards;
- the baby's chin is touching or almost touching the breast.
These signs show that the baby is close to the breast, and opening his or her mouth to take in plenty of breast. The areola sign shows that the baby is taking the breast and nipple from below, enabling the nipple to touch the baby's palate, and his or her tongue to reach well underneath the breast tissue, and to press on the ducts. All four signs need to be present to show that a baby is well attached. In addition, suckling should be comfortable for the mother.
The signs of poor attachment are:
- more of the areola is visible below the baby's bottom lip than above the top lip – or the amounts above and below are equal;
- the baby's mouth is not wide open;
- the baby's lower lip points forward or is turned inwards;
- the baby's chin is away from the breast.
If any one of these signs is present, or if suckling is painful or uncomfortable, attachment needs to be improved. However, when a baby is very close to the breast, it can be difficult to see what is happening to the lower lip.
Sometimes much of the areola is outside the baby's mouth, but by itself this is not a reliable sign of poor attachment. Some women have very big areolas, which cannot all be taken into the baby's mouth. If the amount of areola above and below the baby's mouth is equal, or if there is more below the lower lip, these are more reliable signs of poor attachment than the total amount outside.
2.9. Effective suckling
If a baby is well attached at the breast, then he or she can suckle effectively. Signs of effective suckling indicate that milk is flowing into the baby's mouth. The baby takes slow, deep suckles followed by a visible or audible swallow about once per second. Sometimes the baby pauses for a few seconds, allowing the ducts to fill up with milk again. When the baby starts suckling again, he or she may suckle quickly a few times, stimulating milk flow, and then the slow deep suckles begin. The baby's cheeks remain rounded during the feed.
Towards the end of a feed, suckling usually slows down, with fewer deep suckles and longer pauses between them. This is the time when the volume of milk is less, but as it is fat-rich hindmilk, it is important for the feed to continue. When the baby is satisfied, he or she usually releases the breast spontaneously. The nipple may look stretched out for a second or two, but it quickly returns to its resting form.
Signs of ineffective suckling
A baby who is poorly attached is likely to suckle ineffectively. He or she may suckle quickly all the time, without swallowing, and the cheeks may be drawn in as he or she suckles showing that milk is not flowing well into the baby's mouth. When the baby stops feeding, the nipple may stay stretched out, and look squashed from side to side, with a pressure line across the tip, showing that the nipple is being damaged by incorrect suction.
Consequences of ineffective suckling
When a baby suckles ineffectively, transfer of milk from mother to baby is inefficient. As a result:
- the breast may become engorged, or may develop a blocked duct or mastitis because not enough milk is removed;
- the baby's intake of breast milk may be insufficient, resulting in poor weight gain;
- the baby may pull away from the breast out of frustration and refuse to feed;
- the baby may be very hungry and continue suckling for a long time, or feed very often;
- the breasts may be over-stimulated by too much suckling, resulting in oversupply of milk.
These difficulties are discussed further in Session 7.
2.10. Causes of poor attachment
Use of a feeding bottle before breastfeeding is well established can cause poor attachment, because the mechanism of suckling with a bottle is different. Functional difficulties such as flat and inverted nipples, or a very small or weak infant, are also causes of poor attachment. However, the most important causes are inexperience of the mother and lack of skilled help from the health workers who attend her. Many mothers need skilled help in the early days to ensure that the baby attaches well and can suckle effectively. Health workers need to have the necessary skills to give this help.
2.11. Positioning the mother and baby for good attachment
To be well attached at the breast, a baby and his or her mother need to be appropriately positioned. There are several different positions for them both, but some key points need to be followed in any position.
Position of the mother
The mother can be sitting or lying down (see Figure 9), or standing, if she wishes. However, she needs to be relaxed and comfortable, and without strain, particularly of her back. If she is sitting, her back needs to be supported, and she should be able to hold the baby at her breast without leaning forward.

FIGURE 9
Baby well positioned at the breast.
Position of the baby
The baby can breastfeed in several different positions in relation to the mother: across her chest and abdomen, under her arm (See Figure 16 in Session 6), or alongside her body.
Whatever the position of the mother, and the baby's general position in relation to her, there are four key points about the position of the baby's body that are important to observe.
- The baby's body should be straight, not bent or twisted. The baby's head can be slightly extended at the neck, which helps his or her chin to be close in to the breast.
- He or she should be facing the breast. The nipples usually point slightly downwards, so the baby should not be flat against the mother's chest or abdomen, but turned slightly on his or her back able to see the mother's face.
- The baby's body should be close to the mother which enables the baby to be close to the breast, and to take a large mouthful.
- His or her whole body should be supported. The baby may be supported on the bed or a pillow, or the mother's lap or arm. She should not support only the baby's head and neck. She should not grasp the baby's bottom, as this can pull him or her too far out to the side, and make it difficult for the baby to get his or her chin and tongue under the areola.
These points about positioning are especially important for young infants during the first two months of life. (See also Feeding History Job Aid, 0–6 months, in Session 5.)
2.12. Breastfeeding pattern
To ensure adequate milk production and flow for 6 months of exclusive breastfeeding, a baby needs to feed as often and for as long as he or she wants, both day and night (28). This is called demand feeding, unrestricted feeding, or baby-led feeding.
Babies feed with different frequencies, and take different amounts of milk at each feed. The 24-hour intake of milk varies between mother-infant pairs from 440–1220 ml, averaging about 800 ml per day throughout the first 6 months (29). Infants who are feeding on demand according to their appetite obtain what they need for satisfactory growth. They do not empty the breast, but remove only 63–72% of available milk. More milk can always be removed, showing that the infant stops feeding because of satiety, not because the breast is empty. However, breasts seem to vary in their capacity for storing milk. Infants of women with low storage capacity may need to feed more often to remove the milk and ensure adequate daily intake and production (30).
It is thus important not to restrict the duration or the frequency of feeds – provided the baby is well attached to the breast. Nipple damage is caused by poor attachment and not by prolonged feeds. The mother learns to respond to her baby's cues of hunger and readiness to feed, such as restlessness, rooting (searching) with his mouth, or sucking hands, before the baby starts to cry. The baby should be allowed to continue suckling on the breast until he or she spontaneously releases the nipple. After a short rest, the baby can be offered the other side, which he or she may or may not want.
If a baby stays on the breast for a very long time (more than one half hour for every feed) or if he or she wants to feed very often (more often than every 1–1½ hours each time) then the baby's attachment needs to be checked and improved. Prolonged, frequent feeds can be a sign of ineffective suckling and inefficient transfer of milk to the baby. This is usually due to poor attachment, which may also lead to sore nipples. If the attachment is improved, transfer of milk becomes more efficient, and the feeds may become shorter or less frequent. At the same time, the risk of nipple damage is reduced.
References
- 1.
- WHO. Infant feeding: the physiological basis. Bulletin of the World Health Organization. 1989;67(Suppl.):1–107. [PMC free article: PMC2491197] [PubMed: 2702124]
- 2.
- Lawrence RA, Lawrence RM. Breastfeeding: a guide for the medical profession. 6th Edition. London: Mosby; 2005.
- 3.
- Schanler R, guest editor. Preface. The Pediatric Clinics of North America. 2001;48(1):xix–xx.
- 4.
- Riordan J. Breastfeeding and human lactation. Boston, USA: Jones and Bartlett; 2004. The biological specificity of breast milk.
- 5.
- Butte N, Lopez-Alarcon MG, Garza C. Nutrient adequacy of exclusive breastfeeding for the term infant during the first six months of life. Geneva: World Health Organization; 2002.
- 6.
- Cernadas JMC, Carroli G, Lardizábal J. Effect of timing of cord clamping on neonatal venous hematocrit values and clinical outcome at term: a randomized, controlled trial: In reply. Pediatrics. 2006;118:1318–1319. [PubMed: 16951036]
- 7.
- Chaparro CM, et al. Effect of timing of umbilical cord clamping on iron status in Mexican infants: a randomised controlled trial. Lancet. 2006;367:1997–2004. [PubMed: 16782490]
- 8.
- Hanson LA. Immunobiology of human milk: how breastfeeding protects babies. Texas, USA: Pharmasoft Publishing; 2004.
- 9.
- Hamosh M. Digestion in the newborn. Clinics in Perinatology: Neonatal Gastroenterology. 1996;23(2):191–208. [PubMed: 8780901]
- 10.
- Sheard N. The role of breast milk in the development of the gastrointestinal tract. Nutrition Reviews. 1988;48(1):1–8. [PubMed: 3277089]
- 11.
- Innis SM. Human milk: maternal dietary lipids and infant development. The Proceedings of the Nutrition Society. 2007;66(3):397–404. [PubMed: 17637092]
- 12.
- Casey C, et al. Nutrient intake by breastfed infants during the first five days after birth. American Journal of Diseases of Childhood. 1986;140:933–936. [PubMed: 3740001]
- 13.
- WHO. Home-modified animal milk for replacement feeding: is it feasible and safe? Discussion paper prepared for “HIV and infant feeding Technical Consultation”. Geneva: World Health Organization; Oct 25–27, 2006. [5 November 2008]. 2006. http://www
.who.int/child _adolescent_health /documents/a91064/en/ - 14.
- WHO. Guiding principles for feeding non-breastfed children 6–24 months of age. Geneva: World Health Organization; 2005.
- 15.
- Forsythe S. Enterobacter sakasakii and other bacteria in powdered infant milk formula. Maternal and Child Nutrition. 2005;1:44–50. [PMC free article: PMC6874386] [PubMed: 16881878]
- 16.
- Setchell K, et al. Exposure to phyto-oestrogens from soy-based formula. Lancet. 1997;350:23–27. [PubMed: 9217716]
- 17.
- WHO. Breastfeeding counselling: a training course. Trainer's guide (Session 3: How breastfeeding works); and Overhead figures (Figure 3/1). Geneva: World Health Organization; 1993. (WHO/CDR/93.4 and WHO/CDR/93.6)
- 18.
- Edgar A. Anatomy of a working breast. New Beginnings. 2005 March–April [La Leche League International]
- 19.
- Hartmann PE, et al. Breast development and the control of milk synthesis. Food and Nutrition Bulletin. 1996;17(4):292–302.
- 20.
- Glasier A, McNeilly AS, Howie PW. The prolactin response to suckling. Clinical Endocrinology. 1984;21:109–116. [PubMed: 6467637]
- 21.
- Ramsay DT, et al. Ultrasound imaging of milk ejection in the breast of lactating women. Pediatrics. 2004;113:361–367. [PubMed: 14754950]
- 22.
- Uvnas Moberg K. The neuroendocrinology of the mother-child interaction. Trends in Endocrinology and Metabolism. 1996;7:126–131. [PubMed: 18406738]
- 23.
- Klaus M. Mother and infant: early emotional ties. Pediatrics. 1998;102(5):1244–46. [PubMed: 9794962]
- 24.
- Moore ER, Anderson GC, Bergman N. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database of Systematic Reviews. 2007;(2) [PubMed: 17636727]
- 25.
- Wilde CJ, Prentice A, Peaker M. Breastfeeding: matching supply and demand in human lactation. Proceedings of the Nutrition Society. 1995;54:401–406. [PubMed: 8524887]
- 26.
- Nyqvist KH, Sjoden PO, Ewald U. The development of preterm infants' breastfeeding behaviour. Early Human Development. 1999;55:247–264. [PubMed: 10463789]
- 27.
- Woolridge MW. The ‘anatomy’ of infant sucking. Midwifery. 1986;2:164–171. [PubMed: 3643397]
- 28.
- Kent J, et al. Volume and frequency of breastfeeding and fat content of breastmilk throughout the day. Pediatrics. 2006;117(3):e387–392. [PubMed: 16510619]
- 29.
- Dewey K, Lonnerdal B. Milk and nutrient intake of breastfed infants from 1–6 months: relation to growth and fatness. Journal of Pediatric Gastroenterology and Nutrition. 1983;2:497–506. [PubMed: 6620057]
- 30.
- Daly Hartmann PE, et al. Breast development and the control of milk synthesis. Food and Nutrition Bulletin. 1996;17:292–302.
- Breast-milk composition
- Colostrum and mature milk
- Animal milks and infant formula
- Anatomy of the breast
- Hormonal control of milk production
- Feedback inhibitor of lactation
- Reflexes in the baby
- How a baby attaches and suckles at the breast
- Effective suckling
- Causes of poor attachment
- Positioning the mother and baby for good attachment
- Breastfeeding pattern
- References
- The physiological basis of breastfeeding - Infant and Young Child FeedingThe physiological basis of breastfeeding - Infant and Young Child Feeding
- Gm12333 predicted gene 12333 [Mus musculus]Gm12333 predicted gene 12333 [Mus musculus]Gene ID:105244611Gene
- MIR7515HG MIR7515 host gene [Homo sapiens]MIR7515HG MIR7515 host gene [Homo sapiens]Gene ID:102800314Gene
- ftsI [Yersinia pestis CO92]ftsI [Yersinia pestis CO92]Gene ID:1173393Gene
- GEMIN8P4 gem nuclear organelle associated protein 8 pseudogene 4 [Homo sapiens]GEMIN8P4 gem nuclear organelle associated protein 8 pseudogene 4 [Homo sapiens]Gene ID:492303Gene
Your browsing activity is empty.
Activity recording is turned off.
See more...