Introduction
Rural hospitals1 are a critical source of health care for the 50 million Americans that reside in rural areas. These roughly 2,000 hospitals—about 40 percent of community hospitals in the U.S.2—face a host of challenges in providing quality care to the rural population. The rural population is, on average, older, less wealthy, more likely to be uninsured and have more health problems than the population at large.3 In addition, because many rural hospitals are publicly owned, they can be especially vulnerable to cuts in state and local budgets which occur during times of economic stress.
This Statistical Brief presents data from the Healthcare Cost and Utilization Project (HCUP) on rural hospital stays in 2007. Utilization, resource, and patient characteristics of these hospitalizations are presented and compared to characteristics of urban hospital stays. The most common reasons for rural hospital stays, as well as the most common reasons for rural residents’ stays in urban hospitals are provided. Similarly, the most common procedures performed during rural hospital stays, as well as during rural residents’ stays in urban hospitals are provided. Differences between estimates noted in the text are statistically significant at the 0.05 level or better.
Findings
Highlights
- Rural hospitals were typically smaller than urban hospitals: half of rural hospitals had fewer than 50 beds while only one-fifth of urban hospitals were this small.
- Hospitalizations in rural hospitals accounted for 12.8 percent of all hospitalizations and 9.6 percent of aggregate hospital costs in 2007.
- On average, costs per stay in rural hospitals were less than those in urban hospitals (respective costs of $6,500 and $9,000).
- Over half (54.7 percent) of all stays in rural hospitals were by patients residing in the lowest income communities; such patients accounted for one-quarter of all stays in urban hospitals.
- Medicare accounted for the majority of aggregate costs in rural hospitals (55.7 percent); private health insurance accounted for 23.3 percent. In urban hospitals, Medicare and private health insurance accounted for 44.3 percent and 32.2 percent of aggregate costs, respectively.
- Although most hospitalizations for rural residents took place in rural hospitals, 33 percent took place in urban hospitals.
- Rural residents were treated more frequently in urban hospitals than in rural hospitals for some common conditions and procedures: back problems (63 percent), coronary artery disease (61 percent), complication of device, implant or graft (61 percent) and heart attack (56 percent), spinal fusion (78 percent), PCTA (percutaneous transluminal coronary angioplasty) (74 percent), and cardiac pacemaker-related procedures (61 percent).
Background on rural hospital characteristics
Rural hospitals were typically smaller, more likely to be publicly owned, and less likely to be teaching hospitals than were urban hospitals. Half of rural hospitals had fewer than 50 beds; only one-fifth of urban hospitals were this small. The majority of rural hospitals were private, non-profit institutions, as were the majority of urban hospitals (52.3 percent of rural hospitals, 60.5 percent of urban hospitals). Just over a third of rural hospitals were publicly owned, in contrast to only 12.6 percent of urban hospitals. About one-tenth of rural hospitals were private, for-profit hospitals, while about a quarter of urban hospitals were private and for-profit. The majority of rural hospitals were located in the South (36.8 percent) and the Midwest (40.2). The share of rural hospitals located in the Northeast (7.1 percent) was less than half of the share of urban hospitals located there (16.6 percent) (table 1). Only 2.7 percent of rural hospitals were teaching hospitals; Critical Access Hospitals (hospitals certified to receive cost-based reimbursement from Medicare) accounted for 50.7 percent of rural hospitals.
Table 1
Characteristics of rural and urban hospitals, 2007.
General findings on inpatient stays in rural hospitals
As shown in table 2, stays in rural hospitals accounted for 12.8 percent (5.1 million) of all U.S. hospitalizations and 9.6 percent of aggregate hospital costs in 2007. These hospitalizations were almost a day shorter than stays in urban hospitals (3.9 versus 4.7 days) and less expensive than stays in urban hospitals. On average, charges and costs per stay in rural hospitals were less than those in urban hospitals (charges of $14,400 versus $27,900 and costs of $6,500 and $9,000, respectively).
Table 2
Characteristics of hospital stays in rural hospitals compared to urban hospitals, 2007.
Rural hospital stays by patient characteristics
The characteristics of rural hospital patients differed from those of urban hospital patients in terms of age, location of patient residence, and median household income. The average age of patients discharged from rural hospitals was 51.1, about 4.5 years higher than that of patients discharged from urban hospitals (46.6 years). Patients 65 years and older accounted for 41.1 percent of stays in rural hospitals; in contrast, these patients accounted for 32.4 percent of stays in urban hospitals. Gender patterns for rural and urban hospital stays were similar: females accounted for 60.4 percent of stays in rural hospitals and 58.6 percent in urban hospitals.
In terms of location of patient residence, rural residents accounted for a dramatically larger share of stays in rural hospitals than they did in urban hospitals (94.0 versus 6.9 percent). Patients residing in the lowest income communities accounted for a larger share of discharges from rural hospitals than they did from urban hospitals (54.7 versus 25.4 percent).
Rural hospital stays by region
Figure 1 shows the distribution of rural and urban stays in each region. Greater shares of hospitalizations in the Midwest (16.5 percent) and South (15.8 percent) took place in rural hospitals than in the Northeast (7.2 percent) and West (7.8 percent). This trend follows regional population trends: greater shares of the population in the Midwest and South reside in rural areas (23.6 and 20.2 percent, respectively) than in the Northeast and West (9.7 and 10.2 percent, respectively).4
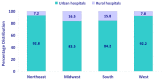
Figure 1
The share of stays in rural hospitals was greatest in the Midwest and South. Source: AHRQ, Center for Delivery, Organization, and Markets, Healthcare Cost and Utilization Project, Nationwide Inpatient Sample, 2007
Rural and urban hospital stays by payer
As shown in figure 2, Medicare paid for almost half (45.4 percent) of all stays in rural hospitals while private health insurance paid for a quarter (25.3 percent) of such stays. In contrast, Medicare and private health insurance paid for similar shares of hospitalizations in urban hospitals (35.1 and 36.2 percent, respectively). In both urban and rural hospitals, about 20 percent of stays had Medicaid as the primary payer, 5 to 6 percent of discharges were uninsured, and 3 to 4 percent of discharges were paid for by other payers.
Aggregate costs of rural and urban hospital stays by payer
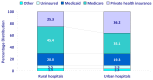
Overall, stays in rural hospitals accounted for 9.6 percent ($33.1 billion) of total aggregate costs, while stays in urban hospitals accounted for the balance ($310.4 billion). Figure 3 presents the distribution of aggregate costs by payer for rural and urban hospitals. Medicare accounted for the majority of aggregate costs in rural hospitals (55.7 percent); private health insurance accounted for 23.3 percent. In urban hospitals, Medicare accounted for a smaller share of aggregate costs (44.3 percent) and private health insurance accounted for a larger share (32.2 percent). In both urban and rural hospitals, Medicaid accounted for just under 15 percent of aggregate costs, the uninsured accounted for about 4 percent of aggregate costs, and other payers accounted for about 3 percent of aggregate costs.
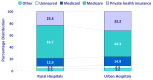
Figure 3
Medicare accounted for over half of the aggregate costs for rural hospital stays, 2007. Source: AHRQ, Center for Delivery, Organization, and Markets, Healthcare Cost and Utilization Project, Nationwide Inpatient Sample, 2007
Top principal diagnoses and principal procedures among stays in rural hospitals
In general, the most common principal diagnoses and principal procedures among rural hospital stays were similar to those among urban hospitals stays. There was some variation in the rankings of the diagnoses and procedures between the two types of hospitals.
As shown in table 3, the three most common conditions in rural hospitals—newborn infant, pneumonia, and congestive heart failure—were among the most common conditions in urban hospitals, as well. Other common diagnoses in rural hospitals—such as chronic obstructive lung disease and fluid and electrolyte disorders—were not as common in urban hospitals. Chronic obstructive lung disease was the fourth most common reason for a stay in a rural hospital (2.9 percent of rural hospital discharges), but ranked seventeenth among reasons for stays in urban hospitals (1.3 percent of urban hospital discharges). Fluid and electrolyte disorders (primarily dehydration or fluid overload) was the sixth most common reason for a rural hospitalization, accounting for 2.1 percent of these stays, but was not among the top twenty principal diagnoses in urban hospitals.
Table 3
Top 20 principal diagnoses among stays in rural hospitals, 2007.
Three diagnoses which were among the top twenty in urban hospitals did not rank among the top twenty in rural hospitals. These were back problems (disorders of intervertebral discs and bones in the spinal column), complication of device, implant or graft, and complications of surgical procedures or medical care (data not shown).
Table 4 shows the top 20 principal procedures performed during stays in rural hospitals. The two most frequent procedures performed in rural hospitals—circumcision and cesarean section—were also the two most frequent procedures performed in urban hospitals. Seventeen of the twenty most frequently performed procedures in rural hospitals were among the most frequent in urban hospitals as well. The rankings on some procedures differed between the two types of hospitals. For example, PTCA (percutaneous transluminal coronary angioplasty, procedure involving use of a balloon-tipped catheter to enlarge a narrowed artery) was rank 15 for rural hospitals but rank 6 for urban hospitals.
Table 4
Top 20 principal procedures among stays in rural hospitals, 2007.
Stays for rural residents in urban hospitals
Although rural residents are generally hospitalized in rural hospitals, one-third of their hospital stays were in urban hospitals. Rural residents were treated more frequently in urban hospitals than in rural hospitals for some common hospital conditions and therapeutic procedures. The difference in hospital location for these stays may be due in part to the availability of more specialized resources or services at urban hospitals.
Table 5 shows the top ten conditions for which rural residents stayed in urban hospitals and the distribution of stays for these conditions by hospital location. Of the ten most common conditions for which rural patients were treated in urban hospitals, four conditions were treated more frequently in urban than in rural settings: hardening of the heart arteries and other heart disease (61.4 percent in urban hospitals), back problems (disorders of intervertebral discs and bones in the spinal column) (62.6 percent), complication of device, implant, or graft (60.9 percent), and heart attack (acute myocardial infarction) (56.4 percent).
Table 5
Top 10 principal diagnoses for hospitalizations of rural residents in urban hospitals, 2007.
Table 6 shows the top ten principal procedures performed during rural residents stays in urban hospitals, as well as the distribution of stays for these procedures by hospital location. Four of the top ten procedures were performed more frequently in urban hospitals than in rural hospitals. These included three cardiovascular procedures and one musculoskeletal—PTCA (percutaneous transluminal coronary angioplasty, procedure involving use of a balloon-tipped catheter to enlarge a narrowed artery) (73.7 percent in urban hospitals), diagnostic procedure to explore the functioning of the heart (59.2 percent), procedures related to cardiac pacemaker or cardioverter/defibrillator (60.5 percent), and spinal fusion (correction of an unstable part of the spine by joining two or more vertebrae)(78.0 percent).
Table 6
Top 10 principal procedures for hospitalizations of rural residents in urban hospitals, 2007.
Data Sources
The estimates in this Statistical Brief are based upon data from the HCUP 2007 Nationwide Inpatient Sample (NIS). Many statistics were generated from HCUPnet, a free, online query system that provides users with immediate access to the largest set of publicly available, all-payer national, regional, and State-level hospital care databases from HCUP. A supplemental source included hospital characteristics from the American Hospital Association Annual Survey of Hospitals.
Definitions
Case definition
For this report, discharges from rural hospitals were determined based on the hospital location. The classification of urban or rural hospital location uses Core Based Statistical Area (CBSA) groups based on 2000 Census data. Hospitals residing in counties with a CBSA type of metropolitan are considered urban, while hospitals with a CBSA type of micropolitan or that are outside Core-Based Statistical Areas are classified as rural.
Diagnoses, procedures, ICD-9-CM, and Clinical Classifications Software (CCS)
The principal diagnosis is that condition established after study to be chiefly responsible for the patient’s admission to the hospital. All-listed procedures include all procedures performed during the hospital stay.
ICD-9-CM is the International Classification of Diseases, Ninth Revision, Clinical Modification, which assigns numeric codes to diagnoses and procedures. There are about 13,600 ICD-9-CM diagnosis codes and 3,500 ICD-9-CM procedure codes.
CCS categorizes ICD-9-CM diagnoses into a manageable number of clinically meaningful categories.5 This “clinical grouper” makes it easier to quickly understand patterns of diagnoses and procedures.
Types of hospitals included in HCUP
HCUP is based on data from community hospitals, defined as short-term, non-Federal, general and other hospitals, excluding hospital units of other institutions (e.g., prisons). HCUP data include OB-GYN, ENT, orthopedic, cancer, pediatric, public, and academic medical hospitals. They exclude long-term care, rehabilitation, psychiatric, and alcoholism and chemical dependency hospitals, but these types of discharges are included if they are from community hospitals.
Unit of analysis
The hospital is the unit of analysis in table one. The unit of analysis in the remaining tables is hospital discharge (i.e., the hospital stay), not a person or patient. This means that a person who is admitted to the hospital multiple times in one year will be counted each time as a separate “discharge” from the hospital.
Costs and charges
Total hospital charges were converted to costs using HCUP Cost-to-Charge Ratios based on hospital accounting reports from the Centers for Medicare and Medicaid Services (CMS). Costs will tend to reflect the actual costs of production, while charges represent what the hospital billed for the case. For each hospital, a hospital-wide cost-to-charge ratio is used because detailed charges are not available across all HCUP States. Hospital charges reflect the amount the hospital charged for the entire hospital stay and does not include professional (physician) fees. For the purposes of this Statistical Brief, costs are reported to the nearest hundred.
Median income of the patient’s ZIP Code
Median community-level income is the median household income of the patient’s ZIP Code of residence. The cut-offs for the quartile designation are determined using ZIP Code demographic data obtained from Claritas. The income quartile value is missing for homeless and foreign patients. In 2007, the lowest income quartile ranged from $1–$38,999, while the highest income quartile was defined as $63,000 or above.
Place of residence
Place of residence is based on the urban-rural classification scheme for U.S. counties developed by the National Center for Health Statistics (NCHS). For this Statistical Brief, we collapsed the NCHS categories into either urban or rural according to the following:
Urban:
- –
Large central metropolitan includes metropolitan areas with 1 million or more residents.
- –
Large fringe metropolitan includes counties of metropolitan areas with 1 million or more residents.
- –
Median and small metropolitan includes areas with 50,000 to 999,999 population
Rural:
- –
Micropolitan and noncore includes nonmetropolitan counties, i.e., counties with no town greater than 50,000 residents.
Region
Region is one of the four regions defined by the U.S. Census Bureau:
- –
Northeast: Maine, New Hampshire, Vermont, Massachusetts, Rhode Island, Connecticut, New York, New Jersey, and Pennsylvania
- –
Midwest: Ohio, Indiana, Illinois, Michigan, Wisconsin, Minnesota, Iowa, Missouri, North Dakota, South Dakota, Nebraska, and Kansas
- –
South: Delaware, Maryland, District of Columbia, Virginia, West Virginia, North Carolina, South Carolina, Georgia, Florida, Kentucky, Tennessee, Alabama, Mississippi, Arkansas, Louisiana, Oklahoma, and Texas
- –
West: Montana, Idaho, Wyoming, Colorado, New Mexico, Arizona, Utah, Nevada, Washington, Oregon, California, Alaska, and Hawaii
Payer
Payer is the expected primary payer for the hospital stay. To make coding uniform across all HCUP data sources, payer combines detailed categories into more general groups:
- –
Medicare includes fee-for-service and managed care Medicare patients.
- –
Medicaid includes fee-for-service and managed care Medicaid patients. Patients covered by the Children’s Health Insurance Program (CHIP) may be included here. Because most state data do not identify CHIP patients specifically, it is not possible to present this information separately.
- –
Private insurance includes Blue Cross, commercial carriers, and private HMOs and PPOs.
- –
Other includes Worker’s Compensation, TRICARE/CHAMPUS, CHAMPVA, Title V, and other government programs.
- –
Uninsured includes an insurance status of “self-pay” and “no charge.”
When more than one payer is listed for a hospital discharge, the first-listed payer is used.
For More Information
For more information about HCUP, visit http://www.hcup-us.ahrq.gov.
For additional HCUP statistics, visit HCUPnet, our interactive query system, at http://hcupnet.ahrq.gov/. For statistics on specific types of hospitals, including rural hospitals, visit Hospitals Like Mine, also available on HCUPnet.
For information on other hospitalizations in the U.S., download HCUP Facts and Figures: Statistics on Hospital-Based Care in the United States in 2006, located at http://www.hcup-us.ahrq.gov/reports.jsp.
For a detailed description of HCUP, more information on the design of the NIS, and methods to calculate estimates, please refer to the following publications:
Steiner, C., Elixhauser, A., Schnaier, J. The Healthcare Cost and Utilization Project: An Overview. Effective Clinical Practice 5(3):143–51, 2002.
Introduction to the HCUP Nationwide Inpatient Sample, 2007. Online. June 14, 2009. U.S. Agency for Healthcare Research and Quality. http://www.hcup-us.ahrq.gov/db/nation/nis/2007NIS_INTRODUCTION.pdf.
Footnotes
- 1
Throughout this Brief, the term rural refers to non-metropolitan counties and urban refers to metropolitan counties. See Definitions section for further detail.
- 2
American Hospital Association. AHA Hospital Statistics. 2008. Chicago, IL: Health Forum.
- 3
Institute of Medicine. Quality Through Collaboration: The Future of Rural Health Care. Washington, D.C.; National Academy Press, 2005.
- 4
Claritas population data, 2007.
- 5
HCUP CCS. Healthcare Cost and Utilization Project (HCUP). May 2008. U.S. Agency for Healthcare Research and Quality, Rockville, MD. www
.hcup-us.ahrq.gov /toolssoftware/ccs/ccs.jsp.
About the NIS
The HCUP Nationwide Inpatient Sample (NIS) is a nationwide database of hospital inpatient stays. The NIS is nationally representative of all community hospitals (i.e., short-term, non-Federal, non-rehabilitation hospitals). The NIS is a sample of hospitals and includes all patients from each hospital, regardless of payer. It is drawn from a sampling frame that contains hospitals comprising about 90 percent of all discharges in the United States. The vast size of the NIS allows the study of topics at both the national and regional levels for specific subgroups of patients. In addition, NIS data are standardized across years to facilitate ease of use.
About HCUPnet
HCUPnet is an online query system that offers instant access to the largest set of all-payer health care databases that are publicly available. HCUPnet has an easy step-by-step query system, allowing for tables and graphs to be generated on national and regional statistics, as well as trends for community hospitals in the U.S. HCUPnet generates statistics using data from HCUP’s Nationwide Inpatient Sample (NIS), the Kids’ Inpatient Database (KID), the State Inpatient Databases (SID), and the State Emergency Department Databases (SEDD).
Suggested Citation
Stranges, E. (Thomson Reuters), Holmquist, L. (Thomson Reuters) and Andrews, R.M. (AHRQ). Inpatient Stays in Rural Hospitals, 2007. HCUP Statistical Brief #85. January 2010. Agency for Healthcare Research and Quality, Rockville, MD. http://www
.hcup-us.ahrq .gov/reports/statbriefs/sb85.pdf.
- Review Hospital Burden of Opioid-Related Inpatient Stays: Metropolitan and Rural Hospitals, 2016.[Healthcare Cost and Utilizatio...]Review Hospital Burden of Opioid-Related Inpatient Stays: Metropolitan and Rural Hospitals, 2016.Owens PL, Weiss AJ, Barrett ML. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. 2006 Feb
- Review Overview of Hospital Stays Among Children and Adolescents, 2019.[Healthcare Cost and Utilizatio...]Review Overview of Hospital Stays Among Children and Adolescents, 2019.Weiss AJ, Liang L, Martin K. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. 2006 Feb
- Review Hospitalizations in which Patients Leave the Hospital against Medical Advice (AMA), 2007.[Healthcare Cost and Utilizatio...]Review Hospitalizations in which Patients Leave the Hospital against Medical Advice (AMA), 2007.Stranges E, Wier L, Merrill CT, Steiner C. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. 2006 Feb
- Review Health System Affiliation and Characteristics of Inpatient Stays at Rural and Metropolitan Hospitals, 2016.[Healthcare Cost and Utilizatio...]Review Health System Affiliation and Characteristics of Inpatient Stays at Rural and Metropolitan Hospitals, 2016.Karaca Z, Fingar KR. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. 2006 Feb
- Review Hospital Stays for Prostate Cancer, 2004.[Healthcare Cost and Utilizatio...]Review Hospital Stays for Prostate Cancer, 2004.Milenkovic M, Russo CA, Elixhauser A. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. 2006 Feb
- Inpatient Stays in Rural Hospitals, 2007 - Healthcare Cost and Utilization Proje...Inpatient Stays in Rural Hospitals, 2007 - Healthcare Cost and Utilization Project (HCUP) Statistical Briefs
Your browsing activity is empty.
Activity recording is turned off.
See more...