All rights reserved. Publications of the World Health Organization can be obtained from WHO Press, World Health Organization, 20 Avenue Appia, 1211 Geneva 27, Switzerland (tel.: +41 22 791 3264; fax: +41 22 791 4857; e-mail: tni.ohw@sredrokoob). Requests for permission to reproduce or translate WHO publications - whether for sale or for noncommercial distribution - should be addressed to WHO Press, at the above address (fax: +41 22 791 4806; email: tni.ohw@snoissimrep).
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Manual for the Health Care of Children in Humanitarian Emergencies. Geneva: World Health Organization; 2008.
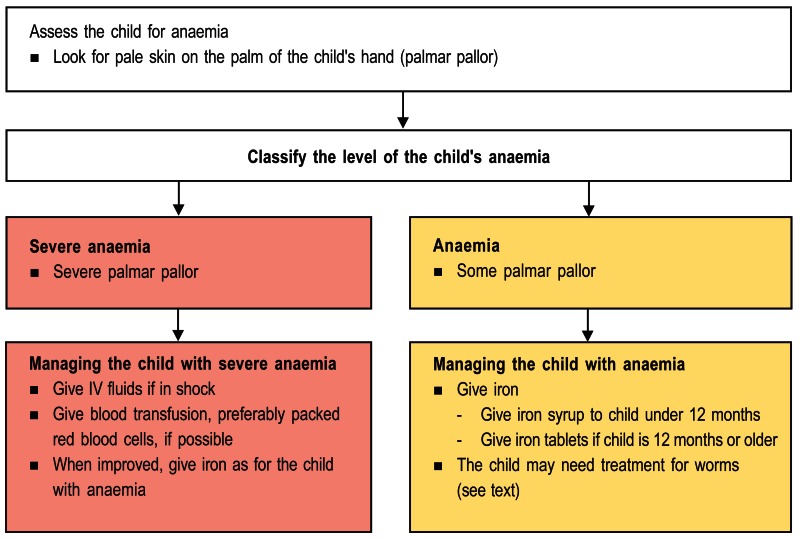
Assessment the child with anaemia
Assess the child with anaemia
- LOOK for palmar pallor (unusual paleness of the skin)
- Look at the skin of the child's palm
- Compare the colour of the child's palm with your own palm and with the palms of other children.
- If the skin of the child's palm is pale, the child has some palmar pallor
- If the skin of the palm is very pale or so pale that it looks white, the child has severe palmar pallor.
If possible, measure the haemoglobin or packed cell volume (PCV).
Classify the child with anaemia
Classify the child with severe palmar pallor as SEVERE ANAEMIA.
- A child with severe anaemia is in danger of congestive heart failure.
Classify the child with some palmar pallor as ANAEMIA.
Management of the child with severe anaemia
This child needs:
- IV fluids if in shock (see Module 1, Chapter 2).
- Blood transfusion if possible (see below).
- When improved, the child will need iron as for the child with anemia.
Blood transfusion for severe anaemia
It is essential to ensure a safe supply of blood for transfusion. Blood should be cross-matched and screened for HIV, malaria and hepatitis B, and if possible, hepatitis C and syphilis. If a safe supply cannot be assured, transfusion should be restricted to patients with severe anaemia and signs of shock (i.e. cold hands and capillary refill > 3 seconds or weak fast pulse) or severe respiratory distress (fast breathing or chest indrawing). If suitable donors without malaria infection cannot be found, blood should be administered with antimalarial treatment.
Children with haemoglobin <5 g/dl (or packed cell volume <15%) and respiratory distress need blood as an emergency.
- Give 20 ml/kg, as packed red cells or whole blood.
- Infuse the first 10 ml/kg over 30 minutes and the next 10 ml/kg over 2 hours.
- Reassess the patient at the end of the transfusion. If the child still has respiratory distress and haemoglobin <5 g/dl, repeat the transfusion.
Children with haemoglobin <5 g/dl (or packed cell volume <15%) but without respiratory distress should be transfused but, because their condition is less critical, can be given 20 ml/kg over 3–4 hours.
- Diuretics (furosemide) are unnecessary.
Severely malnourished children (severe wasting plus oedema).
- Give blood much more cautiously to these children
- Infuse 10 ml/kg blood over 3 hours.
- Give furosemide, 1 mg/kg IV, halfway through the transfusion.
Management of the child with anaemia1
This child needs the following interventions.
- Give iron syrup to the child under 12 months of age.
- Give iron tablets if the child is 12 months or older.
- Give the mother enough iron for 14 days. Tell her to give her child one dose daily for the next 14 days.
- Do not give iron to a child receiving the antimalarial sulfadoxine-pyrimethamine
- The child may need treatment for malaria if the malaria risk is high.
- Only if there are worms in the area or if the hygienic situation is bad give the child mebendazole or albendazole. Only give mebendazole if the child with anaemia is 1 year of age or older and has not had a dose of mebendazole in the last 6 months.
- As vitamin C helps iron absorption, advise the caretaker to give citrus fruits to the child.
- Advise that iron tablets may cause constipation.
- Advise the mother to return immediately with the child if the child develops any danger sign (lethargy or unconsciousness, convulsions, or inability to drink).
- Follow up in 14 days.
Footnotes
- 1
Anaemia in Mediterranean countries may be due to thalassemia or sickle cell and special attention should be given.
- Pallor/anaemia - Manual for the Health Care of Children in Humanitarian Emergenc...Pallor/anaemia - Manual for the Health Care of Children in Humanitarian Emergencies
Your browsing activity is empty.
Activity recording is turned off.
See more...